
 Those who are in the sub-clinical phase (age 35-45) and clinical phase of aging (age 45 and above) have a one in three chance of getting this syndrome and not knowing it. It’s extremely common, but hardly anyone knows what it is. Some of the symptoms are more recognizable such as feeling mentally and physically sluggish after a meal or gaining weight and struggling to lose it. If your blood pressure creeps up year after year and your blood cholesterol, triglycerides, and blood sugar levels are doing the same, then you may be the victim of Metabolic Syndrome.
Those who are in the sub-clinical phase (age 35-45) and clinical phase of aging (age 45 and above) have a one in three chance of getting this syndrome and not knowing it. It’s extremely common, but hardly anyone knows what it is. Some of the symptoms are more recognizable such as feeling mentally and physically sluggish after a meal or gaining weight and struggling to lose it. If your blood pressure creeps up year after year and your blood cholesterol, triglycerides, and blood sugar levels are doing the same, then you may be the victim of Metabolic Syndrome.
Metabolic syndrome is a very common disorder, and it may explain why you’re not feeling well when nothing obvious seems to be wrong. It is estimated that this syndrome afflicts over 60 million Americans and one in four adults over age 35 and it sets the stage for catastrophic health problems, such as heart disease, diabetes, Alzheimer’s, cancer, and other age-related diseases. That’s why you need to be aware of some key metabolic syndrome risk factors.
Metabolic Syndrome is a disorder that develops slowly over time, often over a course of 20 years or more. It refers to a cluster of conditions that occur simultaneously and increase your risk of dangerous diseases and disorders such as cardiovascular disease and diabetes. These conditions usually include:
Having one of these conditions doesn’t mean that you have metabolic syndrome. In fact, this is a complicated disorder and the criteria for metabolic syndrome is constantly changing. But the more of these conditions that you suffer from, the greater your risk of the more serious conditions increases that are associated with metabolic syndrome.
Every person is different and will experience a range of metabolic syndrome symptoms. The reason why a metabolic syndrome diagnosis can be so hard to make is because of the fact that you won’t realize you have many of these issues until you visit your doctor. This means you could go for years not knowing the damage that these conditions are doing to your body. Which is another reason why you should have regular check-ups to keep watch over your health.
The most common metabolic syndrome symptoms are:
If you have 3 or more of the above, you should consider yourself either having or at high risk of Metabolic Syndrome
Making a metabolic syndrome diagnosis isn’t easy because it involves many different criteria and must be assessed on an individual basis. However, generally speaking there are 5 criteria for metabolic syndrome. Any three of these factors must be present in one person to make a diagnosis. These factors are:
No one knows for sure what causes Metabolic Syndrome. However, there are several metabolic risk factors that you should be aware of. These include:
If you have a strong family history of type 2 diabetes, early heart disease and hypertension, then it increases your risk of developing metabolic syndrome.
If you have a mostly sedentary lifestyle and low activity levels, you’re more likely to develop this metabolic syndrome symptoms and problems.
Excess weight is probably the biggest metabolic syndrome risk factor. Metabolic syndrome affects about 9 percent of people who are in a healthy weight range. It affects 22 percent of people who are overweight and 60 percent of obese people.
Eating a diet rich in carbohydrates, particularly simple or refined carbohydrates, will raise your blood sugar and increase your risk of insulin resistance.
Smoking increases your risk of everything, including metabolic syndrome.
Another common metabolic syndrome risk factor is menopause. Once women are past this milestone, their risk of metabolic syndrome increases.
The fundamental defect in patients with Metabolic Syndrome is insulin resistance in both adipose or fat tissue and muscle tissue. The net result is hyperinsulinemia, which is higher than normal levels of insulin in the blood.
