 In the medical world, things change all the time. Research is constantly revealing new ways to address different disorders and diseases. This is true of Lyme Disease as well. This disease can cause multiple problems over both the long and short term, so it’s important that you address it early and aggressively. These new Lyme guidelines can be used as a guide to help you get back to good health once more. This is particularly important if you have Adrenal Fatigue Syndrome (AFS) or other disorders that are caused or impacted by stress.
In the medical world, things change all the time. Research is constantly revealing new ways to address different disorders and diseases. This is true of Lyme Disease as well. This disease can cause multiple problems over both the long and short term, so it’s important that you address it early and aggressively. These new Lyme guidelines can be used as a guide to help you get back to good health once more. This is particularly important if you have Adrenal Fatigue Syndrome (AFS) or other disorders that are caused or impacted by stress.
Black-legged or deer ticks carry bacteria known as Borrelia burgdorferi. The ticks are infected after they feed on other infected animals like deer, mice, or birds. When the ticks then bite humans, they pass on these bacteria, which cause Lyme disease. For the infection to be transmitted, the tick has to be on your skin for at least 36 hours. But this doesn’t mean that you’ll be aware of it. Many people who have Lyme disease don’t remember ever being bitten by a tick. That’s why this disease can go unnoticed for a long time.
Lyme disease was first identified in 1975 and is very common throughout Europe and the United States. You’re particularly at risk if you live in a wooded area or keep animals that visit wooded areas.
Lyme disease can affect both adults and children and its symptoms can vary widely. Some of the most common symptoms are:
Obviously, these symptoms can be quite vague, which is why Lyme disease is often mistaken for something else or missed completely. However, if you do get this disease, then you need to know the best ways to address it with the new Lyme guidelines.
Lyme disease isn’t easy to identify. Its symptoms can look like lots of other conditions, so sufferers often have to go through periods of uncertainty before the disease is identified. The rash is the most obvious sign of Lyme disease. However, it only appears in around 80% of cases. If you experience this uncertainty, then there may be a long delay during which you don’t benefit from the new Lyme guidelines. This will obviously hamper and delay your recovery. One of the keys to a fast recovery from Lyme disease is to start taking antibiotics as soon as possible after the bite.
To identify Lyme disease, your doctor will take a full medical history and do a physical exam. They will specifically want to know about any rashes and about your connection to areas where ticks are known to live. Make sure that you think back and give them accurate information.
After this, your doctor may recommend a few lab tests, which are more accurate a few weeks after infection once your body has developed antibodies:
There are obvious problems with this approach. The laboratory tests look for an immune response to the bacteria, not to the bacteria itself. In this way, many people who have Lyme disease receive negative blood results when they actually have the disease. It’s just that their bodies haven’t mounted a defense yet. This can lead to weeks or even months of uncertainty and fear while patients and medical professionals try to work out what’s wrong.
There are other laboratories that can test for PCR which looks at the DNA content, IgG and IgM antibody response, and antigens, but these tests are very expensive and might not change your care strategy overall.
Lyme disease can be a controversial topic, as can the new Lyme guidelines. One of the biggest issues with this disease is what’s often known as Chronic Lyme disease. This is the subject of much disagreement. Many researchers instead use the term "persistent Lyme disease" or "post-treatment Lyme disease (PTLD)" to describe people who have symptoms after their antibiotics course has ended.
Only a small proportion of people experience PTLD. Most people take the antibiotics and go on with life without any long-term complications. However, some people experience symptoms that can last for years. These symptoms are usually vague and include:

Unfortunately, most of the evidence for PTLD is anecdotal and in most cases, there is no laboratory proof that the bacteria remain in the body. This makes it hard for both medical professionals and sufferers to address. Conventional medicine seems to be helpless against PTLD, but the suffering of its victims is very real. If the pathogen load is low and escapes laboratory testing, you can be symptomatic but laboratory values are normal. This "sub-clinical" state of Lyme is thus hard to diagnose with pinpoint accuracy.
Many physicians will restart antibiotic treatment when PTLD is suspected based on clinical symptoms alone. This is controversial. The length of time that sufferers should take antibiotics is a particular point of contention, and until recently there was no consensus. This is one of the issues that the new Lyme guidelines is attempting to correct.
It is still unclear whether these clearer guidelines will help people with PTLD. Some anecdotal evidence shows improvement in PTLD cases after months of antibiotics. But there are no studies at this stage to support taking antibiotics for such a long duration. And there are obvious problems with this approach, as antibiotics are powerful medications that can have dangerous side effects.
If you believe that you have PTLD, then you must still be tested for Lyme disease just in case. If it’s present, then your doctor will probably follow the new Lyme guidelines and give you antibiotics. However, if you finish an antibiotic course and still have symptoms even though your lab tests are clear, then you may be presumed to have PTLD.
