 Heart disease is usually ascribed to many different causes. Amongst these are issues relating to the blood vessels, including coronary artery disease, arrhythmias, and even congenital heart defects. According to new research, however, endothelial dysfunction may play a significant role in the development of heart conditions.
Heart disease is usually ascribed to many different causes. Amongst these are issues relating to the blood vessels, including coronary artery disease, arrhythmias, and even congenital heart defects. According to new research, however, endothelial dysfunction may play a significant role in the development of heart conditions.
Symptoms commonly associated with heart conditions include shortness of breath, chest pain, tightness, pressure, or discomfort (angina), pain or numbness in your arms or legs, and pain in the jaw, throat, neck, and back.
Common risk factors that may contribute towards the development of a heart condition include:
Heart disease, in the USA, accounts for one in four deaths each year. That makes it the cause of approximately 630,000 deaths each year in the United States alone. But while the traditional cardiovascular disease risk factors mentioned above are the primary targets for most current therapies, these risk factors only account for about fifty percent of heart-related deaths. The culprit may very well be endothelial dysfunction.
Endothelial dysfunction, according to new research, may initiate and also cause the progression of atherosclerotic cardiovascular conditions. By measuring endothelial dysfunction, we may be able to determine a person’s risk of developing cardiovascular issues. Looking forward, therapies used in ensuring heart health may stop focusing on the symptoms presented by heart conditions, and focus instead on endothelial dysfunction and accompanying atherosclerotic plaque formations.
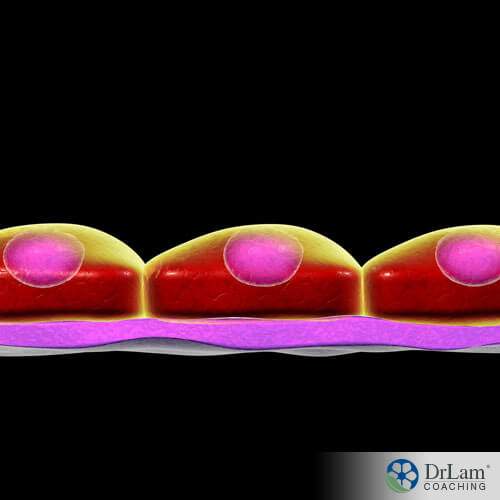
Your endothelium is a thin, single-cell layer that forms the inner lining of both your blood vessels and lymph vessels. It is a single-cell layer between the walls of your blood vessels and your blood. Your endothelium thus plays a major role in what passes between your blood and the rest of your body. The body of a human adult has approximately 60,000 miles of blood vessels.
The endothelium plays an extremely important role, not only in heart health and function, but in the function of your entire body, including your brain. It helps maintain a normal vascular tone, and thus healthy blood pressure, by releasing both relaxing and contracting factors.
The endothelium also serves as a transport barrier between the blood and the rest of your body. It allows for the passage of certain molecules while disallowing the passage of others. For example, it regulates beneficial glucose and amino acid transport.
The agents for transcellular transport in endothelial cells are known as caveolae. Caveolae also regulate nitric oxide and calcium signaling in the endothelium. Tight junctions, the intercellular junctions between two individual endothelial cells, also play a role in vascular permeability. A tight junction functions either as a gate or a fence. When functioning as a fence, no molecules are allowed to pass through. While acting as a gate, certain selected molecules may pass through. A compromised tight junction could result in compromised vascular permeability. Endothelial dysfunction may occur, resulting in pathogens spreading to various parts of the body with possible dire consequences.
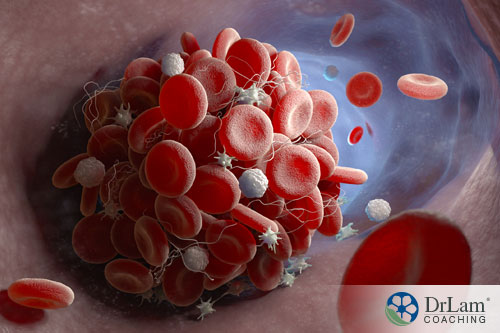 The endothelium may also have antithrombotic and fibrinolytic properties. This is because your endothelial cells can generate an antithrombotic surface, meaning plasma and other cellular contents are not able to stick to that specific area. This means that blood clots are both prevented from forming and growing.
The endothelium may also have antithrombotic and fibrinolytic properties. This is because your endothelial cells can generate an antithrombotic surface, meaning plasma and other cellular contents are not able to stick to that specific area. This means that blood clots are both prevented from forming and growing.
Another function associated with the endothelium is that it modulates the interaction between your blood vessel walls and circulating leukocytes (white blood cells) and platelets. Leucocytes play an important immune function, fighting off foreign pathogens while staving off infection. Platelets, on the other hand, play a role in clot formation in the event of injury and bleeding. Wherever an injury is sustained, platelets rush to that specific site and form a clot in order to repair the damage.