Each cell reacts to insulin differently. Some organs are highly sensitive to high insulin levels, while others are less so. Insulin resistance itself doesn’t cause damage, it’s the reaction of the various tissues to chronic high insulin that is the main problem. This problem manifests throughout the body. Some of the main problems that can occur as a result of this are:
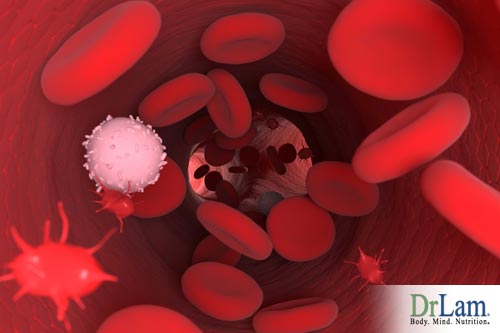
Excess insulin attacks the inner lining or endothelium of the arterial walls and increases the risk of arterial blood clots, which can cause heart attacks or strokes. The pathophysiology of this is very complicated and not fully understood. However, high insulin levels appear to reduce nitrous oxide activities , which could lead to hypertension. They also increase platelet and monocyte adhesion, causing increased coagulation and caused impaired fibrinolytic activity and impaired degradation of glycosylated fibrin. The end result can be increased blood pressure, increased formation of atherosclerotic plaques, increased thrombus formation, angina, and heart attack. Damage to the endothelium also markedly increases the risk of cardiovascular disease.
Type 2 diabetes develops when the pancreas “burns itself out”. This occurs when the demand for insulin is high for a prolonged period and the pancreas can’t keep up because it’s in an insulin resistance state.
When the ovaries are consistently exposed to high insulin levels they increase their testosterone secretion accordingly. This is often a major factor in the development of polycystic ovary syndrome.
Some research indicates that metabolic syndrome symptoms and problems might also increase the risk of prostate, colon and breast cancer.
Metabolic Syndrome also generates high levels of cell-damaging free radicals and causes premature aging. Some researchers believe it can also increase the risk of Alzheimer’s disease.
Excessive insulin leads to sodium retention and the build up of fluid. This can result in hypertension, a condition that is present in 50% of those with Metabolic Syndrome.
A metabolic syndrome diagnosis usually occurs as the end results of years (often decades) of taking in a modern day diet high in refined carbohydrates such as breads, starches and sweets. These foods trigger a rapid increase in blood sugar levels, and the body responds by raising insulin levels. This in turn helps to move the sugar out of the bloodstream into the cells. Insulin is a hormone secreted by the pancreas. It helps the body utilize glucose (blood sugar) by binding with receptors on cells like a key fits into a lock. Once the key – insulin – has unlocked the door of the cell, the glucose passes from the blood into the cell. Inside the cell, glucose is either used for energy or stored for future use in the form of glycogen in liver or muscle cells.
The more carbohydrates you eat, the more insulin your pancreas releases to lower your blood sugar. This is especially relevant when it comes to simple or refined carbohydrates like white bread or flour that are converted into sugar quickly once inside your body. While insulin levels naturally rise and fall with each meal as part of the normal metabolic process, chronic carbohydrate overload causes chronic insulin overload. This is because both muscle and fat cells recognize that excessive sugar is toxic.

When you eat too much sugar, your body tries to shut down the influx of sugar into the cells and goes into a down-regulation process to resist the command of insulin. This state is called insulin resistance. As insulin resistance is activated and blood glucose levels increase, the pancreas puts out even more insulin in order to avoid too high a blood sugar level. This compensatory increase in insulin output continues until the pancreas fails to keep up. For some people, this means that their body will produce two, three or even four times the normal amount of insulin. Yet, because the cells have lost their sensitivity to insulin, they require even more of it to maintain normal glucose levels. In advanced stages of insulin resistance, when the pancreas becomes exhausted and can no longer maintain the insulin production, insulin production drops, resulting in type 2 diabetes. Insulin resistance plus compensatory hyperinsulinemia or high blood insulin levels is nature’s way of preventing the evolution into type 2 diabetes. It is often referred to as a pre-diabetic state.
