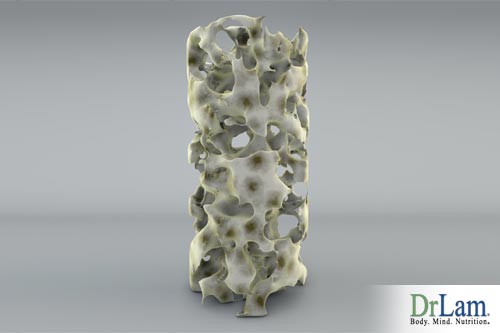
 Recent research has shown a helpful relationships between strontium for osteoporosis. Have you ever thought about using strontium for osteoporosis? Have you ever wondered if strontium for osteoporosis is the right choice for you? Well, if you have these questions or any others concerning the relationship and use of strontium for osteoporosis, keep reading. The word "Osteoporosis" means "porous bones". It is a silent disease that makes bones brittle. If not prevented or left untreated, osteoporosis can progress painlessly until a bone fractures. When essential building block nutrition is balanced, such as calcium and strontium for osteoporosis prevention and treatment, bones are stronger and healthier. The use of strontium for osteoporosis prevention and treatment is not difficult and is a natural option. So, it one less prescription pressuring your pocket and one more way to improve health. Using strontium for osteoporosis may be the answer you have been looking for.
Recent research has shown a helpful relationships between strontium for osteoporosis. Have you ever thought about using strontium for osteoporosis? Have you ever wondered if strontium for osteoporosis is the right choice for you? Well, if you have these questions or any others concerning the relationship and use of strontium for osteoporosis, keep reading. The word "Osteoporosis" means "porous bones". It is a silent disease that makes bones brittle. If not prevented or left untreated, osteoporosis can progress painlessly until a bone fractures. When essential building block nutrition is balanced, such as calcium and strontium for osteoporosis prevention and treatment, bones are stronger and healthier. The use of strontium for osteoporosis prevention and treatment is not difficult and is a natural option. So, it one less prescription pressuring your pocket and one more way to improve health. Using strontium for osteoporosis may be the answer you have been looking for.
There are approximately 1.5 million osteoporosis-related fractures occurring annually in the United States, and over 500,000 of these cases occur in post-menopausal women. Over half of the women over age fifty will have an osteoporosis related fracture in their remaining lifetime and could be helped using strontium for osteoporosis.
Any bone in the body can be affected, but fractures typically occur in the hip, spine, and wrist. A hip fracture almost always requires major surgery as well as hospitalization. More significantly, one in four hip fracture patients over the age of fifty will die within the year following their fracture.
Millions of Americans are at risk for osteoporosis and could potentially use strontium for osteoporosis suffering. An estimated ten million Americans today have osteoporosis and are not even aware of the fact that strontium for osteoporosis prevention is an option. Among those, eight million are women, and two million are men. Risk factors of osteoporosis include alcoholism, gastro-intestinal disorders, kidney stones, smoking, lack of physical activity, low exposure to sunlight, age of menarche, overweight, as well as prolonged use of steroids such as cortisone or prednisone.
Osteoporosis targets more women that men, because of the hormonal cycle. In fact, women are four times more likely than men to develop and suffer from the disease and can lose up to 20% of their bone mass from the first five to seven years following menopause. In the busy days that most women have been breadwinners as well as mothers, using strontium for osteoporosis treatment and prevention is an easy add to a daily routine.
During menopause, bone loss accelerates due to an absolute drop in estrogen levels in the body. This leads to an increase in the resorption (teardown) of the existing bone in the body. There is also at the same time an even more severe drop in the body's production of progesterone, and without an adequate level of progesterone, there is a reduction of new bone formation. This imbalanced state is often termed estrogen dominance, where the relative amount of estrogen in the body post-menopausally is actually higher than before menopause due to the severe reduction in progesterone. Strontium for osteoporosis treatment can work to counterbalance some of the effects and impacts of hormonal imbalance.
For decades, women have been told that taking synthetic hormone replacement therapy (HRT) such as Premarin or Pempro post-menopausally would help to reduce the risk of fractures and slows down the aging process. In a study published in the Journal of American Medical Association, (June 13th, 2001,) a review of 22 previous studies shows that HRT does not bring any benefit to the bones and isn't the best option. For many of you reading this utilizing strontium for osteoporosis may offer a better result and more symptom relief.
Men are also at risk for osteoporosis, although the incidence of fractures is less than that in women. More than two million men in the US have osteoporosis and it is estimated that another three million are at risk and could be utilizing strontium for osteoporosis prevention.
Men over age 50 have a greater risk of developing osteoporosis than they do with prostate cancer, even though prostate cancer is much more publicized. Thus, taking strontium for osteoporosis prevention should be considered by both men and women alike.
While women are four times more likely to get osteoporosis than men, men are more likely to develop an extreme form of the disease, which can result in the loss of height by several inches.
 Osteoporosis is often diagnosed by x-ray or bone density tests. Upon diagnosis, using strontium for osteoporosis can begin immediately. The conventional choice of treatment is the use of a class of drugs called biphosphates and other "designer variations of this class of drugs. One such drug in this class is Fosamax. Fosamaxis made from the same type of chemicals that are used to remove soap scum in your bath tub. Is this really what you want to put into your body or would you prefer a more natural remedy such as strontium for osteoporosis treatment?
Osteoporosis is often diagnosed by x-ray or bone density tests. Upon diagnosis, using strontium for osteoporosis can begin immediately. The conventional choice of treatment is the use of a class of drugs called biphosphates and other "designer variations of this class of drugs. One such drug in this class is Fosamax. Fosamaxis made from the same type of chemicals that are used to remove soap scum in your bath tub. Is this really what you want to put into your body or would you prefer a more natural remedy such as strontium for osteoporosis treatment?
