Your intestines contain approximately 40 to 100 trillion bacteria. Collectively, they make up your gut flora. And these gut flora, also known as your gut microbiota, greatly affect your overall health.
» Read our complete long-read article on Microbiome Gut Brain Axis
» Adrenal Fatigue FAQs
» Take our 3-minute test to see if you may have Adrenal Fatigue
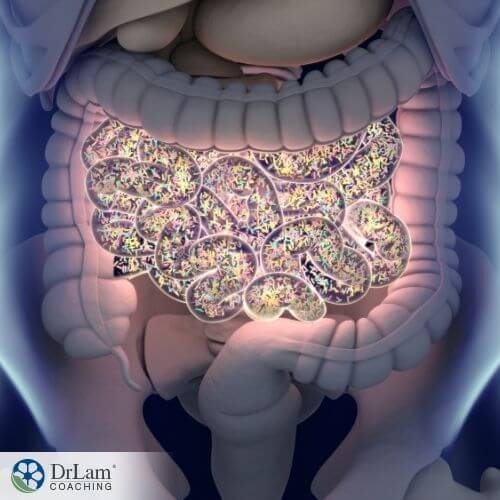 The scientific term for a collection of plant or bacteria, flora describes the bacteria that live on your skin or in your body in medical terms. In this context, flora includes bacteria, yeast, and fungi. Gut flora concerns the microorganisms that inhabit your intestines.
The scientific term for a collection of plant or bacteria, flora describes the bacteria that live on your skin or in your body in medical terms. In this context, flora includes bacteria, yeast, and fungi. Gut flora concerns the microorganisms that inhabit your intestines.
More and more research focuses on the effects of these gut flora on your overall health. You may see several names used for the flora that reside in your intestines. For example, some call them the "microbiota." Others use the term "microbiome." In addition, the terms "gut bacteria," "intestinal flora," and "microflora" all describe these increasingly important bacteria.
Three hundred to five hundred different kinds of bacteria containing at least two hundred genes live and thrive in your gut. And every person’s collection of gut flora differs from every other person’s. Partly, this unique mixture comes from your mother’s gut flora because that is the environment to which you’re exposed during birth. Another part comes from your lifestyle, primarily what you eat.
Bacteria live throughout your body, but the ones in your gut appear to have the most effect on your overall health. These gut flora line your entire digestive tract, most in your intestines and colon. Research indicates they affect all of your health from your immune system to your metabolism and your mood.
Digestive substances in your body delineate where these bacteria colonize to a great extent. The acids in your stomach and bile, along with enzymes from your pancreas may prevent the growth of bacteria in your stomach and small intestine. In fact, problems can arise if bacteria begin growing in your small intestine. This condition, small intestine bacterial overgrowth (SIBO), can occur when dysbiosis happens in your gut. Dysbiosis can occur in conditions like Adrenal Fatigue Syndrome (AFS) or when the immune circuit of your NeuroEndoMetabolic (NEM)stress response becomes dysregulated.
Consequently, most of your gut flora reside in your large intestine, although some may live in the latter part of your small intestine. And all of these bacteria and other microorganisms remain separated from the rest of your body by a single layer of epithelial cells lining your large intestine.
In its normal response to stress from any source, your body activates your adrenal glands to produce and release cortisol to fight the effects of that stress. Ideally, once the stress resolves, you no longer need extra cortisol, and your adrenal glands return to normal. However, in the continuing stress of this culture, your adrenals may continue to be stimulated. Over time, the demand for cortisol may become overwhelming, leading to adrenal fatigue when they no longer can produce sufficient cortisol. This begins the long road of Adrenal Fatigue Syndrome (AFS). One of the chief results of AFS involves increased inflammation throughout your body, including in your gut.
Another automatic mechanism that your body uses to keep its systems functioning in balance when under stress is the NeuroEndoMetabolic (NEM) stress response. This mechanism consists of six interconnected circuits of three organs or systems each. Every one of these circuits deals with a specified part of your body. The inflammation circuit makes up a key responder when your body encounters stress. This circuit contains your immune system, gut, and microbiome. Because of this connection, if stress dysregulates the inflammation circuit, it can affect your gut flora significantly.
 Animal research indicates prolonged stress can ‘turn on’ genes that make changes in gut bacteria that lead them to become destructive pathogens that spread throughout the body and infect tissue. In addition, this type of change shows a link in humans to the development of autoimmune disorders. The link appears possible due to the significant amount of cross-communication between the immune system and the gut.
Animal research indicates prolonged stress can ‘turn on’ genes that make changes in gut bacteria that lead them to become destructive pathogens that spread throughout the body and infect tissue. In addition, this type of change shows a link in humans to the development of autoimmune disorders. The link appears possible due to the significant amount of cross-communication between the immune system and the gut.
Other research shows a change in the gut coming from stress and depression. This change comes about due to increased stress hormones, added inflammation, and changes in the autonomic nervous system. In addition, when gut bacteria come under stress, they release toxins, metabolites, and neurohormones that affect mood and eating behavior. Your eating habits may become dysregulated under the influence of some of these bacterial species. Further, gut bacteria can increase sensitivity to stress and increased the risk of depression.