As long as there is insulin resistance, blood sugar and blood insulin levels will stay high. Over time, high blood sugar and high insulin will cause damage to almost every tissue they touch. It is important to recognize that while insulin resistance or high blood sugar are both bad for your health on their own, it takes both insulin resistance and compensatory hyperinsulinemia to cause the most harm. This will affect every system and organ in your body including the cardiovascular system, muscular system, kidney system, reproductive system, and lipid metabolic system.
There are over 60 million people in the United States alone who have Metabolic Syndrome. There are an additional 24 million people that have glucose intolerance, a pre-diabetic state. In addition, there are over 16 million people who have adult onset diabetes mellitus (Type 2 diabetes) and only half of these individuals knows they have diabetes. Some diabetics have had their disease for over 8 to 10 years before the physician even makes the diagnosis. This may account for the fact that over 60% of their diabetic patients already have major cardiovascular disease at the time of diagnosis of diabetes.
 Science has not yet determined why some people with insulin resistance eventually develop diabetes and others do not. Type 2 diabetes develops in a relatively small number of individuals who are insulin resistant. Most individuals who are insulin resistant continue to secrete large amounts of insulin and do not get type 2 diabetes. Insulin resistance is the body’s natural defense against chronic high sugar load and against the evolution to diabetes. In other words, type 2 diabetes is often the advanced stage of insulin resistance.
Science has not yet determined why some people with insulin resistance eventually develop diabetes and others do not. Type 2 diabetes develops in a relatively small number of individuals who are insulin resistant. Most individuals who are insulin resistant continue to secrete large amounts of insulin and do not get type 2 diabetes. Insulin resistance is the body’s natural defense against chronic high sugar load and against the evolution to diabetes. In other words, type 2 diabetes is often the advanced stage of insulin resistance.
The easiest way to measure your blood sugar levels is through a simple fasting blood sugar laboratory test. A fasting serum glucose level of more than 125 mg/dL is the current threshold for identifying patients with diabetes.
However, physicians are increasingly focused on the diabetes-related risk of coronary heart disease. In a cross-sectional study of 2,440 people, researcher Dr. Dennis Sprecher reported that people with a fasting serum glucose level of 100-125 mg/dL had an adjusted, 2.8-fold higher risk of having a coronary heart disease event than people with a fasting glucose level of less than 79 mg/dL. This finding suggests that patients with high levels of serum glucose in the nondiabetic range (100-125 mg/dl) also face a substantial risk of having coronary heart disease. In fact, the Cleveland Clinic Foundation now uses fasting serum glucose of 90 mg/dL or higher as a biomarker of coronary heart disease risk and this is a good marker of low cardiac risk.
Individuals with Metabolic Syndrome have an increased risk of heart disease according to the American Heart Association (AHA). Metabolic Syndrome doesn’t lead directly to Coronary Heart Disease (CHD) and neither do metabolic syndrome symptoms. Instead, people with metabolic syndrome symptoms have an increased prevalence of CHD. Having Metabolic Syndrome is akin to being injured by a shotgun blast, with multiple bullet wounds. While none of the multiple bullet wounds may by itself lead to death, the collative damage caused by the multiple bullet wounds raises the chances of death significantly. In real-life terms, this refers to the increasing risks of cardiovascular disease, cancer, stroke, and premature aging.
 Vladimir M. Dilman, M.D., co-author of The Neuroendocrine Theory of Aging, refers to insulin resistance as an “age-related pathology.” In fact, it is one of the few consistent indicators of longevity. Centenarians consistently have lower blood sugar levels and blood insulin levels relative to their age.
Vladimir M. Dilman, M.D., co-author of The Neuroendocrine Theory of Aging, refers to insulin resistance as an “age-related pathology.” In fact, it is one of the few consistent indicators of longevity. Centenarians consistently have lower blood sugar levels and blood insulin levels relative to their age.
