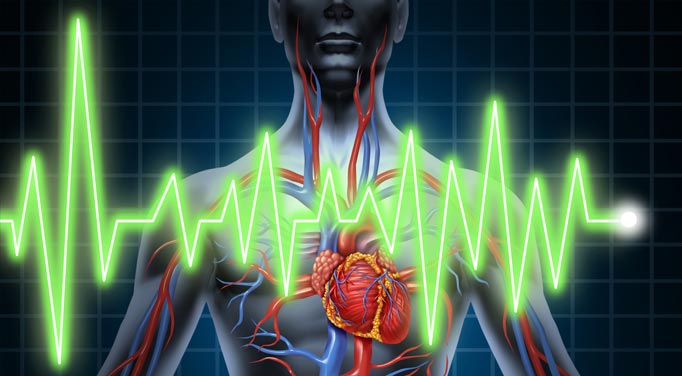
 Everyone is at risk for cardiovascular disease, the leading cause of death worldwide. The established risk factors for heart disease, such as serum cholesterol level, smoking, and family history, account for only one-half to three-fourths of the cases. The remainder is a result of other factors that promote atherosclerosis (the buildup of fatty deposits in blood vessels) such as infections. A homocysteine blood test may offer insight into atherosclerosis. C. pneumoniae, a bacterium that causes respiratory infection, has been found in 70-80% of plaques taken from a heart disease patient. The jury is still out as far as the exact mechanism of injury is concerned. However, it has been postulated that the infection triggers the immune system's response and inflammation within the blood vessel wall. Large-scale research to determine mechanism is currently underway. Efforts to determine more ways of preventing heart disease and the use of homocysteine blood test have led to the unearthing of about 300 predictors. One of these new markers for heart disease is male baldness. Hair loss to the crown area has been linked to a three-fold greater risk of heart disease in men, according to a study at Harvard Medical School by Joanne Manson, chief of the Division of Preventive Medicine at Brigham and Women's Hospital in Boston, and her colleagues. The connection may be elevated male hormone levels. These findings will pave the way in the coming years to new therapies.
Everyone is at risk for cardiovascular disease, the leading cause of death worldwide. The established risk factors for heart disease, such as serum cholesterol level, smoking, and family history, account for only one-half to three-fourths of the cases. The remainder is a result of other factors that promote atherosclerosis (the buildup of fatty deposits in blood vessels) such as infections. A homocysteine blood test may offer insight into atherosclerosis. C. pneumoniae, a bacterium that causes respiratory infection, has been found in 70-80% of plaques taken from a heart disease patient. The jury is still out as far as the exact mechanism of injury is concerned. However, it has been postulated that the infection triggers the immune system's response and inflammation within the blood vessel wall. Large-scale research to determine mechanism is currently underway. Efforts to determine more ways of preventing heart disease and the use of homocysteine blood test have led to the unearthing of about 300 predictors. One of these new markers for heart disease is male baldness. Hair loss to the crown area has been linked to a three-fold greater risk of heart disease in men, according to a study at Harvard Medical School by Joanne Manson, chief of the Division of Preventive Medicine at Brigham and Women's Hospital in Boston, and her colleagues. The connection may be elevated male hormone levels. These findings will pave the way in the coming years to new therapies.
Four new markers will be studied - lipoprotein(a), mitochondrial function, homocysteine, and oxidative stress and their ramifications for the promotion of optimum cardiovascular health.
Fifty percent of Americans have elevated serum cholesterol levels. And the increase occurs naturally as we age. In men, most of the increase occurs after about age 45. In women, most of the increase occurs after age 55, and especially after menopause. The goal for cholesterol management is to lower the blood level of bad (low-density lipoprotein, or LDL)- cholesterol and increase the level of good (high-density lipoprotein, or HDL-) cholesterol as its job is to mop up LDL-cholesterol. There is no question that lowering dietary intake of cholesterol and saturated fats prevent heart disease because it lowers blood LDL-cholesterol levels.
