
 Chronic inflammation and Adrenal Fatigue are quite closely associated: inflammation contributes to and triggers common, but very subtle, symptoms of Adrenal Fatigue such as brain fog, gastric bloating, pain of unknown origin, depression, anxiety, and reactive hypoglycemia. Let us start by trying to understand a little bit more about inflammation itself.
Chronic inflammation and Adrenal Fatigue are quite closely associated: inflammation contributes to and triggers common, but very subtle, symptoms of Adrenal Fatigue such as brain fog, gastric bloating, pain of unknown origin, depression, anxiety, and reactive hypoglycemia. Let us start by trying to understand a little bit more about inflammation itself.
Inflammation is a process started by your own body as part of its response to stress, whether physical or emotional. An example of physical stress would be an ankle sprain. Emotional stress can arise from a heated argument or relationship difficulties. Inflammation involves a complex biological cascade of molecular and cellular signals that alter physiological responses, ultimately resulting in the familiar clinical symptoms of pain, swelling, heat, and redness. These four classic symptoms of inflammation were first described in the first century AD by the Roman medical writer Celsus: rubor, meaning redness; tumor, meaning swelling; color, meaning heat; and dolor, meaning pain. In Latin, the original root of the word inflammation is inflammation, which means “setting on fire.”
So why does your body become inflamed, causing you pain and discomfort? It turns out that this is absolutely necessary for your body’s normal repair processes to occur. Inflammation is the process by which your body fights off and expunges whatever is causing it harm or stress. The discomfort we feel is simply collateral damage of this process.
Inflammation begins when your body rallies to defend itself from toxins or pathogenic invaders or to heal damage. Blood capillaries dilate and the vessel walls become porous, allowing white blood cells to move out of the vessel and to the site of damage or infection. This infusion of blood and fluid into a region of your body causes the characteristic swelling, which often puts pressure on nearby nerves, creating discomfort and pain. The inflammatory molecules may also trigger the activation of pain signals, intensifying the discomfort. The feeling of heat in the inflamed tissue is a result of the increased blood flow to that area.
In general, then, the inflammatory response of your body is a natural biological phenomenon that your body engages in to keep itself healthy and functional. But problems can occur when inflammation begins to run rampant without a proper controlling influence to oppose it, leading to chronic inflammation.
While both physical and emotional stress can trigger inflammation, the intensity of an emotionally triggered inflammatory response tends to be less than a physically triggered one. Remember that inflammation is a body’s automatic response to any form of injury, whether real or perceived. Although the acute inflammatory responses that cause short term pain (due to swelling) benefit your body in the long term, the modern epidemic of chronic, low-grade inflammation due to emotional stress slowly destroys your body’s balance. With the continuous, low-grade inflammation that is typical of emotional stress, your body's systems experience a constant inflammatory response, putting them in an unbalanced state, and you become more susceptible to the effects of aging and disease. In fact, it is this subclinical chronic inflammation that, in the end, causes many of the symptoms that are actually perceptible to an individual. This subclinical inflammatory state often festers for years before it becomes apparent or clinically significant. The length of time this inflammatory state has been aggravated is often directly linked to the severity of the resulting condition, as well as its prognosis In fact, the effect of the body’s inflammatory response is the cause behind many chronic diseases.
 The acute signs of inflammation are familiar and recognizable, as already mentioned: swelling, redness, heat, and pain. However, signs of chronic inflammation are often more subtle. These include frequent infections, irritable bowel, bloating, food sensitivities, dizziness, pain of unknown origin, brain fog, anxiety, and depression.
The acute signs of inflammation are familiar and recognizable, as already mentioned: swelling, redness, heat, and pain. However, signs of chronic inflammation are often more subtle. These include frequent infections, irritable bowel, bloating, food sensitivities, dizziness, pain of unknown origin, brain fog, anxiety, and depression.
In a healthy body, the fire of acute inflammation is tightly controlled: it turns on at the right time to battle invaders and start the repair process, and just as critically, it turns off so that the body can get back to its normal functions. The turning off process is controlled by cortisol, our body’s anti-stress hormone. While inflammation itself is an unpleasant process, your body is designed to tolerate some inflammation and to control it. Research has revealed, however, that low-level chronic inflammation can simmer quietly and insidiously in the body, in the absence of overt trauma or infection, and have profound effects on our physical and mental health.