The bone is a living structure, and a constant breakdown and rebuilding of bones is the key to healthy bones. The Osteoclasts are cells that remove old bones, and they work in conjunction with osteoblasts, which are bone-building cells. When this process is in balance, normal bone density is maintained. Fosamax kills the osteoclasts, so only the osteoblasts are left. This is not the way in which strontium for osteoporosis treatment works.
When the bones are not being broken down, bone density will show an apparent increase. However, as times goes on, this will backfire, making strontium for osteoporosis a potentially better option for treatment. As bones become denser due to the lack of breakdown, they actually become weaker, as they have not been allowed to remold themselves and readjust to the constantly changing forces that are applied to the bones. Over time, the rise in bone density slows down, while the risk of fractures actually increases as the bone becomes more brittle. This is not a concern when you utilize strontium for osteoporosis treatment.
In addition, the bipho-sphates drugs may also cause serious inflammation in several regions of the eyes. In a study reported in the New England Journal of Medicine on March 20th, 2003, researchers reviewed thousands of cases in which patients were prescribed bisphosphonates and tracked 314 patients who had also reported to have eye problems. Although side effects were rare, several types of inflammation did occur, leading to the loss of vision and blindness. Other side effects included nausea, heartburn, abdominal pain, muscle cramps, irritability, pain when swallowing, and diarrhea. Aspirin and other non-steroidal, anti-inflammatory drugs such as ibuprofen may also increase the damage to the stomach if taken with Fosamax? These side effects are not ones that you need to worry about when utilizing a natural supplement such as strontium for osteoporosis treatment.
There is little doubt that there is a strong correlation between dietary habits and osteoporosis. So, be supportive of your health by utilizing strontium for osteoporosis and a proper diet. As far back as 1968, research has shown that the amount of minerals in the bones varies with the diet. An excessively high protein diet (particularly animal protein) leads to a negative calcium balance. In other words, there is a net loss of calcium from the body resulting in reduced calcium storage in bones. This is a serious risk for osteoporosis sufferers and an unnecessary one if you utilize strontium for osteoporosis treatment.
When excessive amounts of meat, refined carbohydrates, and fat are consumed into our diet over a long period of time, our body becomes more acidic. The body is not used to this and prefers to be in an alkaline environment most of the time. As a compensatory mechanism, the body directs calcium and other minerals to be removed from the bones and transported to the rest of the body in an attempt to buffer and neutralize this acidic environment. Some of this calcium goes into the kidney and is excreted out. As a result, there is a net loss of calcium from the body.
 In addition to the loss of calcium from the bones, animal proteins, due to the high sulfur content, alter the kidney's re-absorption of calcium, so that more calcium is excreted. Those on high protein diets such as meat and dairy products can lose about 100 mg of calcium a day. In one study, individuals who consumed excessive amounts of protein were found to have a negative calcium balance of 137mg/day. This translates into approximately 50g/year and a potential skeletal mass loss of 4% per year.
In addition to the loss of calcium from the bones, animal proteins, due to the high sulfur content, alter the kidney's re-absorption of calcium, so that more calcium is excreted. Those on high protein diets such as meat and dairy products can lose about 100 mg of calcium a day. In one study, individuals who consumed excessive amounts of protein were found to have a negative calcium balance of 137mg/day. This translates into approximately 50g/year and a potential skeletal mass loss of 4% per year.
A major concern of those who have been advised to stop drinking milk is, "What will happen to my teeth and bones?" The answer is astoundingly simple, "They will improve."
In researching the effects of strontium for osteoporosis, t is very important to comprehend the realtionships and effects of lifestyle and habits on the body. The majority of the world's population takes in less than half the recommended daily calcium intake of 800 mg a day and yet they have strong bones and healthy teeth. The notion that continuous ingestion of high amount of calcium is needed in order to maintain strong bones and prevent osteoporosis must be dispelled. Studies have repeatedly shown that strong bone is due more to a function of ptimum amount of magnesium and a low acidic environment in the body rather than calcium from a nutrient perspective.
While milk provides calcium, it is ironic that milk also promotes calcium loss in the body. You need calcium to prevent bone damage, and strontium for osteoporosis prevention if you have been consuming larger amounts of milk. This is because the consumption of the excessive proteins found in cow's milk increases the need for minerals found in the body to neutralize the acid formed from digesting the animal protein in cow's milk. Such minerals include calcium and magnesium and 99 percent of the body's calcium and 60 percent of the body's magnesium is stored in the bone. As mentioned before, calcium is removed from the bone to the blood in order to neutralize the acid, resulting in the loss of calcium from the bone. In fact, calcium excretion and bone loss increase in proportion to the amount
In short, milk and dairy products are acid forming substances. Acidic byproducts that accumulate in the body is also one of the primary reasons of accelerated aging and cancer. It is best that our body be bathed in a slightly alkaline environment. A diet high in milk, meat, and poultry means that, more protein is ingested, and the more acidic the body becomes. Vegetarians, for example, need about half as much calcium as meat eaters as they lose much less calcium from their bones.
Cow's milk also contains phosphorous. When calcium and phosphorus reach the intestine at the same time, they compete for absorption. The more phosphorus there is, the less calcium will enter the body. Some phosphate compounds form insoluble calcium salts in the intestine. In addition, excess phosphorus triggers the release of parathyroid hormone, which sucks calcium out of the bones. When combined with calcium, phosphorus also competes with and prevents calcium absorption in the intestine. This is something that must be combatted and utilizing strontium for osteoporosis treatment can help.