Lastly, the endothelium may have paracrine functions. This means it facilitates the secretion of substances that help with the regulation of various vascular and body functions.
Endothelial dysfunction refers to the diminished production or availability of nitric oxide (NO), as well as an imbalance in the relaxing and contracting factors released by the endothelium.
Endothelial dysfunction may result from an injury or damage to the endothelium. Common causes of endothelial dysfunction may include:
 High cortisol levels, according to research, may be a source of endothelial dysfunction. Higher cortisol levels are commonly associated with stress and are your body’s output in accordance with its NeuroEndoMetabolic (NEM) Stress Response, which starts in the brain. Your brain or more specifically the Hypothalamic-Pituitary-Adrenal (HPA) axis is the triad that is responsible for the cascade of events in the body as soon as a threat - stress - is experienced.
High cortisol levels, according to research, may be a source of endothelial dysfunction. Higher cortisol levels are commonly associated with stress and are your body’s output in accordance with its NeuroEndoMetabolic (NEM) Stress Response, which starts in the brain. Your brain or more specifically the Hypothalamic-Pituitary-Adrenal (HPA) axis is the triad that is responsible for the cascade of events in the body as soon as a threat - stress - is experienced.
Under normal circumstances, your body’s NEM returns to normal once the period of threat is over. Prolonged periods of stress, on the other hand, lead to prolonged and increased cortisol production. This results in numerous physical symptoms that may seem unrelated.
With regards to heart health, prolonged mental stress has been tied to enhanced platelet aggregation, rupture of atherosclerotic plaque, and thrombosis. These three, as noted, are tied to epithelial function. Stress has also been associated with high blood pressure and high blood sugar levels, while thrombosis could lead to a stroke. Common symptoms associated with stress include feelings of anger, anxiety, and depression, forgetfulness, lower energy levels, sleep issues, aches and pains of unknown origin, and even hormone imbalances.
When cortisol is released from the adrenals, it helps the body deal with stress, providing the nutritional substrates needed for energy production. At the same, it helps with the selection of the correct fuels needed for your heart to work optimally to meet oxygen demands. Vascular tone is also increased. This results in blood vessel constriction that increases blood flow and blood pressure. Blood sugar levels may also show an increase, readying energy for your body. There will be a decrease in insulin production. Your heart may experience strain as it works harder.
Hypertension and the risk of a cardiac episode may temporarily increase. Chronic stress can make this temporary increase long-term, and it also increases your risk for adrenal fatigue.
Besides promoting high blood sugar levels and affecting vascular tone, high cortisol levels are also associated with higher blood cholesterol levels. These are all associated with an increased risk of plaque buildup on your arteries and endothelial dysfunction.
The endothelium’s first line of defense against endothelial dysfunction is a thin, gel-like protective layer called the glycocalyx. This layer coats the side of the endothelium facing the lumen. The glycocalyx is a layer separating your blood and endothelium.
This layer has a number of functions protecting against endothelial dysfunction. It:
In short, the endothelium is safe as long as the endothelial glycocalyx layer is intact. When this layer is compromised, however, and the endothelial layer is exposed, the general picture changes drastically:

The above factors may ultimately lead to the formation of plaque that adheres to the blood vessel walls.
The endothelial glycocalyx limits access to the endothelial cells. It prevents components in your blood such as lipoproteins, sticky leukocytes, and activated platelets from having unlimited access to the endothelium. This layer also has an anti-inflammatory function as well as protecting against thrombosis. This it does this by harboring certain proteins. Amongst these are included:
If the endothelial glycocalyx is damaged, endothelial dysfunction may occur. Known causes of damage to this layer include:
High blood sugar levels are one of the major culprits in endothelial glycocalyx dysfunction, as it can virtually destroy this layer. This may result in inflammation and endothelial dysfunction. Diet thus plays a very important role in a healthy endothelial layer, because when the glycocalyx layer breaks down, the endothelial cells lose their protective shield and become vulnerable. It can take anything from six hours to several days for this layer to be rebuilt.
Interestingly, constant eating may result in blood sugar spikes that have a negative effect on this layer, while intermittent fasting may be beneficial. This is because the latter allows the body time to rebuild this layer. Diabetics may also benefit from intermittent fasting as the same scenario applies.