In cases where inflammation is tied to a specific chronic condition, the inflammation is generally local: in the arteries for those with heart disease, in the brain for those with Alzheimer’s, or in the pancreas for those with diabetes. Certain foods and environmental toxins also give rise to inflammation throughout the body, involving disparate areas, including the brain. This can affect your health, mental acuity, and even lifespan.
Other illnesses with a strong component of inflammation include psoriasis, stroke, fibromyalgia, gastroesophageal reflux disease (GERD), Hashimoto's thyroiditis, lupus, asthma, allergies, autism, celiac disease, and Crohn’s Disease.
Other conditions that involve inflammation include:

Unfortunately, the weapons for fighting inflammation are extremely imprecise. Analgesic and non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen are tools of temporary benefit; they only act to suppress inflammation, not the underlying condition. They reduce pain, alleviate the swelling, and make us feel better in the short term, but they do not address the root of the problem.
Steroids, however, are like indiscriminate weapons of mass destruction that slow down the whole immune system. They are great tools for fighting inflammation, but they also raise the risk of infection, erode the bones, predispose the patient to diabetes, and cause mood swings. Steroids have also been found to affect blood vessel walls, possibly increasing the risk of blood clots.
Statins are another important category of drugs. They are widely used to combat high cholesterol in your body, but they also have anti-inflammatory properties. Statins can lower your chance of having a heart attack, but there are mounting concerns about the possible side effects, including muscle pains and an increased risk of diabetes.
The decision regarding what type of drug to use to control your inflammation is further complicated by the grade and severity of your inflammation, where and how the inflammation is localized, as well as the suspected root cause of the inflammation (if known).
Common causes of chronic inflammation include:
 Mild but chronic allergies or sensitivities to food that may have only subtle symptoms.
Mild but chronic allergies or sensitivities to food that may have only subtle symptoms. An inflammatory response is activated whenever our body is stressed. To control this inflammation so that it does not go rampant, our adrenal glands secrete cortisol, the main anti-stress hormone, which calms the inflammatory process. This balance allows the body to return to a normal state after the inflammation is no longer needed. With chronic stress, however, inflammation persists in your body. The adrenals are put on overdrive to constantly secrete cortisol under the direction of the hypothalamic-pituitary-adrenal (HPA) axis. If stress is unrelenting, our adrenal glands can ultimately become exhausted, a condition known as Adrenal Fatigue. At first, the body simply becomes progressively more fatigued. In advanced stages, common symptoms of Adrenal Fatigue include reactive hypoglycemia, chronic Inflammation, low blood pressure, insomnia, anxiety, depression, heart palpitations, reduced exercise capacity, menstrual irregularities, and low thyroid symptoms. A body in advanced Adrenal Fatigue has a limited ability to control inflammation, leading to a variety of other problems.
An inflammatory response is activated whenever our body is stressed. To control this inflammation so that it does not go rampant, our adrenal glands secrete cortisol, the main anti-stress hormone, which calms the inflammatory process. This balance allows the body to return to a normal state after the inflammation is no longer needed. With chronic stress, however, inflammation persists in your body. The adrenals are put on overdrive to constantly secrete cortisol under the direction of the hypothalamic-pituitary-adrenal (HPA) axis. If stress is unrelenting, our adrenal glands can ultimately become exhausted, a condition known as Adrenal Fatigue. At first, the body simply becomes progressively more fatigued. In advanced stages, common symptoms of Adrenal Fatigue include reactive hypoglycemia, chronic Inflammation, low blood pressure, insomnia, anxiety, depression, heart palpitations, reduced exercise capacity, menstrual irregularities, and low thyroid symptoms. A body in advanced Adrenal Fatigue has a limited ability to control inflammation, leading to a variety of other problems.