 The higher phosphorous level found in animal food (as compared to plant food) may also interfere with calcium absorption. Phosphorous is an important component in a balanced nutritional program, but it may bind with calcium and therefore reduce the amount of calcium that is absorbed by the body. Plant-based foods have protein but contains a lower calcium -phosphorous ratio.
The higher phosphorous level found in animal food (as compared to plant food) may also interfere with calcium absorption. Phosphorous is an important component in a balanced nutritional program, but it may bind with calcium and therefore reduce the amount of calcium that is absorbed by the body. Plant-based foods have protein but contains a lower calcium -phosphorous ratio.
Not all calcium in food enters the body. Many components of food such as phosphates, vitamin D, fiber, proteins, and hormones alter the absorption of calcium in our diet. For example, Cow's milk contains 1,200 milligrams of calcium per quart; human milk contains only 300 milligrams. But the total calcium absorbed in breastfed babies is higher than in babies fed cow's milk. This is because the phosphates and palmitic acid in cow's milk reduce the absorption of calcium by the body.
The optimum calcium/phosphorus ratio is important for bone building. The ideal ratio is 2.5 to 1. Too much phosphorus consumed will upset the balance, and will lead to a progressive bone loss in the body. The ratio in cow's milk is only 1.3 to 1.
In addition, milk consumption is not helpful in improving bone density for those over 30 years old, because the milk has been pasteurized. The pasteurization process causes a severe destruction of essential nutrients.
In a discussiong about strontium for osteoporosis, as mentioned before, a diet must be evaluated. As more Americans turn to the low-carb, high protein diet to lose weight quickly, some research studies are reporting that such diet can increase the risk of kidney stones as well as the risk of osteoporosis. In a six-week study reported in the American Journal of Kidney Disease in 2002, ten healthy adults consumed a regular diet for two weeks, followed by a low-carb, high protein diet for two weeks, and finally followed by a moderately restricted carbohydrate diet for four weeks. It was found that while the volunteers lost nine pounds on average, most developed ketones. These ketones raise the acid level in the blood, and some volunteers had their acid level increased by 90%. There is also an increase of calcium being lost in the urine by the volunteers. Protein is a source of acid and produces an acidic environment in the body. The body simply does not like this. When exposed to a high acidic environment, the body tries to buffer or neutralize the acid by withdrawing minerals such as calcium from the bones. As such, the body's calcium stored in the bones is therefore reduced.
The kind of vegetables that is good for osteoporosis prevention include leafy vegetables, legumes, raw nuts ( that have been pre-soaked overnight in water), and seeds. All these contain plentiful amounts of calcium. It has been shown that the average African women only consumes only 500mg of calcium a day, and mostly from plant sources. However, they have a positive calcium balance because they retain their calcium much better.
The key is to control the protein level and thus maintain an environment that is not overly acidic in the body. When protein intake is reduced to a modest level, and especially if the protein can be derived from plant sources, excessive calcium intake to compensate for the calcium lost is not necessary. The level of calcium intake can further be reduced if it is combined with magnesium and strontium, both facilitators of calcium transport.
 Soy is high in phytoestrogen, a plant estrogen precursor. The effect of soy in the body is still controversial, but many experts believe that soy blocks excessive estrogen from being absorbed and acts like estrogen when it is deficient, thus providing the best of both worlds.
Soy is high in phytoestrogen, a plant estrogen precursor. The effect of soy in the body is still controversial, but many experts believe that soy blocks excessive estrogen from being absorbed and acts like estrogen when it is deficient, thus providing the best of both worlds.
Interesting studies have been conducted, including one from Italy involving 90 women age 53-65. It was found that ipriflavone and calcium supplementation was able to increase bone mineral density by 2% after 6 months and 5.8% after 12 months with the added bonus of significant decrease in pain-45% in 6 months, and 62% at 12 months. However, it should be noted that soy does have a dark side. Excessive amounts of unfermented soy intake such as tofu can lead to thyroid disturbances. Women who are in post-menopausal period should therefore be careful when using soy as a supplementation for osteoporosis. Fermented soy products such as miso or tempeh do not have this problem and can be taken liberally.
Avoid stimulatory drinks that contains caffeine which acidifies the body and causes calcium to be withdrawn from the bone. Avoid coffee and tea. Distilled water should also be avoided. Decaffeinated coffee and decaffeinated tea are acceptable in moderate amounts. Herbal tea is acceptable.
Weight bearing exercises is as close as one can get when one is searching for a magic bullet in the prevention of osteoporosis. The positive effect of exercise on bone density is greatest in adults who have been sedimentary and just started exercising. Studies have shown that even elderly adults over age 80 who have done active exercise and weight bearing programs can significantly increase their bone density over a short period of time. Weight-bearing exercises such as walking, running, jogging, dancing, are especially important. While swimming is a great exercise for cardiovascular diseases, it is not as good for bone health when compared to walking and jogging.
Bone is alive tissue and it responds to stress placed upon it. In a positive way when a person becomes sedimentary, the normal stress placed on the bones is removed. The bone will lose its density and become brittle over time. It comes as no surprise that a patient with spinal cord injuries will have significant loss of bone density if proactive steps are not taken. The opposite is also true; athletes have stronger bones than the average adult.
Exercise is a lifelong activity. Its effect on bone mass will decrease when one stops to exercise. Therefore, exercise needs to be done on an ongoing basis. 30 minutes of weight bearing exercise daily will improve bone density, heart health, muscle strength, coordination, and balance. The good news is that studies have now shown that the 30 minutes of exercise can be broken down into ten-minute blocks without sacrificing results.