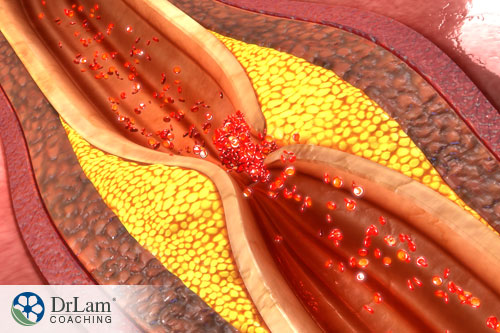 Although heart health is commonly said to depend on factors such as plaque buildup in arteries, inflammation, high cholesterol levels, and others, these factors are only detrimental to your heart health once the endothelium is compromised. Endothelial dysfunction may thus very well be the starting point of all cardiovascular disease.
Although heart health is commonly said to depend on factors such as plaque buildup in arteries, inflammation, high cholesterol levels, and others, these factors are only detrimental to your heart health once the endothelium is compromised. Endothelial dysfunction may thus very well be the starting point of all cardiovascular disease.
The endothelium’s main source of protection is the endothelial glycocalyx, but this layer also has numerous other functions in cardiovascular health. Protecting the glycocalyx layer and maintaining its health may thus be an important step in preventing cardiovascular disease.
There are currently no medications used in the traditional western healthcare sphere that directly target the endothelial glycocalyx. Instead, only symptoms of the glycocalyx and thus endothelial dysfunction are given consideration.
Prediabetes and type-2 diabetes are good examples. Here, glycemic control is initiated by means of certain medications in order to keep blood sugar levels stable. While these medications may be effective in addressing blood sugar issues, they are not addressing or supporting the real issue – a compromised glycocalyx layer and the resulting endothelial dysfunction.
There are, however, a number of natural compounds that could support the glycocalyx layer. Amongst these are:
Reducing inflammatory mediators such as cortisol, which is linked to stress and adrenal fatigue, may also support glycocalyx health and function.
A limited amount of research has been done on endothelial dysfunction and the endothelial glycocalyx. Although partly to investigate causes of endothelial dysfunction, the main aim was to determine the action of natural compounds on endothelial glycocalyx health.
When exposed to high glucose levels, the glycocalyx virtually disappears. By introducing natural compounds from polysaccharides that have a similar structure to the glycosaminoglycans which are found on the glycocalyx, you may see a marked improvement in endothelial glycocalyx structure. Certain marine-based polysaccharides have been shown to be beneficial to heart health.
A specialized, sulfated polysaccharide compound has been found to maintain and repair the glycocalyx. Plant foods are a good source of polysaccharides, and include:
 A study on mice regarding leukocyte adhesion to the endothelial layer showed that stripping this layer resulted in increased leukocyte adhesion to the endothelium. Once a natural polysaccharide compound was introduced, however, this layer was repaired and leukocyte function returned to normal.
A study on mice regarding leukocyte adhesion to the endothelial layer showed that stripping this layer resulted in increased leukocyte adhesion to the endothelium. Once a natural polysaccharide compound was introduced, however, this layer was repaired and leukocyte function returned to normal.
A study on endothelial function and arterial elasticity also had a positive outlook. Arterial elasticity is a good indication of endothelial function. When participants in the study were given a formulate polysaccharide compound, arterial elasticity was increased by almost ninety percent. This may be of particular benefit to the elderly, as high blood pressure and a decrease in blood vessel flexibility are commonly associated with the aging process.
An ongoing study on atherosclerotic plaque conducted in China showed that participants given a formulated polysaccharide product experienced a marked improvement after only two months.
It is interesting to note that arterial stenosis only makes up about half of the incidents of arterial lesion occurrence. Furthermore, approximately sixty percent of people who have had a heart attack have normal cholesterol levels. Cholesterol’s role in heart-related conditions may thus be over-exaggerated.
Plaque rupture, when the surface of plaque ruptures, may often result in thrombosis and the forming of coronary atherosclerotic lesions. It accounts for approximately 75% of thrombosis incidents that result in myocardial infarctions, or heart attacks, and up to 90% of thrombosis incidents resulting in ischemic stroke. More than 70% of ruptured coronary plaque is non-stenotic, i.e. not occurring at places where blood vessels are abnormally narrow.
When talking about vulnerable plaque, you are referring to atherosclerotic plaque that shows a rapid progression, is in danger of rupture, and which is prone to thrombosis. This type of plaque may also have a rupture of the fibrous cap or intrude into the lumen.
When a formulated polysaccharide was administered to test subjects, the response of plaque, thus far, has been exceedingly promising. Subjects with endothelial dysfunction due to plaque buildup show a significant improvement when given a formulated polysaccharide for plaque stabilization and reversal in vulnerable carotid artery plaque. Here, a significant reduction was seen in the lipid-rich necrotic core. The term ‘necrotic core’ refers to the area where plaque buildup occurs.
Furthermore, results so far suggest that using a formulated polysaccharide may be of benefit with regards to the lumen, increasing its size and thus reducing arterial stenosis. It is estimated that approximately 2.5 million US citizens over the age of 75 years have aortic stenosis (stenosis in the arteries). The current survival rate is estimated at 50% after two years from the onset of the condition, and 20% at five years unless action is taken to mitigate the situation.
