 Truth be told, very few women are aware of menopausal metabolic syndrome (MMS) or even the process their body undergoes during menopause. Menopause has gotten a pretty bad reputation with related hot flashes and mood swings. In order to deal accordingly with the actual physical process the body is undergoing, it is extremely important to separate all the facts from fiction to make the transition from one phase of a woman’s life to another much easier.
Truth be told, very few women are aware of menopausal metabolic syndrome (MMS) or even the process their body undergoes during menopause. Menopause has gotten a pretty bad reputation with related hot flashes and mood swings. In order to deal accordingly with the actual physical process the body is undergoing, it is extremely important to separate all the facts from fiction to make the transition from one phase of a woman’s life to another much easier.
With all of the body’s independent systems integrated to function together in a uniform operation, when one change enters our bodies, such as menopause, it could affect many other systems directly and indirectly. We will focus on the correlation between menopause and the metabolic system and how one affects the other, causing menopausal metabolic syndrome.
The metabolic system includes life sustaining chemical transformations within the cells of all living organisms. Their main purposes are:
All of these allow organisms to grow then reproduce, respond to their specific environments, and maintain their molecular structures. It is the sum of all chemical reactions that occur in the human body and all living things. Many think of it only in terms of digestion, however, with its involvement of transporting substances to and from various cells, its importance in the medical field is of complete importance. It has now been scientifically proven that menopause is a primary reason for metabolic dysfunction. Studies have shown that when women enter menopause, they have increased risk for MMS, a subset of the large clinical condition known as metabolic syndrome, and only combined therapy of BHRTY and Metformin with nutrition therapy could reduce and prevent the risk.
The metabolic system is a series of smaller systems working together in a team formation. The system includes the pancreas, liver, thyroid and hypothalamus, a section of the brain that is responsible for the production of many of the essential hormones and the chemical substances that help control different cells and organs in the body. Just to put the importance of this system into perspective, the hormones secreted from the hypothalamus alone control physiologic functions such as temperature regulation, thirst, hunger, sleep, mood, sex drive, and the release of other hormones within the body.
Although small in size, this section of the brain also houses the pituitary gland, as well as other glands in the body, and is involved in many necessary processes such as behavioral, autonomic, and endocrine functions such as metabolism, growth, and development. All these systems combined play very specific roles, such as digesting food, turning that food into energy, and then processing the energy. If treated well, they will perform the jobs they were created for at optimal levels.
The thyroid controls how the energy of the body is used. If this system is not functioning properly, it is most likely a result of genetic predisposition. However, there are conditions such as Hashimoto’s and Grave’s disease that affect the thyroid; all lead to the body’s inability to metabolize efficiently. For example, if one suffers from a disorder known as hypothyroidism, they do not metabolize fat very easily. On the opposite side of the spectrum is hyperthyroidism, which leads to an overactive metabolism and could prevent a person from gaining weight.
While many like to blame their thyroid when they can’t lose weight, thyroid conditions only contribute to a small portion of obesity cases. In the unfortunate cases where a tumor is found on the thyroid, its removal will most likely cause weight gain in the individual who will then have trouble getting rid of it.
The liver is the big organ in the metabolic system that is responsible for processing the sugars and producing the bile to eliminate fat. If a person’s diet is unhealthy and consists of excess fat, the liver may not be able to produce enough bile to break it all down, digest and excrete it efficiently, resulting in a number of health problems and concerns. This could also be the case if the liver malfunction is caused by a disease or injured by a person who drinks too much alcohol.
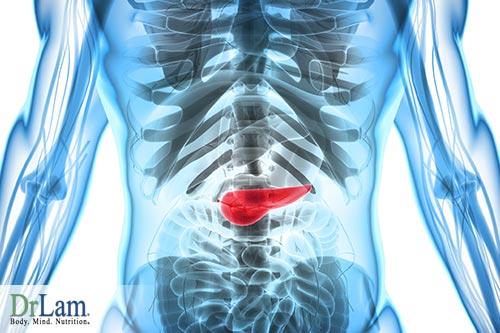 Next, in the metabolic system, we find the pancreas. Upon digestion, calories become fuel. Glucose and blood sugar are converted into energy. The pancreas creates the insulin in which the body uses to regulate blood sugar and sends it to the parts of the body which need it the most. If the body falls short of glucose, a person can feel shaky, indicating, it needs more glucose. If the system receives too much, the energy is then stored, and turned into fat. The pancreas also works closely with the GI tract by releasing enzymes to process food.
Next, in the metabolic system, we find the pancreas. Upon digestion, calories become fuel. Glucose and blood sugar are converted into energy. The pancreas creates the insulin in which the body uses to regulate blood sugar and sends it to the parts of the body which need it the most. If the body falls short of glucose, a person can feel shaky, indicating, it needs more glucose. If the system receives too much, the energy is then stored, and turned into fat. The pancreas also works closely with the GI tract by releasing enzymes to process food.