To fully understand the pathophysiology of inflammation, we need to first understand that the body’s overall response to stress is governed by its neuroendometabolic stress response. This response has six major components that help our body maintain homeostasis, which is necessary for long term survival. Here is graphical representation of the components of the neuroendometabolic stress response:
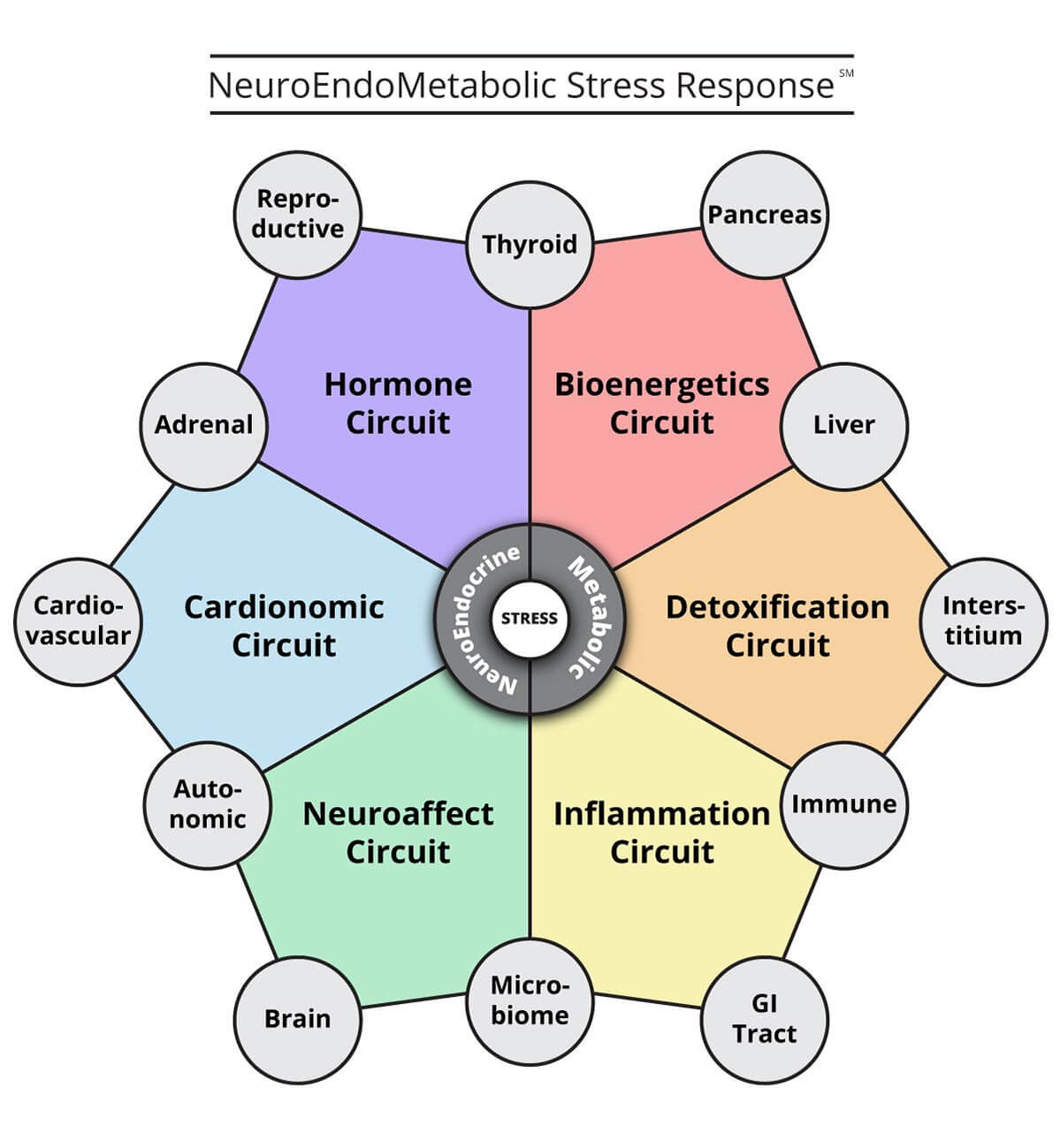
The inflammatory response is one of these key components in how our body reacts to stress. Inflammation works synergistically with other systems and organs to properly react to the situation while maintaining crucial functions.