In the mid-1970s, biologist Anthony Cerami discovered that chronically high blood glucose levels were the main trigger in a chemical process that produced advanced glycosylation end products (AGES), which were implicated in normal and advanced aging and age-enhanced diseases. AGEs form at accelerated rates whenever blood-sugar levels are high as they often are in advanced age.
The damage that AGEs can do to the body is extensive. Referred to as a carmelization or browning reaction, cross-linking by AGEs involve a chemical reaction between sugar and protein molecules. Every part of the body is affected by this, not a single organ or cells is left undamaged. This cross-linking of sugar and protein molecules leads to the stiffening of connective tissue and hardening of arteries, resulting in premature aging and hypertension. As cross-links increasingly reduce the flexibility and permeability of tissues and cells, cellular communications and repair processes also begin to break down. In response, a compensatory inflammatory response may be launched by the body, especially in the endothelium. This leads to a cascade of damaging events resulting in fatty streaks and atherosclerosis. Eventually, the tissues of the body become irreversibly transformed and the inevitable result is aging, disease and finally death.
It is well known that bathing your cells in high sugar (as in diabetics) causes premature aging. This is because this sugar-driven damage advances at breakneck speed, raising your levels of AGE-infused collagen so they’re comparable to those of much older people. Diabetics also suffer a very high incidence of nerve, artery and kidney damage because high blood sugar levels in their bodies markedly accelerate the chemical reactions that form AGEs. The endothelium of diabetic patients also secretes unwanted growth factors that leads to blood vessel hypertrophy and reduced lumen size. This reduces the blood flow, exacerbating the already compromised insulin delivery and further increases the chances of insulin resistance. The reduced blood flow leads to reduced oxygen delivery to needy tissues, resulting in the increased peripheral neuropathy or nerve conditions commonly seen in diabetes.
Physicians have been concentrating on treating the Metabolic Syndrome symptoms such as hypertension and dyslipidemia rather than concentrating on the underlying problem, which is insulin resistance. Since over 50% of the prescriptions filled in the United States are for hypertension, elevated cholesterol levels, heart disease, and diabetes, you can get a glimpse of the economic importance of this problem.
Metabolic Syndrome is usually totally reversible without drugs. The key is to slow down carbohydrate absorption while increasing insulin sensitivity. This can be done by lowering your carbohydrate intake (the low-carb diet), together with a nutritional supplementation program designed to slow carbohydrate absorption, increase insulin sensitivity, and normalize blood sugar levels.
 However, human nature (and human metabolism) being what it is, the majority of patients with Metabolic Syndrome cannot accomplish these goals. In these cases, each metabolic disorder associated with Metabolic Syndrome needs to be treated individually, and aggressively. A short-term treatment with drugs may sometimes be needed.
However, human nature (and human metabolism) being what it is, the majority of patients with Metabolic Syndrome cannot accomplish these goals. In these cases, each metabolic disorder associated with Metabolic Syndrome needs to be treated individually, and aggressively. A short-term treatment with drugs may sometimes be needed.
The lipid abnormalities seen with Metabolic Syndrome (low HDL, high LDL, and high triglycerides) respond nicely to weight loss and exercise. Treatment should be aimed primarily at reducing LDL and triglyceride levels, and raising HDL levels. Successful drug treatment usually requires treatment with a statin or a fibrate drugs, or a combination of a statin with either niacin or a fibrate. It should also be noted that the use of statin drugs is not without problems.
Patients with Metabolic Syndrome often have disorders of coagulation that make it easier to form blood clots within blood vessels. These blood clots are often a precipitating factor in heart attacks. That’s why patients with metabolic Metabolic Syndrome should generally be placed on daily aspirin therapy to help prevent such clotting events.
High blood pressure is present in more than half of people Metabolic Syndrome. When combined with insulin resistance, this is one of the most serious metabolic syndrome risk factors. Recent studies have suggested that successfully treating hypertension in patients with diabetes can reduce the risk of death and heart disease substantially. Low dose diuretics should be used according to Dr. Reaven. No more than 12.5 mg of hydrochlorothiazide should be prescribed.