The GI Tract, or gastrointestinal tract in good condition, will process food easily. Bacteria are in order and balanced with the good bacteria consuming the bad, and maintaining a comfortable working system. When a person is unbalanced they may suffer from constipation or the reverse side of the spectrum, diarrhea. They are then unable to absorb nutrients properly that are required for the body to produce energy, or for the vitamins and minerals to fully support the intended organs. Diarrhea also leads to dehydration, causing injury to the liver.
In essence, the metabolic system is in charge of running our entire energy system. The best way for its optimal operations and a healthy digestion process is:
 Due to the importance of the metabolic system for proper functioning of the human body, as described in detail above, it has become a primary focus of anti-aging and is being examined thoroughly from many different aspects to ensure its regulation. In particular, and in the forefront of this article, is its association to menopause, and menopausal metabolic syndrome.
Due to the importance of the metabolic system for proper functioning of the human body, as described in detail above, it has become a primary focus of anti-aging and is being examined thoroughly from many different aspects to ensure its regulation. In particular, and in the forefront of this article, is its association to menopause, and menopausal metabolic syndrome.
The metabolic syndrome itself consists of a combination of factors that cause risk that include hypertension, abdominal obesity, insulin resistance, and atherogenic dyslipidemia, and greatly increases the risk of type 2 diabetes and cardiovascular disease. As will be discussed in more detail, estrogen replacement therapy is often used to improve insulin sensitivity and reduces the risk of the development of diabetes.
The key elements in managing the menopausal metabolic syndrome are weight reduction, increasing physical activity, and diet modification. If blood pressure, lipid and glycemic control are not achieved through these interventions then pharmacological therapy will be required.
In reference to gender, before the age of 50 men have been diagnosed with the syndrome more often. Then after 50, the average of women have an incredible increase of the disease. Menopausal metabolic syndrome also changes one's emotional status as well as their ability to fight against stress, which in itself is a precursor to an abundant amount of illnesses.
 Menopause, also called Climacteric, is classified as a time in a woman’s life when her menstrual period ceases, and she is no longer able to bear children. For many, this is a new type of freedom from monthly periods often ranging from 3-10 days of discomfort and bleeding. This is the opposite of menarche, a time period when a girl’s period begins. The average age for the naturally occurring process of menopause typically occurs between 49 — 52 years of age. Physiologically, menopause happens due to a decrease in the production of the hormones estrogen and progesterone by the ovaries. The woman at this time is considered infertile, and the possibility of her becoming pregnant has been extremely low for a number of years prior to this. These changes affect the metabolic system and can lead to menopausal metabolic syndrome.
Menopause, also called Climacteric, is classified as a time in a woman’s life when her menstrual period ceases, and she is no longer able to bear children. For many, this is a new type of freedom from monthly periods often ranging from 3-10 days of discomfort and bleeding. This is the opposite of menarche, a time period when a girl’s period begins. The average age for the naturally occurring process of menopause typically occurs between 49 — 52 years of age. Physiologically, menopause happens due to a decrease in the production of the hormones estrogen and progesterone by the ovaries. The woman at this time is considered infertile, and the possibility of her becoming pregnant has been extremely low for a number of years prior to this. These changes affect the metabolic system and can lead to menopausal metabolic syndrome.
In summary, menopause is more clearly defined with the following:
Before menopause, a woman’s periods usually become irregular, increasing or decreasing in duration and blood flow. The woman quite often experiences hot flashes ranging from 30 seconds to 10 minutes with associated sweating, reddening of the skin, or shivering. Many women suffer vaginal dryness, sleep problems, and elevated mood swings. Of course, symptoms vary in severity among women.
For those women who have had a hysterectomy, or a removal of their uterus, but they still have their ovaries intact, menopause may have occurred at the time of the operation, or when their hormone levels fell. Following the surgery, symptoms usually occur at an earlier age, an average of 45 years of age.
Menopausal Metabolic Syndrome occurs when the metabolic system is directly affected by menopause. Research has shown that menopausal state is associated with a 60 percent increased risk factor of metabolic syndrome and the fact that by their final period 13.7 percent of women did indeed have newly onset metabolic syndrome. Of course, not all women will develop Menopausal Metabolic Syndrome, but they are at a very high risk to do so.
As is well known in the medical, health and wellness industries, the decrease of estrogen decreases dramatically with menopause and is considered to be a key factor in Menopausal Metabolic Syndrome as well as the underlying and abrupt increases in weight, diabetes, cardiovascular disease risks, elevated blood pressure, low HDL cholesterol, high triglyceride, and abdominal obesity. These are all prevalent among women after menopause. Obesity is the most common disorder associated with women in their menopausal stage and occurs in approximately 65 percent of all women.
 Due to the loss of estrogen, and the increase in androgens, the pathological redistribution of fat from subcutaneous and gluteofemoral regions end up in the abdominal zone.
Due to the loss of estrogen, and the increase in androgens, the pathological redistribution of fat from subcutaneous and gluteofemoral regions end up in the abdominal zone.