The most important systems that affect inflammation in your body are the:
To understand how inflammation affects your body, let’s look at these individual components in more detail.
Inflammation is an important part of innate immunity. Innate immunity refers to nonspecific mechanisms that respond to any threat or stressor the body many encounter, as opposed to mechanisms that target specific pathogens.
Acute inflammation is a normal process that helps to protect and heal the body in response to physical injury or infection. However, if your body's inflammatory response continues for a prolonged period of time, the inflammation is said to be chronic. Chronic inflammation can be the result of an infection, an environmental antigen such as pollen, an autoimmune reaction to the body’s own material, or the persistent activation of inflammatory molecules. Chronic inflammation is primarily mediated by the immune system components known as macrophages and monocytes.
Macrophages and monocytes are both classes of leukocytes, a type of immune cell commonly known as a white blood cell. Leukocytes release reactive oxygen species (ROS) and proteases, chemical agents that destroy whatever has triggered the inflammatory response; however, these agents are indiscriminate and attack not only the foreign invaders but also the body’s own tissues. The damaged tissues must be continuously repaired by replacement of damaged cells, either with the same type of cells or with fibrous connective tissues. Another important characteristic of chronic inflammation is local angiogenesis—the development of new blood vessels. As part of the inflammatory response, the damaged tissues also undergo repair. The affected areas are replaced by new functional cells or fibrous connective tissues; and the site undergoes angiogenesis, building new blood vessels to supply the new tissue with blood. This repair work, although started by your body with the best of intentions, can actually be disruptive, and the irritation it causes can retrigger inflammatory processes. If this cycle repeats itself time after time, the cascade can continue indefinitely and keep your body in a chronic inflammatory state. Chronic inflammation is abnormal and does not benefit the body.
 The fact that your immune system is the driver of your body’s inflammatory response to disease is well established. Unfortunately modern allopathic medicine does not provide solutions for long term alleviation of immune- and autoimmune-driven chronic inflammation. Oftentimes, immunosuppressive therapy or steroids are recommended by doctors in order to suppress the immune system response. But while these approaches reduce inflammation, neither addresses the underlying pathology to heal the body.
The fact that your immune system is the driver of your body’s inflammatory response to disease is well established. Unfortunately modern allopathic medicine does not provide solutions for long term alleviation of immune- and autoimmune-driven chronic inflammation. Oftentimes, immunosuppressive therapy or steroids are recommended by doctors in order to suppress the immune system response. But while these approaches reduce inflammation, neither addresses the underlying pathology to heal the body.
Until the actual cause of inflammation is addressed, the problem remains and continues to consume resources and destroy tissues.
The majority of inflammatory diseases actually begin in the gastrointestinal (GI) tract. A single autoimmune response there can magnify and spread through the body to become a systemic inflammatory reaction.
Your GI tract is a very large and complex organ system with an intricate semi-permeable lining. In fact, the internal surface area of the gut could cover two tennis courts! The permeability of the GI tract lining changes in response to various body functions and chemical reactions. If the hormone cortisol, for example, rises in response to a stressful argument, or if thyroid hormone levels fluctuate due to disruptions in your sleep cycle, the intestinal lining becomes more permeable; the tight junction responsible for holding adjacent mucosal cells together to prevent penetration becomes laxer in response to the those hormones. In this more permeable state, difficult to digest food particles, toxins, and pathogens such as bacteria, viruses, or yeasts have a greater chance of making it past the intestinal wall and into your bloodstream. The invading toxins and pathogens trigger an immune response, which causes inflammation, allergic reactions, and other symptoms we relate to a variety of diseases.
Furthermore, when the intestinal lining is repeatedly damaged due such recurring “leaks”, the microvilli cells of the gut lining start to break down and are rendered unable to process the nutrients and facilitate the work of enzymes vital to proper digestion. Digestion becomes impaired and nutrient absorption becomes problematic, preventing proper energy and nutrient intake from food.The diminished nutrient intake capacity further degrades the health of the body, making it even more susceptible to disease.