 Remember to warm up and cool down always. It is also wise to combine several different kinds of weight bearing exercises. Incorporate exercises that build strength, and increase resistance in weight to the program. Lastly, drink plenty of water to prevent dehydration.
Remember to warm up and cool down always. It is also wise to combine several different kinds of weight bearing exercises. Incorporate exercises that build strength, and increase resistance in weight to the program. Lastly, drink plenty of water to prevent dehydration.
Fifty years ago, nutritional supplementation for bone building involves primarily around the single element calcium. Later, it was found that magnesium and vitamin D are important components as well. The latest nutritional research now points to three other important team players ?strontium, vitamin K, and collagen.
Bone building is no longer about any one single nutrient. The best program consists of a cocktail with all six nutrients working concurrently.
Calcium is a basic building block of bones. The average adult has about 3 lbs of it in their bones, teeth, and blood. The use of calcium supplementation to treat post menopause osteoporosis has increased significantly since 1987, which is the year the National Institute of Health increased the recommended daily intake of calcium to 1500mg for the prevention of primary post-menopausal osteoporosis (PPMO). There is significant controversy surrounding this recommendation because working it was made despite the conflicting conclusions research by some clinical studies presented to the NIH. Some of the studies show no significant effect of calcium intake on mineral density on the trabecular bone and only a slight effect on the cortical bone. Since PPMO is predominantly a condition due to the demineralization of the trabecular bone, there is no justification for calcium mega dosing for postmenopausal women. In fact, soft tissue calcification can be a serious risk factor arising from calcium mega dosing under certain conditions. Most research and trials using calcium in the prevention of post-menopausal osteoporosis also involve the use of vitamin D and this makes it difficult to attribute the benefit to calcium alone.
It is also interesting to note that the bone density increase found in the first two years of calcium supplementation may not substantially increase over a long period of time. In contrast to most clinical data, a great number of studies did not find a significant association between calcium intake and a reduced risk of bone loss fracture. It is well known that calcium at low or moderate doses is largely dependent on the action of vitamin D for active support. Sufficient amount of Vitamin D is important for the prevention of post-menopausal bone loss. Insufficient vitamin D leads to less calcium absorption, the elevated blood concentration of parathyroid hormone, as well as an increased rate of bone absorption. All these can eventually lead to a bone fracture if not corrected in time.
The conventional wisdom and recommendation taken for granted is that a high dose of calcium is necessary for the prevention of post menopausal osteoporosis, as well as for the building of strong bones for children and elderly. Long term studies, however, have not been able to confirm that calcium alone can get the job done without the help of other nutrients especially in the case of PPMO.
 Current Recommended Dietary Allowance (RDA) is 1000 mg of calcium for younger adults, and 1200 mg for people over the age of 50.These numbers reflect the total calcium needed for a diet that is high in protein and fat (typical of the young American diet). Such diet also produces a body that is acidic and as a result, calcium is drawn out of the bones to neutralize this acidic environment in order to return the body to a more alkalized state. A high calcium intake of more than 1000 mg or more is suggested for anyone who falls into this demographic group that takes in a diet high in protein.
Current Recommended Dietary Allowance (RDA) is 1000 mg of calcium for younger adults, and 1200 mg for people over the age of 50.These numbers reflect the total calcium needed for a diet that is high in protein and fat (typical of the young American diet). Such diet also produces a body that is acidic and as a result, calcium is drawn out of the bones to neutralize this acidic environment in order to return the body to a more alkalized state. A high calcium intake of more than 1000 mg or more is suggested for anyone who falls into this demographic group that takes in a diet high in protein.
This recommendation of 1000 to 1500 mg calcium is not suitable in the case of postmenopausal osteoporotic women whose diet is likely to be high in green leafy vegetables. In this type of diet, the amount of calcium required in terms of supplementation is much reduced. If you have a high calcium intake from food source, then less supplemental calcium will be needed. As well, a diet high in green leafy vegetables leads to an alkaline internal environment. The body will not have a need to withdraw calcium from the bone required. As a result, only 500 mg is required if
Mega-dosing of calcium in excess of 1000 mg per day has little correlation with an increase in bone density. In fact, taking too much calcium can inhibit the absorption and utilization of other important bone nutrients, such as zinc and copper. In fact, mega-dosing of calcium can be detrimental to your health, leading to the extra cellular deposit of calcium and eventual formation of bone spurs. Excess calcium also can serve as a cardiac irritant and can lead to cardiac arrhythmias.
Multiple studies have shown that calcium supplements - such as calcium gluconate, calcium citrate, calcium carbonate, and even calcium citrate-malate - slow, but do not halt or reverse, menopausal bone loss, whether taken alone or with vitamin D. Even a total daily calcium intake of 3000 milligrams of calcium alone isn't enough to stop bone loss. The bone will not be able to take in more calcium than it is capable of if other supporting nutrients are not present. An osteoporosis program focusing largely on calcium intake is a recipe for failure.
Metabolic Typing and Calcium
Metabolically, most people can be divided into three types. Protein, carbohydrates (carbs), and mixed (a combination of carbs and protein). Certain metabolic types naturally require a higher amount of calcium in their diet in order to function at their best. They tend to have sufficient synergistic nutrients but lack sufficient amounts of calcium. Other metabolic types are the opposite. These types tend to already have high levels of calcium in their body and are low in synergistic nutrients. They do well in diets that are relatively low in calcium and high in other synergistic nutrients. By simply overloading one's body with mega doses of calcium may make things worse.