Likewise, stress can bring about changes in your gut bacteria which then will affect your immune system. For example, you may experience changes in the composition of the bacteria in your gut, a change in the diversity of bacteria, and changes in the number of bacteria in your gut.
Stress can also cause changes that lead to leaky gut and an overactive immune system, as will be discussed below.
When you’re born, researchers believe your gut contains few, if any, flora. Consequently, it appears sterile. Your passage through the birth canal exposes you to your mother’s gut flora, which then begins populating your microbiome. Likewise, your gut flora continues to grow, influenced by your environment, your intake of breast milk and/or formula, and the food you eat.
However, babies born by cesarean section and who don’t pass through the birth canal don’t get their mothers’ flora. Their microbiome grows under the influence of the environment and the intake of nourishment. Some researchers believe these children develop a weaker microbiome and may suffer an increased risk of some types of illnesses.
Most importantly, your gut flora continues to develop throughout your life span, depending greatly on diet and lifestyle factors.
Ongoing research finds more and more support for the idea that your microbiome influences your overall health to a great extent. Two of the most important tasks your gut flora perform include the protection of your immune system and metabolism.
 Your gut flora works to protect your immune system in a couple of ways.
Your gut flora works to protect your immune system in a couple of ways.
Firstly, healthy gut bacteria work alongside your immune system in the lining of your intestine to fight unhealthy bacteria and other microorganisms that may cause health risks.
Secondly, they directly protect the lining of your large intestine, preventing harmful substances from crossing that single layer of epithelial cells.
As a result of this second task, if your inflammatory circuit of the NEM becomes dysregulated, the ratio of healthy to unhealthy bacteria in your microbiome becomes unbalanced. This can lead to the normally tight junctions between the epithelial cells in your large intestine becoming loose. Therefore, harmful bacteria and other substances may access your bloodstream and cause significant harmful effects.
When this occurs, your immune system becomes triggered to fight these foreign substances. Inflammation increases in an effort to deal with them, becoming systemic and harmful in itself. Your immune system may become overwhelmed, leading it to become hyperactive and attacking healthy cells in addition to the unhealthy ones. This can lead to a significant risk of the development of autoimmune health conditions.
In addition to protecting your immune system, your gut flora also works to support your metabolism. It plays a vital role in supplying you with adequate nutrition through vitamins and other nutrients. Likewise, it assists in digesting some carbohydrates that may not completely digest in your small intestine. This helps provide you with more nutrients, controls the storage of fat, and encourages the growth of epithelial cells.
Research shows a number of illness conditions connected to an imbalance of gut flora. These problems may not only affect your digestive system. They can affect your overall health as well. For example, some of the conditions more directly related to imbalanced gut flora include:
Research indicates the gut flora of healthy people differs from that of unhealthy people. For instance, those with some health conditions may lack a wide variety of bacteria, may contain too many types of certain bacteria, or too few of other types. Several of these conditions are discussed below.
As discussed above, your gut flora supports your metabolism. They can affect how many nutrients you get from the food you eat and how many calories you draw from it. If you have too many bacteria in your gut, they may work to turn fiber into fatty acids. As a result, you may build up deposits of fat in your liver. These deposits may then lead to a condition called metabolic syndrome that increases the risk of developing type 2 diabetes, obesity, and heart disease.
 While research does not yet provide a clear explanation for how conditions such as ulcerative colitis and Crohn’s disease develop, the microbiome of people who suffer from these conditions appears to contain fewer anti-inflammatory gut bacteria. Researchers believe some types of gut bacteria stimulate your body to attack the intestines and provide the basis for these conditions to develop.
While research does not yet provide a clear explanation for how conditions such as ulcerative colitis and Crohn’s disease develop, the microbiome of people who suffer from these conditions appears to contain fewer anti-inflammatory gut bacteria. Researchers believe some types of gut bacteria stimulate your body to attack the intestines and provide the basis for these conditions to develop.
Some studies show the microbiota of people who suffer from colon cancer contains more disease-causing bacteria than those who do not develop it.
Research indicates a definite connection between your brain and your gut. This gut-brain connection contains numerous communication pathways between the two. Research in this area shows an association between an imbalance in gut flora and disorders of the central nervous system, including anxiety, autism spectrum disorder, and depression.
Scientists speculate that the microbiome of people who suffer from rheumatoid arthritis may contain higher levels of bacteria associated with inflammation than those who do not develop it.
As noted above, much of your microbiome continues developing based on the foods you eat. Unfortunately, the standard American diet consists of large amounts of fats and sugars. This tends to weaken your gut flora and can lead to a higher risk of several types of illness conditions. However, you can begin improving your gut flora by ingesting the right kinds of foods.
Many people get into a rut of eating the same foods over and over. As a result, your gut flora may weaken. A healthy gut flora contains a wide range of bacteria that thrive on different foods. These many species of bacteria all play different roles in your overall health. Thus, a diverse microbiome indicates better health. This is why eating a diverse range of foods helps support a more diverse microbiome.
Prebiotic foods feed certain types of beneficial bacteria in your gut. These foods consist of complex carbohydrates and fiber that your body doesn’t digest. However, the bacteria in your microbiome will digest them, breaking them down to use for fuel.