 This situation can become quite serious, leading to severely debilitating conditions. The immune system can become overburdened, allowing pathogens and toxins to cycle through your bloodstream, where they can affect joints, muscles, connective tissues, nerves, and even other organ systems. Leaked toxins entering our bloodstream from the gut can enter the brain, causing inflammation and resulting in depression. It has been also been shown that many of the inflammatory diseases we suffer from are gut mediated but do not present as gut issues. For example, gluten sensitivity can be primarily, and at times exclusively, a neurological disease. In other words, some people show gluten sensitivity because of problems with their brain functions, despite having no gastrointestinal problems whatsoever. No organ is spared when the gut is inflamed. Without a healthy gut, it is impossible to feel vibrant and healthy. The many symptoms associated with these issues are referred to collectively as leaky gut.
This situation can become quite serious, leading to severely debilitating conditions. The immune system can become overburdened, allowing pathogens and toxins to cycle through your bloodstream, where they can affect joints, muscles, connective tissues, nerves, and even other organ systems. Leaked toxins entering our bloodstream from the gut can enter the brain, causing inflammation and resulting in depression. It has been also been shown that many of the inflammatory diseases we suffer from are gut mediated but do not present as gut issues. For example, gluten sensitivity can be primarily, and at times exclusively, a neurological disease. In other words, some people show gluten sensitivity because of problems with their brain functions, despite having no gastrointestinal problems whatsoever. No organ is spared when the gut is inflamed. Without a healthy gut, it is impossible to feel vibrant and healthy. The many symptoms associated with these issues are referred to collectively as leaky gut.
In addition to the gut itself as a source of inflammation, there is also the microbiome—trillions of microbes that live in and on your body, including within your gut— which can also play a role in inflammation.
You may think of your body as a single organism, but in reality, your body harbors trillions of commensal microorganisms that are intricately tied to maintaining homeostasis and functional balance within your body. The relationship is so intimate that the human body can be considered a metaorganism; interactions between the human host and its resident microbes are a critical part of its development and function. These populations of microbes and the environment they live in and help to keep healthy are collectively known as the microbiome.
When your internal microbiome is disrupted by illness, stress, or antibiotic medications, the composition and functionality of the microbiome is altered, a state known as dysbiosis. Dysbiosis is involved in several metabolic and inflammatory diseases, and is thought to be connected to many more.
If your gut microbiome is altered due to mass die-off of microbial populations from antibiotic medications, normal gut functions may be negatively affected by the limited functional capacity of the remaining gut microbes. In addition, the reduced population size creates a vulnerable niche which other, less beneficial bacterial or fungal organisms may colonize. These other organisms are often detrimental to your gut health, producing toxins and irritating the gut lining; this can, in turn, have implications for all of the other systems in your body, as discussed above.
Unlike acute inflammation, which causes localized redness and swelling of a particular affected area, chronic inflammation effects are more diffuse and systemic. They also develop and affect the body over long periods of time Signs and symptoms include:
 Food sensitivity
Food sensitivitySince inflammation is commonly mediated by the gut, proper evaluation of an inflammatory condition often starts with the gastrointestinal tract. There are seven common areas that should be considered when looking at causative factors for gastrointestinal dysfunction that has produced chronic inflammation. They are listed below, along with key triggers within the category of evaluation:
Common laboratory indicators of chronic inflammation include elevated:
 Psychological stress manifesting in the form of panic attacks, rapid heart rate, or night sweats is a sign of cortisol-prompted inflammation. Cortisol is your body’s general “fight or flight” hormone, kicking in whenever the adrenal glands respond to a threat or stressor. An increase in cortisol results in dilated blood vessels and increased blood flow to your organs so as to prepare the body to respond to an attack. With persistent stress, the adrenal glands and immune system are constantly in overdrive, eliciting the Chronic Inflammation response.
Psychological stress manifesting in the form of panic attacks, rapid heart rate, or night sweats is a sign of cortisol-prompted inflammation. Cortisol is your body’s general “fight or flight” hormone, kicking in whenever the adrenal glands respond to a threat or stressor. An increase in cortisol results in dilated blood vessels and increased blood flow to your organs so as to prepare the body to respond to an attack. With persistent stress, the adrenal glands and immune system are constantly in overdrive, eliciting the Chronic Inflammation response.