 Generally speaking, protein types are fast oxidizers and are autonomically parasympathetically driven. These people require large amounts of calcium to normalize their acid-base balance. On the other end of the spectrum, those who are in the carb groups are slow oxidizers and are sympathetically driven (they respond in a different way). Therefore when the carb types receive calcium, their pH and acid-base balance get considerably worse. This may be one reason that helps to explain the observation that calcium does not seem to be associated with reducing bone fractures in all people.
Generally speaking, protein types are fast oxidizers and are autonomically parasympathetically driven. These people require large amounts of calcium to normalize their acid-base balance. On the other end of the spectrum, those who are in the carb groups are slow oxidizers and are sympathetically driven (they respond in a different way). Therefore when the carb types receive calcium, their pH and acid-base balance get considerably worse. This may be one reason that helps to explain the observation that calcium does not seem to be associated with reducing bone fractures in all people.
Calcium can be found in vegetables and milk. Traditionally, milk is consumed, but it is not helpful in improving bone density as it is pasteurized. Raw milk on the other hand, is very different and beneficial, but not everybody has access to this, however.
You can get an ample supply of calcium from green leafy vegetables. Supplementation with calcium is an easy and inexpensive way to assure that you get enough. About 500 mg of calcium a day is all that is needed for strong bones, provided that you also take 500 mg of Magnesium and follow a diet ample in green leafy vegetables. The ratio of magnesium to calcium should be one to one (1:1) or even two to one (2:1) for strong bones, according to many researchers who are in the forefront of anti-aging medicine. Over 80% of adults in America do not consume even the 300 mg of magnesium recommended. While there is no harm in an excessive amount of magnesium being consumed, some people do develop harmless diarrhea.
How Much to Take?
A recent study made by the National Institute of Health supports the notion that, starting at childhood, an adequate amount of bone reserve needs to be built up in order to have it for the future. As such, a high dose of calcium intake of 800 mg for children from years 3-8 and 1300 mg for those between 9-17 is suggested.
From age 18 onwards, the use of high-dose calcium above 1500 mg is only indicated if the diet is high in meat (leading to an acidic body). Only 500 mg is required if the diet is high in vegetables (leading to an alkaline body), and excessive calcium intake can, in fact, cause more harm than good. The blanket recommendation of high doses of calcium (over 1000mg )after adulthood regardless of diet or metabolic type, should be abandoned.
Nutritional Consideration : 500 mg of calcium in a diet high in green leafy vegetables. The calcium intake should be increased up to 1500 mg a day if the diet is high in meat and protein.
Magnesium acts as a balancer of calcium in our body, much like progesterone balances the effect of estrogen, and omega-3 balances omega-6 fatty acids.
 Magnesium balances the body's calcium supply and keeping it from being excreted. Without magnesium and other trace minerals, calcium ingested, especially if excessive, will be deposited not in the bone but perhaps in the wall of our arteries.
Magnesium balances the body's calcium supply and keeping it from being excreted. Without magnesium and other trace minerals, calcium ingested, especially if excessive, will be deposited not in the bone but perhaps in the wall of our arteries.
It is interesting to note that human autopsy studies have shown a close correlation between osteoporosis and abdominal aortic calcification. Since magnesium deficiency can promote osteoporosis and calcium deposit in the aorta, logic dictates that magnesium is likely to be the primary factor and that calcium is secondary when it comes to the prevention of bone loss.
Magnesium regulates the active calcium transport. It has been shown that magnesium has fracture prevention effect, and is able to increase bone density when taken on an ongoing basis. Magnesium deficiency has been shown to be a significant risk factor for post-menopausal osteoporosis, and this may due to the fact that magnesium deficiency alters calcium metabolism and the hormones that regulate calcium.
Magnesium has been shown to prevent the formation of calcium oxalate crystals, the most common cause of kidney stones. Studies have shown that 500 mg a day of magnesium is able to reduce the recurrence rate of kidney stones by as much as 90%. Magnesium is also nature's "calcium channel blocker", preventing the entry of excessive calcium into the cell resulting in contractions, chest pain, hypertension, and arrhythmias. Magnesium deficiency can cause various abnormalities of calcium metabolism, resulting in the formation of calcium deposits in arteries. Osteoporotic women who were deficient in magnesium had abnormal calcium crystals in their bones, whereas osteoporotic women with normal magnesium status had normal calcium crystals in their bones.
One researcher, Dr. Guy Abraham, postulated that a dietary program emphasizing magnesium as well as calcium for the management of PPMO would be more effective in preventing bone loss. His concern for low magnesium for osteoporosis is similar to his concern for women with premenstrual tension syndrome. To test Dr. Abraham's hypothesis, 19 post-menopausal women on hormone replacement therapy were given a supplement consisting of 500mg of calcium (50% of RDA), and 600mg of magnesium (200% of RDA). Studies were conducted every 3 months. Subjects receiving the treatment showed an 11% increase in bone density versus 0.7% in the untreated group. Results also showed that in post-menopausal women on hormone replacement therapy, the magnesium emphasized program was able to produce calcaneus bone density 16 times greater than that of the dietary advice alone. At the start of the study, 15 subjects were below the fracture threshold. After a year of treatment with magnesium supplementation, in conjunction with calcium supplementation, only 7 of them were below the fracture threshold.
Researchers such as Dr. Abraham postulate that PPMO is predominantly a skeletal manifestation of chronic magnesium deficiency facilitated by estrogen withdrawal during the post-menopausal period. He suggests raising the RDA of magnesium to 1000mg a day and lowering the RDA of calcium to 500mg a day. This suggestion is more in line with the World Health Organization?(practical allowance)?
Nutritional Consideration: 500 mg magnesium.