Conventional medicine often makes use of statins in addressing atherosclerotic plaque issues. Statins are medications designed to lower your blood cholesterol by blocking enzyme action in the liver that is responsible for cholesterol production. Yet cholesterol is not all bad. It is essential for both normal cells and body function. High cholesterol levels are, however, linked to atherosclerosis, a condition whereby cholesterol-containing plaque builds up in your arteries and deters a healthy blood flow. Although studies indicate a significant reduction of the lipid-rich necrotic core, no stenosis reduction has been observed in any of the studies looked at thus far.
When addressing atherosclerosis, the ideal would be to not only change the lipid-rich necrotic core but to increase the lumen size while decreasing stenosis as well.
With regards to the above statement, studies using formulated polysaccharides have thus far proved promising. For example:
The above statistics that show that the use of formulated polysaccharide with regards to addressing atherosclerosis positively impacts the lipid-rich necrotic core, lumen volume, and incidence of stenosis.
 Stress and its accompanying higher-than-normal cortisol production are among the main causes of heart issues. Diet is probably just as high on the list. By addressing these two issues, you can go a long way towards assuring heart health and the elimination of endothelial dysfunction. Stress and diet are also associated with the incidence of adrenal fatigue, as are lifestyle issues such as exercise.
Stress and its accompanying higher-than-normal cortisol production are among the main causes of heart issues. Diet is probably just as high on the list. By addressing these two issues, you can go a long way towards assuring heart health and the elimination of endothelial dysfunction. Stress and diet are also associated with the incidence of adrenal fatigue, as are lifestyle issues such as exercise.
Stress may be the result of psychological, environmental, or physiological issues. While it may be difficult to remove these causes from your daily life, one could try alternative means of getting rid of them. You could move, or remove all chemical substances from your environment, or consider meditation or deep breathing exercises.
With regards to diet, there is much you can do. The first step would be to seriously limit your intake of trans fats and processed foods. Furthermore, a balanced diet is essential.
When it comes to diet, many foods contain compounds that help with heart and adrenal health. In both, keeping an eye on blood sugar levels is very important, as is ensuring your body gets the nutrients it needs for rebuilding and optimal health.
Caffeine stimulates cortisol production, putting extra stress on the adrenals while potentially negatively influencing an already overworked heart. The aim is thus to eliminate that from your diet which negatively impacts your adrenals and heart and arterial function, while at the same time opting for food choices that aid in recovery.
Whole, fresh organic fruit and vegetables are thus a better choice, while protein, complex carbohydrates, and omega-3 fatty acids should also be considered as part of a healthy, balanced diet. With regards to complex carbohydrate choices, this means changing from white pasta to whole grain pasta, for example. Good protein choices include lean beef and chicken. Good sources of omega-3 fatty acids would include cold water fatty fish such as salmon, mackerel, and herring, nuts and seeds such as walnuts and flaxseed, and plant oils like canola oil.
With regards to exercise, it not only helps address adrenal issues but promotes heart health as well. This does not, however, mean you should go out and attempt to run a marathon! In most cases of adrenal fatigue, as is the case with promoting heart health, gentle exercise is the way to go. This includes walking, pilates, and yoga. The latter two, especially, concentrate on building your core muscles while promoting flexibility.
Lastly, you should always remember to stay hydrated. This means drinking plenty of water, thereby allowing your body to heal itself. Dehydration, albeit even unknowingly, is often associated with people suffering from adrenal fatigue.
 Adrenal and heart health are closely intertwined. Although new research into addressing endothelial dysfunction is promising, you should always keep in mind that arterial and heart health is largely dependent on adrenal health. A holistic approach may thus be the best course of recovery. While addressing your heart health, remember to consider your adrenal health at the same time. The team at Dr. Lam Coaching can help. We offer a free** phone consultation at +1 (626) 571-1234 where we will privately discuss any queries you may have. You can also ask a question through our Ask The Doctor system by clicking here.
Adrenal and heart health are closely intertwined. Although new research into addressing endothelial dysfunction is promising, you should always keep in mind that arterial and heart health is largely dependent on adrenal health. A holistic approach may thus be the best course of recovery. While addressing your heart health, remember to consider your adrenal health at the same time. The team at Dr. Lam Coaching can help. We offer a free** phone consultation at +1 (626) 571-1234 where we will privately discuss any queries you may have. You can also ask a question through our Ask The Doctor system by clicking here.
Heart health and adrenal fatigue are closely related issues. Endothelial dysfunction could very well be related to adrenal function. Addressing endothelial dysfunction may need to incorporate adrenal support because high cortisol levels have an impact on both heart and adrenal conditions.