Unexpected stressful situations, such as being put on the spot at a work meeting, can also trigger sudden bouts of anxiety and the cortisol stress response. It’s important to understand that the parts of your brain that sense pain also responds to social and mental stress.
Your body’s response to physical stress is similar to its response to emotional stress. For example, a hypoglycemic episode puts the body into a panic mode that triggers the immune response, leading to systemic inflammation. This can disrupt your body’s normal homeostasis and lead to systemic reactions such as breaking out in hives and the shutting down your GI tract. Restoring the body to equilibrium, in this case by providing it with the proper nutrients, often restores the body’s functions to normal. Skipping meals or eating at odd times, however, will continuously disturb the body’s balance, triggering immune reactions and inflammatory episodes.
Gut disturbances from an unbalanced diet can often be the source of inflammation. Simply eating an anti-inflammatory diet with the proper balance of nutrition from healthy sources is a powerful method to keep the gastrointestinal tract working at optimal function. Prebiotic and probiotic supplements and exercise can also bolster your GI tract health. On the other hand, if you eat a meal that’s particularly rich, your digestive system is forced to put in extra work. It’s unfortunate that the modern diet in developed countries consists of so many processed fast foods that are overloaded with sugars, fats, and carbohydrates. This leads many people to unduly stress their digestive tract, triggering chronic inflammation.
Studies have linked insulin and glucose levels with chronic inflammation. For instance, obese individuals who are prone to developing type-2 diabetes often have issues with chronic inflammation. In addition, studies have shown that consuming foods high in simple carbohydrates that quickly spike your postprandial blood sugar also seems to trigger an inflammatory response.
Inflammation has also been linked to unbalanced levels of certain hormones, including estrogen, progesterone, and testosterone. That’s why chronic inflammation often affects menopausal women, causing conditions like osteoporosis, weight gain, and adult acne. Furthermore, since the level of any one hormone is tied to multiple others through the body’s hormonal axes, disequilibrium in a single hormone can cascade, affecting hormonal balance across the board.
Certain individuals may experience allergies or sensitivities leading to inflammatory responses in reaction to the synthetic fibers found in products like latex, adhesives, and plastics. You may not realize that these synthetic triggers exist in your workplace or home.
 Chemicals in cleaning products, cosmetics, and air fresheners are another common source of inflammation. Some of these chemicals can be particularly harmful if they can become airborne or are absorbed directly through the skin. Even low levels of chemical exposure can give rise to chronic inflammation.
Chemicals in cleaning products, cosmetics, and air fresheners are another common source of inflammation. Some of these chemicals can be particularly harmful if they can become airborne or are absorbed directly through the skin. Even low levels of chemical exposure can give rise to chronic inflammation.
When you gain weight, the fat cells of adipose tissue actually enlarge and can begin to bulge. This stresses the cells and causes them to call for help. The immune system responds and the affected tissues become inflamed. If these cells remain stressed, the immune system remains activated and the inflammatory response continues, the white blood cells sent to these tissues start to leak out and enter the bloodstream, and need to be cleaned up by the liver.
Weight gain is very often the result of either overeating or consuming too many processed foods. As previously mentioned, the modern diet is full of exactly these kinds of food: potato chips, frozen dinners, white bread, and sugary frosting. The prevalence of these kinds of foods make it all too easy to inadvertently raise your risk of chronic inflammation.
Limiting your consumption or making healthier food choices with an eye towards controlling your weight will help you control the size of your fat cells. Once they stop feeling the stress of being overfilled, they will no longer call for help, and the immune system and its inflammatory response will also quiet down.
Another way to help cut those fat cells down to size is through exercise; but even if you already look lean, exercise may still protect you from unnecessary inflammation. Studies in both human and animal subjects indicate that physical activity decreases inflammation of both chronic and acute varieties. Physical activity on a regular basis is also important in reducing your risk for obesity and other chronic diseases associated with inflammation.
But don’t overdo it. Excessive or overly intense exercise actually stresses the body and pushes it into a chronic inflammatory state which can trigger adrenal crashes. In fact, overtraining syndrome is so named for athletes pushing themselves too far, and is linked with a suppression of immune function as well as systemic chronic inflammation.