 Vitamin K is an essential nutrient, best known for its role in blood clotting. There is significant emerging evidence that vitamin K plays a protective role in fighting age related bone loss.
Vitamin K is an essential nutrient, best known for its role in blood clotting. There is significant emerging evidence that vitamin K plays a protective role in fighting age related bone loss.
There are three types of Vitamin K. The primary source of Vitamin K is phylloquinone, and can be found in green vegetables and certain plant oils. Vitamin K2, also called menaquinone, is made by the bacteria that line the gastrointestinal tract of our body.
Osteocalcin is a protein that is produced by the osteoblast. This chemical is utilized within the bone and is an integral part in the process of bone formation. Before osteocalcin can be used, it has to be carboxylated and Vitamin K functions as a cofactor for the enzymes that catalyzes the carboxylation of osteocalcin.
Numerous studies have now shown that people with the lowest intake of vitamin K have a higher chance of hip fractures than those who have higher intakes of vitamin K. This was the conduction of the "nurse health study?conducted by Harvard Medical School. Another study involving 800 elderly men and women followed the Framingham Heart Study for 7 years found that people with the highest vitamin K intake only has 35% of the risk of hip fracture experienced by those with the lowest dietary intake of vitamin K. In fact, vitamin K has been approved for the treatment of osteoporosis in Japan since 1995.
Recent studies on Vitamin K have been impressive. 72 osteoporotic women taking a first-generation bisphosphonate drug called Didronel for two years was compared to those taking vitamin K for the same period of time. There was no difference found in the bone fracture rates between women taking vitamin K and those taking the bisphosphonate drug for osteoporosis.
In fact, vitamin K has the additional benefit of being a protector of our cardiovascular system as well as fighting cancer. One study published in the September 2003 issue of International Journal of Oncology found that lung cancer patients treated with vitamin K2 were able to show the growth of cancer cells.
Vitamin K can be found naturally from a variety of foods including collar greens (440mcg/100g), spinach (380mcg/100g), salad greens (315mcg/100g), Kale (270mcg/100), broccoli (180mcg/100g), Brussels sprouts (177mcg/100g), olive oil (55mcg/100g) green beans (33mcg/100g), and lentil (22mcg/100g). Unfortunately, you have to eat more than a pound of green leafy vegetables per day just to get enough vitamin K into your diet.
Vitamin K supplementation should not be taken by those on blood thinner, pregnant or nursing mothers beyond the RDA recommendation of 65mcg unless monitored by a health care professional.
Those who have experienced strokes and cardiac arrest, as well as those who are on blood thinning medication, should also consult their physicians first before taking vitamin K. Those living in the modern day world may already have a vitamin K deficiency brought on primarily by environmental as well as lifestyle factors and not knowing it. Many prescription drugs and antibiotics such as penicillin, tetracycline, warfarin, deplete this valuable vitamin. Other causes of vitamin K deficiency include smoking, excessive use of alcohol and caffeine, chemotherapy, x-rays, frozen foods, aspirin, air pollution, lactose intolerance. Unfortunately, most multivitamins do not contain any vitamin K at all.
Both Vitamin K1 and K2 are safe, natural, and needed for strong bones. Vitamin K3, or menadione, is a synthetic form that is manmade in the laboratory. Only Vitamin K1 and K2 are recommended from a nutritional supplementation perspective.
Nutritional Supplement Consideration: K1 and K2 blend: 1000 mcg day. Take with food is best.
 Vitamin D, calciferol, is a fat soluble vitamin. It is found in food and can also be made in the body after exposure to ultra-violet rays from the sun. If you are exposed to the sun for more than 40 minutes a week, your body is able to produce the needed Vitamin D.
Vitamin D, calciferol, is a fat soluble vitamin. It is found in food and can also be made in the body after exposure to ultra-violet rays from the sun. If you are exposed to the sun for more than 40 minutes a week, your body is able to produce the needed Vitamin D.
Vitamin D prevents rickets in children and osteomalacia in adults. In the US, fortified food is the major source of Vitamin D. Exposure to sunlight is an important source. Sunscreen with sun protection factor (spf) of 8 or greater will block the UV rays that causes the body to produce vitamin D. Vitamin D supplementation is therefore recommended.
Season, latitude, time of day, cloud cover, smog, and sunscreens affect UV ray exposure. For example, in Boston, the average amount of sunlight is insufficient to produce a significant amount of vitamin D synthesis in the skin from November through February.
Vitamin D supplements are often recommended for exclusively breast-fed infants because human milk may not contain adequate vitamin D.
Fortified foods are the major dietary sources of vitamin D. Prior to the fortification of milk products in the 1930s, rickets (a bone disease seen in children) was a major public health problem in the United States. Milk in the United States is fortified with 10 micrograms (400 IU) of vitamin D per quart, and rickets is now uncommon in the US.
Vitamin D actually exists in several different forms and each has its own activities. The main biological function of vitamin D is to maintain normal blood levels of Calcium and Phosphate. Vitamin D helps the absorption of Calcium, and without the proper amount of it, calcium is not able to do its job.
Having a normal level of vitamin D in the body helps the bones to be strong. Vitamin D deficiency has been associated with greater incidences of bone fracture, and severe deficiency leads to rickets and osteomaliacia. . Vitamin D deficiency has also been associated with obesity, auto-immune disease, fatigue, depression, arthritis, heart disease, as well as metabolic syndrome. Steroids may impair the vitamin D metabolism, further contributing to the loss of bone and the development of osteoporosis.
Nutritional Supplement Consideration: 600 IU/day.