If this occurs then your doctor may also want to test other parts of your body to determine if there is any long-term damage present. These tests can include:
If these tests don’t show anything, then you will have to try other strategies to find relief. Here’s what to do:
There are also other alternative natural remedies that may help support the body is its fight against PTLD. These include:
There is no evidence that supplements can help address or eliminate Lyme disease. However, you can supplement to improve your immune system overall, which will have beneficial effects on your health. Some of the best supplements for detoxification and immune health are:

Certain essential oils such as clove bud, oregano, and cinnamon bark have demonstrated anti-pathogenic activities in lab settings. Since oral ingestion is not recommended except in exceptional situations, instead try using certain essential oils topically or via inhalation to help reduce specific symptoms such as:
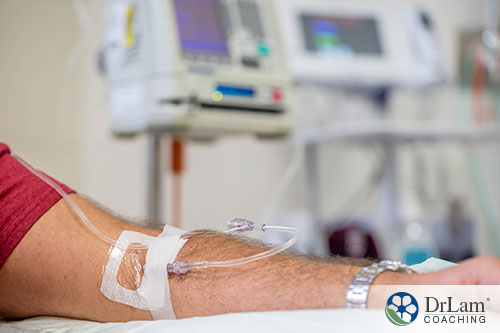
Other forward-looking strategies include the deployment of medical ozone, hyperbaric oxygen, cellular photo modulation by intravenous laser, methylene blue, and molecular hydrogen.
Chelation therapy uses medications that bind to metals in the bloodstream, creating a compound that can be excreted by your kidneys. This therapy is popular among PTLD sufferers who believe Lyme disease is linked to heavy metal toxicity in the body. Chelation therapy is effective in removing these metals, although there’s no evidence that PTLD is linked to metal toxicity directly.
You may also want to try a diet that’s designed to help address Lyme disease. There are several available at the moment, most of them with the goal of strengthening the immune system and reducing stress. Most of these diets are based on eating healthy fruits and vegetables, avoiding sugars and processed foods, and reducing foods that cause inflammation.
Low dose immunotherapy (LDI) is a therapy that teaches your immune system to tolerate Lyme antigens that have been diluted to homeopathic doses. By exposing your white cells to the bio-resonance and energy of the antigens in very minute amounts, you can help educate your immune cells to not overreact to the Lyme that could still be hidden deep within your cells.
 This type of immunotherapy doesn't necessarily "get rid" of Lyme, but it improves your ability to tolerate it in your own body. This can be a game-changer for some. It is very effective for very weak sufferers such as those with advanced adrenal fatigue who can't tolerate Lyme therapies or even supplements due to their body's congestion and sensitivities. Ask your doctor about LDI as it does have to come from an experienced practitioner. Allot 3-12 months to see results.
This type of immunotherapy doesn't necessarily "get rid" of Lyme, but it improves your ability to tolerate it in your own body. This can be a game-changer for some. It is very effective for very weak sufferers such as those with advanced adrenal fatigue who can't tolerate Lyme therapies or even supplements due to their body's congestion and sensitivities. Ask your doctor about LDI as it does have to come from an experienced practitioner. Allot 3-12 months to see results.
It’s very important that you talk to your doctor before you try any of these strategies. Some are fairly harmless. However, there are also other alternative remedies out there that may be outright harmful to your body. Never try any alternative remedies for Lyme disease without the support and assistance of a medical professional.
Adrenal Fatigue Syndrome (AFS) occurs when you’re under chronic stress over a long period and your NeuroEndoMetabolic (NEM) Stress Response becomes overused and unbalanced. The NEM stress response makes changes in your body’s organs and systems - circuits - in response to stress. These changes protect your body against being harmed by the stress and give you the energy to respond to the cause of the stress.
Cortisol is one of the primary means by which the NEM stress response makes these changes. It’s a hormone that’s excreted from the adrenals. In small doses, when it’s needed, cortisol is very beneficial and even essential to your body’s functions. But when you’re chronically stressed, it can cause the circuits and their individual components to become unbalanced. The high ongoing demand for cortisol can also fatigue the adrenals and cause them to start breaking down, which is characteristic of adrenal fatigue.
Lyme disease is an obvious cause of stress. It brings on symptoms that are very similar to AFS symptoms such as fatigue, brain fog, aches and pains, and symptoms of infection. If you already have AFS and become infected with Lyme disease, then you may find your symptoms worsening.
If you’re otherwise healthy but contract Lyme disease, then the resulting stress and poor health may bring on AFS, especially if you experience long-term symptoms. That’s why it’s incredibly important to pay attention to the new Lyme guidelines and give your body the best possible chance of a fast and full recovery.
Lyme disease can have devastating effects on the body’s Inflammation circuit, which includes the immune system, the gut, and the microbiome. When you have AFS, this circuit goes into overdrive. The immune system creates inflammation in order to drive out infections and stress which both negatively affect your body’s microbiome, your bacterial balance. This can cause more ongoing infections and gut problems as the balance shifts towards bad gut bacteria, causing constipation, diarrhea, and other gut issues.