People with Metabolic Syndrome should not be prescribed the anti-hypertensive doses of thiazides that have been recommended in the past. Instead, difficult cases should be controlled with ACE inhibitors. ACE inhibitors increase levels of nitrous oxide (a potent endothelium generated vasodilator), resulting in vasodilation and blood pressure reduction. ACE inhibitors also have been shown to improve endothelial function, and so have HMG-CoA reductase inhibitors (such as lovastatin and pravastatin). To a lesser degree, calcium channel blockers (such as verapamil and nifedipine) can have the same action.
High blood sugar must be normalized. Traditionally there are four points of intervention to reduce blood sugar:
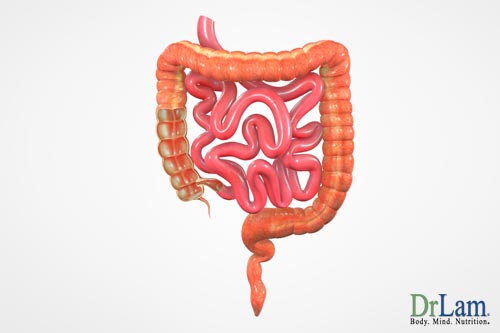 Intestines. Alpha-glucosidase inhibitors such as acabose can be effective here. The primary mechanism of action of these agents is to inhibit specific enzymes that break down carbohydrates in the small intestine. This delays the absorption of carbohydrates, resulting in a reduction of postprandial hyperglycemia or high blood sugar levels after eating. No specific action on insulin resistance has been reported.
Intestines. Alpha-glucosidase inhibitors such as acabose can be effective here. The primary mechanism of action of these agents is to inhibit specific enzymes that break down carbohydrates in the small intestine. This delays the absorption of carbohydrates, resulting in a reduction of postprandial hyperglycemia or high blood sugar levels after eating. No specific action on insulin resistance has been reported.
There are no drug treatments that can directly reverse the insulin resistance that’s associated with metabolic syndrome symptoms and problems. However, there are natural ways to reverse this resistance including:
Clearly, the following goals should be met in any diet for Metabolic Syndrome sufferers:
The question is: If you reduce carbohydrates and fats, then how are you going to get enough calories? The lack must be made up with another food group. Basically, carbohydrates can be replaced with proteins or with fats. There are benefits and drawbacks to both of these options. Firstly, saturated fats must be restricted to reduce the risk of cardiovascular disease and to lower LDL cholesterol level. Therefore, you need to replace your carbohydrates with “good” fat only. These often come from plant and vegetable sources such as olive oil and nuts, not from the artery-clogging saturated fats present in steaks. This may benefit LDL cholesterol levels without raising insulin levels.
Replacing carbohydrates with proteins can be problematic as it ignores the fact that protein, once in the intestinal tract, converts to amino acid. And amino acids increase insulin secretion. However, it is still unclear about whether proteins are as potent as carbohydrates in stimulating insulin secretion.
Dr Reaven’s Metabolic Syndrome diet derives 45 percent of calories from carbohydrates, 15 percent from proteins and a hefty 40 percent from fats. Dr Reaven’s diet is very different from the latest run of carbohydrate diets because it’s low in protein. This is very different from Dr Atkins’ diet, which dictates a high protein diet. A diet high in protein is suitable for those with normal insulin sensitivity, but inappropriate for those with Metabolic Syndrome.
Metabolic syndrome treatment is possible with the use of natural, non-toxic food based compounds. This can help to reduce metabolic syndrome symptoms, normalize blood sugar, and increase insulin sensitivity.
Normalizing the lipid abnormalities.