Strontium is an essential element with an elemental number of 38 in the periodic table. Using strontium for osteoporosis prevenention may be what you have been searching for. It was discovered in 1808 and is one of the most abundant elements on earth. In fact, there is more strontium in the earth crust than there is carbon. It is also the most abundant trace mineral in seawater. Strontium is not a new element to us. In the body, but strontium for osteoporosis is a newer concept. strontium tends to accumulate in bones where the remodeling process is actively taking place.
 Its properties are quite similar to those of calcium, and in fact, strontium is located in the same column as calcium in the periodic table. Research has long suggested that it may be an essential nutrient required for the normal development of bone structure and skeletal system. Like calcium, strontium has 2 positive charges in its ionic form. Because of its structural similarity to calcium, it can replace calcium to some extent in various biochiemical processes in the body. A small portion of calcium in hydroxyapatite crystals of calcified tissues such as bones and teeth can be replaced with strontium.
Its properties are quite similar to those of calcium, and in fact, strontium is located in the same column as calcium in the periodic table. Research has long suggested that it may be an essential nutrient required for the normal development of bone structure and skeletal system. Like calcium, strontium has 2 positive charges in its ionic form. Because of its structural similarity to calcium, it can replace calcium to some extent in various biochiemical processes in the body. A small portion of calcium in hydroxyapatite crystals of calcified tissues such as bones and teeth can be replaced with strontium.
Strontium is a very strong mineral. Not only does it add strength to the calcium, it also is able to draw extra calcium into the bones and thus facilitate the movement of calcium into the bones.
Clinical trials on the use of strontium and osteoporosis have been conducted since the 1940s. Unfortunately, there was a significant amount of bad press given to this mineral in the late 50s. At that time, it was confused with another form called strontium-90, which is a very dangerous and radioactive component of nuclear fallouts produced during the testing of nuclear weapons in the mid-50s. Strontium-90 is radioactive and has cancer-causing abilities. Stable elemental strontium, on the other hand, is non-radioactive and non toxic even when given in large doses over a long period of time. In fact, it is one of the most effective substances for the treatment and prevention of osteoporosis. Interestingly, the non-radioactive form of strontium can compete with the radioactive form and in fact displaces the radioactive form of strontium in the bodies of those who have an overload of radioactive strontium.
One of the most significant studies was conducted in 1959. Researchers administered a dosage of 1.7g of strontium lactate a day to 32 osteoporosis patients. It was found that 84% of the patients reported significant relief of bone pain. The remaining 16% reported moderate improvement. There were no side effects. Due to the rudimentary and crude measurement of bone mass back in the late 50s, extensive objective data was not able to be carried out. Numerous studies have been done since with the administration of strontium to rats. In1986, it was shown that an administration of 0.27% strontium to mice in their drinking water resulted in an increased rate of bone formation, and a decrease in the bone resorption. Dr. Stanley Skoryna of McGill University in Montreal conducted a small-scale study in 1985 in the use of strontium for the treatment of humans with osteoporosis. A total of 6 subjects, 3 women, and 3 men, were given 600-700 mg of strontium carbonate. Bone biopsies were taken before and after 6 months of treatment. The study showed a 172% increase in bone formation after strontium therapy. There is no change in the bone absorption. Interestingly, the patients receiving strontium reported a reduction in bone pain.
 Recently, the use of strontium in the form of strontium ranelate for the prevention and treatment of postmenopausal osteoporosis was carried out. One study had 353 osteoporosis women with at least 1 vertebral bone fracture and low lumbar bone density score. The subjects received a placebo or strontium ranelate in doses of 170, 340, 680mg a day for 2 years. It was shown that there was a significant positive change in bone metabolism and a reduction of vertebral fracture in the second year of the group receiving 680mg a day. There is little doubt that strontium ranelate therapy is able to increase hip bone mineral density and reduce the incidence of vertebral fracture.
Recently, the use of strontium in the form of strontium ranelate for the prevention and treatment of postmenopausal osteoporosis was carried out. One study had 353 osteoporosis women with at least 1 vertebral bone fracture and low lumbar bone density score. The subjects received a placebo or strontium ranelate in doses of 170, 340, 680mg a day for 2 years. It was shown that there was a significant positive change in bone metabolism and a reduction of vertebral fracture in the second year of the group receiving 680mg a day. There is little doubt that strontium ranelate therapy is able to increase hip bone mineral density and reduce the incidence of vertebral fracture.
Another large study of 1649 osteoporotic, postmenopausal women showed that those receiving 2gram a day of strontium renalate (providing 680mg together with calcium and Vitamin D) suffered fewer fractures of up to 49% risk reduction in the first year of treatment and 41% over the 3 year period. There was an average increase in bone density of 14.4% in the lumbar zone as well as an 8.3% increase in the femoral neck area.
Strontium has also been used to treat patients with a metastatic cancer that has spread to the bones, using a dose as low as 274mg a day. In addition, Strontium has reduced the incidence of cavities. In a 10-year study, the United States Naval conducted an examination of 270,000 naval recruits and found that only 360 were completely free of cavities. Curiously, 10% of those came from a small area in Ohio, where the water has an unusually high concentration of strontium. There have also been studies done in animals showing that the administration of strontium reduces the incidences of cavities.
Strontium in doses of up to 1.5g a day appears to offer a safe and cost-effective approach in preventing and reversing osteoporosis. Most of the studies done, show strontium for osteoporosis prevention to be effective, and involved dosage of 680mg per day. Although most of the recent studies use strontium renalate, early studies used other forms of strontium including strontium carbonate, strontium lactate, and strontium gluconate. It is clear that the active ingredient is strontium and not the salt. The salt used is not as important when compared to the amount of actual strontium consumed.