Fruits, vegetables, whole grains, and some starches contain prebiotics. A large number of studies show these prebiotics increase the growth of bacteria such as Bifidobacteria. In addition, other research shows prebiotics also can benefit people with certain conditions. For example, some prebiotics reduce cholesterol, triglyceride, and insulin levels in obese people. These prebiotics may reduce the risk of certain illness conditions that come with obesity, such as heart disease and diabetes.
 Research shows vegetables and fruits to be the best source of nutrients for a more healthy microbiome. These foods contain a lot of fiber, or prebiotics, which is hard for your body to digest. However, certain gut flora in your system can digest them, leading to more growth for these bacteria. High amounts of fiber come in a number of these foods. For example,
Research shows vegetables and fruits to be the best source of nutrients for a more healthy microbiome. These foods contain a lot of fiber, or prebiotics, which is hard for your body to digest. However, certain gut flora in your system can digest them, leading to more growth for these bacteria. High amounts of fiber come in a number of these foods. For example,
Some research shows eating a diet high in vegetables and fruits can even prevent some bacteria that cause diseases from growing.
Other foods can stimulate the growth of healthy bacteria, such as Bifidobacteria, which can increase the health of your gut and work to prevent intestinal inflammation.
For example, apples, blueberries, pistachios, almonds, and artichokes work to increase Bifidobacteria in your gut.
Whole grains contain more fiber and non-digestible carbohydrates that become fuel for beneficial bacteria in your gut flora. They also help decrease inflammation and risk factors for heart disease.
Because the body doesn’t always digest polyphenols, they get to the large intestine where gut bacteria digest them. Their health benefits include reducing blood pressure, cholesterol levels, oxidative stress, and inflammation. These foods include berries, vegetables, cocoa, coffee and tea, olives, and nuts.
Fermenting usually involves microbes, such as bacteria and yeasts, converting sugars in your food into organic acids or alcohol. Fermented foods typically contain lactobacilli, a type of beneficial bacteria. For example, foods like:
Research shows that the gut flora of people who eat large amounts of yogurt consist of higher levels of lactobacilli. Their microbiomes also contain fewer Enterobacteriaceae, a bacteria shown to increase inflammation and linked to some chronic illness conditions.
Other studies show eating yogurt may help with lactose intolerance in both infants and adults. In addition, studies show it also enhances the functioning and composition of your microbiota. In people with irritable bowel syndrome, some types of yogurt may reduce the amount of certain disease-causing bacteria.
However, you should keep in mind that some yogurts contain significant amounts of sugar. The best type of yogurt remains plain, natural yogurt.
Foods are the best source of beneficial bacteria and probiotics. However, sometimes supplements can help fill the gaps. Research indicates these supplements aid in changing the composition of your gut flora and help your metabolism. Research also shows their greatest benefit may lie in helping to restore your gut flora after becoming compromised. It's important to take care to get a good supplement with a high number of diverse bacteria that is properly stored.
 Widely used as substitutes for sugar, artificial sweeteners can lead to a negative effect on your gut flora. A study with rats that consumed aspartame found it did help lose weight, but it also led to an increase in blood sugar and impaired insulin response. In addition, the intestines of rats fed aspartame also contained higher levels of Clostridium and Enterobacteriaceae. Both of these bacteria types can lead to illnesses at high levels. Other research of the same type with humans had similar results.
Widely used as substitutes for sugar, artificial sweeteners can lead to a negative effect on your gut flora. A study with rats that consumed aspartame found it did help lose weight, but it also led to an increase in blood sugar and impaired insulin response. In addition, the intestines of rats fed aspartame also contained higher levels of Clostridium and Enterobacteriaceae. Both of these bacteria types can lead to illnesses at high levels. Other research of the same type with humans had similar results.
In order to increase the diversity and growth of your baby’s microbiota, you should continue breastfeeding for six months or more. Research shows a baby’s gut flora continues developing for the first two years and contains high levels of Bifidobacteria, which can break down the sugars in breast milk. On the other hand, babies fed formula tend to have lower levels of this beneficial bacteria. Likewise, breastfed babies tend to suffer from fewer allergies and to develop obesity less often.
» Read our complete long-read article on Microbiome Gut Brain Axis
» Adrenal Fatigue FAQs
» Take our 3-minute test to see if you may have Adrenal Fatigue
Gut flora exert a significant influence on your overall health. This is why it is important to care for the diversity and health of the bacteria that reside in your intestines. One of the best ways to do this is to change your diet to include more foods high in fiber and probiotics to support a diverse and strong microbiome.
If you would like to know more about or need assistance with improving your gut flora, the team at Dr. Lam Coaching can help. We offer a free** no-obligation phone consultation at +1-626-571-1234 where we will privately discuss your symptoms and various options. You may also send us a question through our Ask The Doctor system by clicking here.
The wide variety of gut flora living in your intestines have been shown by research to be very influential in your overall health. Keeping a good balance between healthy and unhealthy bacteria there is extremely important in keeping your body healthy overall. The health of your gut flora depends on the foods you eat.