Smog is an unfortunate reality in many modern cities. Whether or not you noticed it, your immune system certainly hates it. When the toxins in polluted air are inhaled and enter your bloodstream, your immune system reacts with an inflammatory response, causing a variety of chronic symptoms including the buildup of insulin resistance.
 Even worse than polluted air from the city or around highways is cigarette smoke; tobacco smoke is so irritating and damaging to the lungs that the immune response to repair the damage is overblown. While trying to fix the damage caused by smoking, the immune system’s assault on the invading toxins causes a great deal of collateral damage to the lung tissue. Over time, the damage caused by the war between toxic tobacco smoke and your immune response can lead to lung disease.
Even worse than polluted air from the city or around highways is cigarette smoke; tobacco smoke is so irritating and damaging to the lungs that the immune response to repair the damage is overblown. While trying to fix the damage caused by smoking, the immune system’s assault on the invading toxins causes a great deal of collateral damage to the lung tissue. Over time, the damage caused by the war between toxic tobacco smoke and your immune response can lead to lung disease.
Key nutrients that have anti-inflammatory properties include fish oil, probiotics, vitamin C, glutathione, enzymes, quercetin, bromelain, vitamin E, turmeric, curcumin, vitamin D. Depending on the state of the body, more nutrients are not necessarily better. Avoid pills that have excessive binders and fillers, which can be inflammatory. Focus on liquid or powder delivery systems for better bioavailability.
Adrenal Fatigue sufferers should be extremely careful not to indiscriminately take supplements without careful consideration of the body’s ability to clear the metabolites promptly as excessive accumulation of metabolic byproducts can trigger inflammatory responses and adrenal crashes. Those in advanced stages are particularly at risk, because the liver is often already congested, and the extracellular matrix is polluted, resulting in a slowdown of nutrient assimilation. An aggressive nutritional program can often make matters worse. Improper nutritional supplementation is a common clinical mistake that can retard Adrenal Fatigue recovery and even exacerbate the condition.
Trigger foods aren’t necessarily bad for you themselves, but they have the potential to stress the body and cause inflammation. Certain oils— corn, peanut, soy, sunflower and safflower—contain high levels of linoleic acid, which can trigger an inflammatory reaction in some people. For others, simple carbohydrates may irritate the body, and a diet high in such refined carbohydrates may stress the body and cause an inflammatory response.
Other common triggers include casein, which is found in dairy products, and gluten, found in wheat. For individuals sensitive to these foods, ingesting them will cause stress and discomfort in the gastrointestinal tract, upsetting the internal balance of the gut and triggering inflammation.
It is therefore important to identify what foods you are sensitive to and eliminate them from your diet. This will soothe your gut and allow the inflammatory response to subside. Using prebiotics and probiotics to encourage the growth of “good” bacteria in your gut microbiome can also keep the gut happy and assist healthy digestive function.
Fresh fruits and vegetables are the most effective anti-inflammatory foods. They contain a vast array of phytocompounds that help fight inflammation. Along with magnesium and various antioxidants, these compounds include the carotenoids that give carrots and squash their yellow coloring and lycopene, which gives tomatoes and red bell peppers their red color.
Resveratrol is a phytochemical that has recently been touted for its ability to fight heart disease. This powerful compound has great advantages for cardiovascular health and also helps to quiet inflammation.
 Nuts and seeds are simple but nourishing foods, bursting at the seams with protein, fiber, phytonutrients, and omega-3 fatty acids. These portable nutritional powerhouses also act as a great snack throughout the day to keep blood sugar and insulin levels stable and provide energy between meals. Walnuts, in particular, contain a variety of phytonutrients that are difficult to find anywhere else.
Nuts and seeds are simple but nourishing foods, bursting at the seams with protein, fiber, phytonutrients, and omega-3 fatty acids. These portable nutritional powerhouses also act as a great snack throughout the day to keep blood sugar and insulin levels stable and provide energy between meals. Walnuts, in particular, contain a variety of phytonutrients that are difficult to find anywhere else.