For abnormal lipid levels, try:
Normalizing Clotting
To reduce your risk of developing a blood clot risk, the following natural compounds may be helpful:
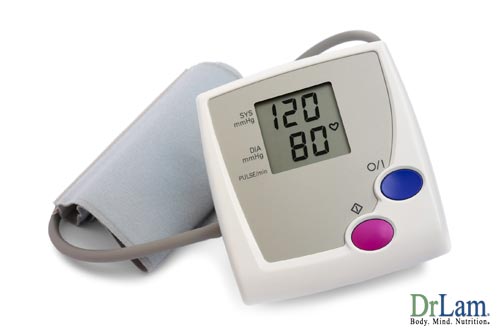
Normalizing Hypertension
For glucose normalization and to increase insulin sensitivity, natural non-toxic compounds that have sugar modulation effects include:
Rebalancing Digestion
You can enhance digestive balance and efficiency with digestive enzymes and green foods such as chlorella, spirulina, algae, soluble fiber, and probiotics.
Antioxidant Deficiency
A strong multivitamin with at least 10,000 I.U. of beta carotene, 500 mg of vitamin C, 200mg of selenium, 100 mg of grape seed extract, 30 mg of coenzyme Q10 should be taken to correct antioxidant deficiencies.
Adrenal Function Support
To support your adrenal glands, try taking Pantethine 300 – 900 mg, licorice root, or Panthothenic acid 400 – 1,200 mg.
General Health Support
Other synergistic nutrients include:
It is obvious that there is no single magic bullet that can overcome this condition. Metabolic syndrome symptoms and problems are highly individual and will manifest differently depending on your body and your overall condition. You must also be careful when taking any supplements in case it has an adverse effect on your body, particularly when you’re already unwell. So, make sure you get professional help before making any changes to your dietary routine.
Studies have shown that modest exercise may be beneficial. However, these benefits will probably not be achieved after a casual walk a couple of nights a week. Significant, regular exercise is required if you want to see improvements in insulin action, triglycerides, and HDL cholesterol. Exercise is as powerful a tool for weight loss, which will improve the benefits of this strategy.
Every attempt should be made to reduce total body weight to within 20% of the “ideal” body weight calculated for age and height. This will improve Metabolic Syndrome symptoms and problems significantly.
a. Alcohol. The evidence is divided about the effects of alcohol on Metabolic Syndrome. The best advice is to ensure that any drinking you do is at moderate levels. And if you’re a non-drinker, don’t take it up in the hopes that it will improve your insulin levels, as it may have the opposite effect in some people.
b. Smoking. Smoking is unequivocally bad for your body and is also associated with high triglycerides, low HDL or good cholesterol and insulin resistance.
 Two of the key factors that affect health are glucose (also known as blood sugar) and the hormone insulin. Because of the high carbohydrate foods that many people eat, insulin and glucose levels can go out of control. Quite simply, many people are overdosing on glucose and insulin — two substances that will accelerate aging and encourage the onset of diseases in high doses. Insulin resistance is the body’s way of resisting these excessive sugar and carbohydrate levels, which is why 60 million Americans now experience this problem. When insulin resistance is accompanied by high blood insulin levels as the pancreas tries to encourage the cells to increase their glucose intake, the systemic damage is collectively known as Metabolic syndrome
Two of the key factors that affect health are glucose (also known as blood sugar) and the hormone insulin. Because of the high carbohydrate foods that many people eat, insulin and glucose levels can go out of control. Quite simply, many people are overdosing on glucose and insulin — two substances that will accelerate aging and encourage the onset of diseases in high doses. Insulin resistance is the body’s way of resisting these excessive sugar and carbohydrate levels, which is why 60 million Americans now experience this problem. When insulin resistance is accompanied by high blood insulin levels as the pancreas tries to encourage the cells to increase their glucose intake, the systemic damage is collectively known as Metabolic syndrome
Fortunately, Metabolic Syndrome can be reversed with dietary, lifestyle, and nutritional supplements. Here are some effective strategies for recovery:
If you need to know about about metabolic syndrome or believe that you may have it, then contact Dr. Lam’s team today on +1-626-571-123. Our friendly team will help you understand your symptoms and options. You can also ask us a question through the Ask The Doctor system by clicking here.