Because of the similarity in structure and physical properties of strontium and calcium, a few researchers question whether strontium should be administered together with calcium to avoid the possibility of both calcium and strontium competing for the same bone building sites. Yet this does not change the fact that strontium for osteoporosis has been found effective. While this appears to be a theoretical possibility, clinical data have not been able to conclusively demonstrate such problem. Furthermore, the presence of strontium may actually facilitate the transport of calcium into the bones. Research in this area is still ongoing. Suffice to say that from what we know at this time, strontium is an important part of any bone-building program.
Nutritional Supplement Consideration: class="articleboldred">1100 mg of Strontium Carbonate, yielding at least 680 mg of elemental strontium.
 Collagen is the most abundant and most important protein in the body. Protein is abundant in all living creatures. It forms an integral part of the body's organs. It is especially important for bones and joints. Bone has a high amount of collagen. Approximately 90% of the organic matrix of bone is Type I collagen, cross-linked to increase strength and rigidity. Collagen derivatives are formed by cross-linking lysine and hydroxyl-lysine residues in mature collagen and elastin. Collagen acts as an external fiber that wraps around the bone matrixes to increase the tensile strength of the bone matrix. Without an adequate amount of collagen, bone strength is weakened. Osteoporosis depletes both calcium and collagen from the bones.
Collagen is the most abundant and most important protein in the body. Protein is abundant in all living creatures. It forms an integral part of the body's organs. It is especially important for bones and joints. Bone has a high amount of collagen. Approximately 90% of the organic matrix of bone is Type I collagen, cross-linked to increase strength and rigidity. Collagen derivatives are formed by cross-linking lysine and hydroxyl-lysine residues in mature collagen and elastin. Collagen acts as an external fiber that wraps around the bone matrixes to increase the tensile strength of the bone matrix. Without an adequate amount of collagen, bone strength is weakened. Osteoporosis depletes both calcium and collagen from the bones.
Nutritional Supplement Consideration: 500 mg to 5,000 mg of mixed blend including Collagen Type 1 and 3. Also take synergistic nutrients that enhances collagen production including L-lysine, L-proline, citrus bioflavonoids, pine bark extract, and L-carnitine.
There is only one compound that we currently know of that will increase bone strength and density by promoting the growth of osteoblast, and this is natural progesterone. The use of natural progesterone to treat osteoporosis was pioneered by Dr. John Lee, who suggested that osteoporosis in women is due to the decreasing level of progesterone and not estrogen. Dr. Lee's research points out that most women over 65 still have adequate estrogen to inhibits bone loss (though not enough to cause ovulation). But at the age of approximately 35, the body's progesterone production decline drastically. That is also the age of peak bone production in women. After that, it declines. By age 50, the body's progesterone level is extremely low.
.The efficacy of natural progesterone is verified by a three-year study of 63 post-menopausal women with osteoporosis. Women using transdermal progesterone cream experienced an average 7-8% bone mass density increase in the first year, 4-5% the second year, and 3-4%, the third year. The untreated women in this age category typically lose 0.7- 2% bone density per year. The impact of this density loss can be counterbalanced by strontium for osteoporosis prevention and treatment.
Nutritional Supplement Consideration:
Women (Postmenopausal): 20 mg of USP Natural Progesterone a day for 25 days a month
Women (Pre or Peri-menopausal): 20 mg of USP Natural Progesterone a day for Day 14-28 of a 28-day cycle.
Men: 5 mg of USP Natural Progesterone a day everyday of the month.
 Osteoporosis is not a debilitating disease if one starts on the prevention protocol, such as using strontium for osteoporosis treatment quickly, as early as age 35, the time when bone loss starts to become significant. From a diet perspective, one that is high in alkaline and base is preferred to an acidic body causes minerals to be bleached out of the bones in most cases. Weight bearing exercises have repeatedly been proven to be important for stimulating osteoblasts and bone formation. From a nutritional perspective, a cocktail consisting of the right balance of calcium, magnesium, and vitamin D is important. Along with these foundational building blocks, Vitamin K, strontium and collagen will synergistically help the bone formation. Natural progesterone cream should also be considered to round out the program. If you really want to change your life and booste your future health follow theses guidlines below and use strontium for osteoporosis prevention.
Osteoporosis is not a debilitating disease if one starts on the prevention protocol, such as using strontium for osteoporosis treatment quickly, as early as age 35, the time when bone loss starts to become significant. From a diet perspective, one that is high in alkaline and base is preferred to an acidic body causes minerals to be bleached out of the bones in most cases. Weight bearing exercises have repeatedly been proven to be important for stimulating osteoblasts and bone formation. From a nutritional perspective, a cocktail consisting of the right balance of calcium, magnesium, and vitamin D is important. Along with these foundational building blocks, Vitamin K, strontium and collagen will synergistically help the bone formation. Natural progesterone cream should also be considered to round out the program. If you really want to change your life and booste your future health follow theses guidlines below and use strontium for osteoporosis prevention.
Based on a diet high in above the ground vegetables, the key osteoporosis prevention nutritional cocktail for those over 35 years of age should contain the following and to be taken on a daily basis with meals:
Calcium blend (carbonate, hydroxyapatite, and citrate): 500 mg. (Calcium may be increase to 1000-1500 mg if the diet is high in meat and protein)
Magnesium: 500 mg
Strontium Carbonate: 1100mg (yielding 650 mg of elemental strontium)
Vitamin K1 and K2 blend: 1000 mcg
Vitamin D3: 600 I.U.
Vitamin C: 145 mg
Collagen Type 1 and 3: 500 mg
L-Lysine: 150 mg
L-Proline: 50 mg
N-acetyl-cysteine: 100 mg

strontium for osteoporosisk