Olive oil is rich in polyphenols, another powerful anti-inflammatory compound. Extra virgin olive oil used for cooking at temperatures less than 140 degrees Celsius is the most beneficial.
Many herbs and spices contain unique mixtures of vitamins and phytonutrients that help curb inflammation and promote the general health of the body. Turmeric, cinnamon, oregano, rosemary, and lavender all have general health benefits and help to suppress inflammation. In addition, they add flavor to dishes without having to resort to excessive salt or sugar, both of which can elicit inflammatory responses.
Some vegetables—including garlic, asparagus, artichokes, and leeks—are also sources of fructooligosaccharides. In addition to their nutritional benefits, the complexity of these sugars makes them indigestible by the human gut, meaning you’ll absorb fewer calories and your blood sugar won’t spike. These complex sugars also feed the beneficial bacteria in your gut, helping to promote and maintain a healthy gut microbiome.
Avocados are a great health food because they are packed with powerful nutrients. Carotenoids, alpha-linolenic acid, phytosterols, and mono- and polyunsaturated fats all contribute to this food’s multitude of health benefits. Multiple studies link avocado consumption to reduction of inflammation, balanced blood sugar, reduced cholesterol, and even curbed arthritis pains. Avocados are also incredibly versatile as a food, able to be sliced, chopped, mashed, or spread as a garnish, a main dish, or a healthy alternative to butter or mayonnaise.
Grass fed, free range, and organic meats are healthier on the whole than their industrial agriculture counterparts. Their meat offers a much better nutritional value: when compared to corn-fed, industrially farmed animals, pasture raised organic cows, lambs, pigs and chickens have higher levels of omega-3 fatty acids (that fight inflammation) and lower levels of omega-6 fatty acids (that promote inflammation).
Adults should eat three servings each week of cold water fish such as sardines, anchovies, herring, and salmon. Fish are high in polyunsaturated omega-3 fatty acids, which have a wide range of health benefits including improving heart health, alleviating autoimmune conditions, curbing mood disorders, helping skin and nail health, and of course reducing inflammation.
Ginger has long been valued for its anti-inflammatory and general health benefits in many cultures. Modern medicine has only recently caught up: in studies since the 1970s, ginger has been shown to inhibit prostaglandin synthesis and leukotriene biosynthesis, both compounds produced by the body in the course of the inflammatory response. This physiological pathway makes ginger similar to, but functionally unique from, pharmaceutical nonsteroidal anti-inflammatory medications.
 Inflammation is one of the primary mechanisms selected by nature to maintain the integrity of your body against the myriad attacks that it faces every day. It is part of your body’s maintenance and repair system, and without it, you cannot heal. However, inflammation is also a common component in many chronic diseases. This dual nature makes dealing with inflammation a tricky prospect, as a proper balance needs to be found. Unfortunately, modern medicine is ill-equipped to provide a proper solution because it deals mainly with eradicating acute diseases and controlling chronic symptoms.
Inflammation is one of the primary mechanisms selected by nature to maintain the integrity of your body against the myriad attacks that it faces every day. It is part of your body’s maintenance and repair system, and without it, you cannot heal. However, inflammation is also a common component in many chronic diseases. This dual nature makes dealing with inflammation a tricky prospect, as a proper balance needs to be found. Unfortunately, modern medicine is ill-equipped to provide a proper solution because it deals mainly with eradicating acute diseases and controlling chronic symptoms.
Another complicating factor is that properly dealing with chronic inflammation requires addressing the problem at all levels, including identifying the root of the problem. Many of the possible causes of inflammation deal with disruptions and dysbioses in the gut; another related and overlapping set of causes are mediated by the chronic overworking of the adrenal glands in Adrenal Fatigue. In both cases, the proper way to address the inflammation is to remove the stressor or agent eliciting the inflammatory immune response and maneuver the body back to its optimal homeostasis. While this is simple in theory, the application can require time and patience to adjust to dietary and lifestyle changes.
In the end it is more than worth it. Cutting chronic inflammation out of your life will leave you healthier and happier, with more energy and motivation to lead your life the way you want to.
Yes. It can be due to chemical sensitivities. This can become very problematic.