If you contract Lyme disease, it could seriously complicate these issues. If you already have AFS, then the immune system malfunctions will make you more likely to contract Lyme disease. As the immune system declines in health, your body will struggle to fight off the Lyme disease, which will put you at a higher risk of experiencing chronic issues. The ongoing issues will cause more inflammation, which will further unbalance your gut and microbiome because of the interconnectedness of the components of this circuit. This will cause more symptoms and problems and further increase your stress levels.
The end result may be increased inflammation and stress, which will increase the demand for cortisol. And this will, of course, worsen AFS.
If you don’t have AFS but you’re chronically stressed, then Lyme disease could be the prompt that brings on adrenal fatigue. The symptoms associated with this disease can be difficult to manage and identify. If your symptoms aren’t all that severe, you may even delay going to see your doctor, which means that you won’t know to implement the new Lyme guidelines. This delay will only slow down your recovery, put you at a higher risk of chronic problems, and increase your stress levels. And this will put you at more risk of developing AFS.
If you have Lyme disease, then it’s important that you talk to your doctor about the new Lyme guidelines, especially if you also suffer from AFS. There are several alternative remedies available, but none of them have shown any beneficial effects under research conditions. In some cases, these alternative options can even be harmful, so make sure you get the advice of a trained medical professional first.
The new Lyme guidelines are based on the latest research on Lyme disease. They recommend:
 If you’re bitten by a high-risk tick, then you should take prophylactic antibiotics within 72 hours of removing the tick. A high-risk tick is:
If you’re bitten by a high-risk tick, then you should take prophylactic antibiotics within 72 hours of removing the tick. A high-risk tick is:
If you have the characteristic spreading rash associated with Lyme disease, then you should take 10 days of doxycycline or 14 days of an antibiotic such as amoxicillin, phenoxymethylpenicillin, or cefuroxime axetil.
Lyme is recognized to be associated with psychiatric disorders. The new Lyme guidelines suggest doctors perform Lyme testing for patients who could have been exposed to high-risk ticks and present with:
However, testing is not recommended for patients with other psychiatric illnesses or neurological syndromes.
Evidence suggests that children with behavioral, developmental, or psychiatric disorders should not be tested for Lyme disease.
The research suggests that patients who experience chronic symptoms should not be given additional antibiotics if they don’t have evidence of reinfection or failure of the first antibiotic course. There is additional information in the new Lyme guidelines on how to evaluate patients with chronic symptoms associated with Lyme disease. A lot of people who have been on multiple courses of antibiotics to try to combat Lyme end up developing severe comorbidities from overuse of antibiotics rather than from the actual Lyme disease.
Previous measures to address Lyme disease were not so clear and often differed from person to person and doctor to doctor. In fact, this is probably the primary purpose of the new Lyme guidelines - to clear up any confusion and introduce a basic standard of care. The biggest differences between the old guidelines and the new are:
The new Lyme guidelines state that antibiotics should be given to people who have been bitten by a high-risk tick for 14 days. The previous guidelines were not nearly as clear and antibiotics were often given for varying lengths of time.
The new Lyme guidelines claim that antibiotics should not be given in cases where symptoms persist after antibiotic therapy. Previously, sufferers were given another, longer dose of antibiotics.
You will need to be very careful when following the new Lyme guidelines when you have AFS. Antibiotics are powerful medications even when you’re healthy, and when you have AFS, they can have significant negative effects on your body including:
When you have AFS, your body is in a heightened state. Your immune system will be overactive and more prone to overreacting to medications. This may cause an allergic reaction to antibiotics, which will make your condition much worse. It will also further unbalance your Inflammation circuit, which will worsen your underlying AFS.
Some of the most common side effects of antibiotics are vomiting, nausea, diarrhea, and abdominal bloating. These issues will further impact your gut health, which may already be poor in AFS because of Inflammation circuit imbalances.
Antibiotics work by killing off bacteria, both good and bad. If AFS has already unbalanced your microbiome, this is the last thing you want. Antibiotics could worsen any problems that you’re already experiencing because of imbalances in your microbiome such as increased infections. And a microbiome imbalance will also further impact the Inflammation Circuit, worsening your AFS.
Despite all of this, you shouldn’t ignore your doctor’s advice about taking antibiotics. Lyme disease is a serious disorder that can have long-term consequences if it isn’t addressed as quickly as possible. Instead, make sure that your doctor is aware of your AFS and the potential consequences of taking antibiotics and decide together what the best option is for your body and health.
Lyme disease can be a long-term problem that causes uncomfortable symptoms and worsens stress. This can be very dangerous if you have AFS or if you’re already close to adrenal fatigue. Using the new Lyme guidelines, here’s what to do if you are infected with this disease:
If you’re struggling with PTLD, a stronger body is always conducive to the healing process. For natural support, get help from our nutritional team by clicking here for our Ask The Doctor system or giving us a call on (626) 571 1234.
© Copyright 2021 Michael Lam, M.D. All Rights Reserved.
The new Lyme guidelines recommend changes such as reducing the length of extended antibiotic use if Lyme disease symptoms persist, and suggest additional testing for problems in other organs if certain symptoms occur. Because research is always giving new and more clear information on how to address these issues, it is important to always follow the most up-to-date guidelines.