Menopausal Metabolic Syndrome predisposes women to cardiovascular disease and Type 2 diabetes, a condition associated with eating too many refined carbohydrates, sugars and fats. Obesity increases in American women by 65 percent between the ages of 40-59, and by 74 percent after the age of 60. In fact, many women have been known to gain 40 pounds with in the two years of beginning menopause, with no changes whatsoever in lifestyle. The hypothalamus gland, which controls obesity, is directly affected by the loss of estrogen and the energy molecules connected to this system. The change in estrogen also affects the central nervous system where food intake is regulated. The menopausal state disrupts the down regulation of food intake, and increases insulin secretion, both leading to fat accumulation. It becomes an imbalance, and a difficult state for the body to accurately handle without proper prevention, knowledge, and care.
Metabolic syndrome also changes one's emotional status as well as their ability to fight against stress, which in itself is a precursor to an abundant amount of illnesses. With this wall down, the body can more easily contract other debilitating syndromes such as adrenal fatigue causing excessive tiredness, difficulty concentrating, insomnia, inability to lose weight, feeling anxious, allergies, and brain fog.
Although the adrenal glands are just two small glands, each about the size of a walnut residing atop the kidneys, their purpose is to help the body cope with stress and help it to survive. You may be especially vulnerable to adrenal fatigue if suffering from menopausal metabolic syndrome. Your adrenal glands are in part responsible for managing your metabolism along with your pancreas, liver, thyroid, and other organs. Metabolic syndrome can put undue stress on your adrenals, forcing them to work overtime to balance your metabolism. Over time, the adrenals can weaken leading to adrenal fatigue.
 With ? of a woman’s life taking place in the menopausal state, it is detrimental to their well being that they are prepared for the changes that their body will be undergoing. Although the science behind it is difficult to the untrained eye, research has brought forth a new understanding into the world when it comes to menopause and metabolic syndrome.
With ? of a woman’s life taking place in the menopausal state, it is detrimental to their well being that they are prepared for the changes that their body will be undergoing. Although the science behind it is difficult to the untrained eye, research has brought forth a new understanding into the world when it comes to menopause and metabolic syndrome.

Lab Work for recognizing menopausal metabolic syndrome is available. Testing all levels of the female hormone profile include: Estradiol, Estrone, Estriol, Progesterone, FSH, SHBG, and Testosterone, is recommended, as well as a comprehensive metabolic panel. If all show up normal, but there is a hormone resistance, the problem is more easily recognizable.
Natural supplementation can help to balance your blood sugar, metabolism and help bring metabolic syndrome under control. These supplements and nutrients have been found to be beneficial:
Alpha lipoic acid, chromium, and vitamin C speed the metabolism system and increase the production of collagen. Glutathione, folic acid, phosphatidyl choline are used for detoxification. When the body starts to lose fat, all the toxins go straight to the blood stream. As an automatic response to protecting the brain, the body starts to fight against the treatment because of toxins.
If you detoxify, you will lose fat easier, the adrenal fatigue treatment will be more beneficial and easier. As the body detoxes, many patients with existing inflammation problems will begin to see a bit of relief. The immune system, in connection with inflammation and detoxification, begins to work more efficiently and can aid not only in the recovery of metabolic syndrome, but in adrenal fatigue, allergies, the NEM stress response system, and many other autoimmune disorders.
In conclusion, when women enter menopause, they have an increased risk for Menopausal Metabolic Syndrome, which not only in itself is life restricting with its correlation to cardiovascular diseases, type 2 diabetes and obesity, but can open the door for many other related health problems. People must learn to adapt to the changes in the body that are brought on by age, illness, or stress, and seek medical guidance.
If a sudden onset of weight gain is noticed, or any menopausal symptoms are recognized, contact a primary care physician immediately to begin the testing and diagnosing procedures.
It must be noted that the aforementioned therapies may not be suitable for everyone, as many people may have intolerances or sensitivities to certain hormones and therapies, or may not be able to digest or process some of the recommended nutritional supplements.
Medical and dietary advice, along with any testing should be obtained prior to beginning any therapy or medications.
While most in normal and good health can tolerate hormone replacement, those already in advanced stages of adrenal fatigue are particularly at risk of negative reactions to treatment. Adrenal crashes may be precipitated. The weaker the adrenals, the greater the risk.
Even post menopause, a woman must continue getting regular check ups and preventative screenings when it comes to her health care such pelvic exams, pap smears, breast exams and mammograms. Preventative care is one of the most important things people can do for themselves for their well-being and longevity. With proper care, education and awareness, youthful aging can be achieved, and the freedom that comes along with menopause can be thoroughly enjoyed.
Yes, new research discovered and documented by Dr. Natalia Chekalska, MD, Ph.D. has indicated that women who enter menopause have an increased risk for developing Menopausal Metabolic Syndrome, and can reduce and prevent the risk of its onset by a combined therapy of BHRTY, Metformin, and nutrition therapy.
"Thank you Dorine, I want you to know that I respect and admire you"
"Thank you Dorine, I want you to know that I respect and admire you and Dr. Lam more than I can ever say. To be sick for decades and then to read your books, especially the AMS 440 pg. has been an incredible, nearly miraculous experience! To realize that you know and understand what I’m going thru is a gift from our creator working mightily through you. Thank you."