Cholesterol levels alone cannot explain many heart attack deaths. Autopsy studies of heart attack victims, however, show that a good percentage of heart attack victims have clean vessels and ideal lipoprotein levels. It is obvious that there are other causes for heart disease than the traditional. Indeed, researchers with the Framingham Heart Study (the decades-long study that brought us the term "risk factor") identified a relative of LDL-cholesterol called lipoprotein(a) [Lp(a)], which is now recognized as MAJOR independent risk factor for heart disease. Lp(a) fosters the deposition of cholesterol on artery walls as well as interferes with the body's means of dissolving clots. Lp(a) fosters cholesterol deposition by enhancing oxidation of LDL-cholesterol. It is the oxidized form of cholesterol that penetrates the endothelium, leading to the build-up of plaque and vascular disease.
 Some researchers believe that cardiovascular disease is primarily caused by chronic deficiencies of vitamins and other essential nutrients with defined biochemical properties, such as coenzymes, cellular energy carriers, and antioxidants. Chronic depletion of these essential nutrients in endothelial and vascular smooth muscle cells impairs their ability to function properly.
Some researchers believe that cardiovascular disease is primarily caused by chronic deficiencies of vitamins and other essential nutrients with defined biochemical properties, such as coenzymes, cellular energy carriers, and antioxidants. Chronic depletion of these essential nutrients in endothelial and vascular smooth muscle cells impairs their ability to function properly.
Certain supplements, along with a homocysteine blood test, can help with cardiovascular health. Take the effects of Vitamin C (ascorbic acid) deficiency as an example. Humans are one of a few animals that cannot produce ascorbate. Humans must get Vitamin C from external sources. Deficiency of Vitamin C leads to a disease called scurvy, the symptoms of which are caused the reduced ability of the body to make collagen, an essential component of wound healing, bones and joints, and blood vessels. Chronic ascorbate deficiency leads to impairment in the structure of the blood vessel walls and tiny lesions in its inner wall. These changes are the hallmarks of early atherosclerosis. Atherosclerotic plaques can develop as the result of an overcompensating repair mechanism consisting of deposition of systemic plasma and local cellular response which includes extra cellular accumulation of Lp(a) and fibrinogen/fibrin at the site of injury. This repair mechanism is exacerbated primarily at sites of hemodynamic stress. This explains why the most frequent clinical manifestation of cardiovascular disease such as myocardial infarction, is the local development of atherosclerotic plaques in coronary arteries. As a result of confirmation in animal studies, ascorbate with other essential nutrients and a homocysteine blood test are now being recommended for the prevention and treatment of cardiovascular diseases.
Mathias Rath and colleague conducted a yearlong study to determine the effect of a defined nutritional supplementation program on the natural progression of coronary artery disease. He gave 55 patients with various stages of coronary artery disease, aged 44-67, a daily nutritional supplementation program including 2,700 mg of Vitamin C, vitamin B complex, 600 IU of Vitamin E (d-alpha-tocopherol), 450 mg of L-proline, 450 mg of L-lysine, 390 mcg of folic acid, 30 mg of coenzyme Q-10, and 450 mg of citrus bioflavinoids. Changes in the progression of coronary artery calcification before and during the program were determined by Ultrafast Computerized Tomography. Before the intervention, the natural progression rate of the coronary artery calcification averaged 44% per year. However, during the year of treatment, the progression of coronary artery calcification decreased by an average of 15%. In a subgroup of patients with early stages of coronary artery disease, treatment resulted in a statistically significant decrease, with no further progression of coronary calcification. In individual cases, reversal and complete disappearance of previously existing coronary calcification were documented. This landmark study, published in the Journal of Applied Nutrition (1996, 48:3), showed that coronary artery disease could be effectively prevented and treated by natural means. In patients with early coronary calcification, progression was halted. In individual cases with small-calcified deposits, nutritional supplement intervention led to the complete disappearance of the deposits.
It is postulated that the nutrients used by Rath initiate the reconstitution of the vascular wall. Ascorbate is essential for the synthesis and hydroxylation of collagen. L-lysine and L-proline are important substrates for the biosynthesis of matrix protein and competitively inhibit the binding of lipoprotein(a) to the vascular matrix. Maintaining the integrity and physiological function of the vascular wall is the key therapeutic target in controlling cardiovascular disease.
 It is worth noting that Vitamin C, being water-soluble, is cleared through the body very quickly, giving it a very short half-life. To maintain continuous optimum levels of Vitamin C in the body, ascorbate should be taken in divided dosages throughout the day. To overcome this problem, a fat-soluble form of Vitamin C, ascorbyl palmitate, has been developed. It is readily absorbed from the gastrointestinal track and finds its way to the micro-capillaries where it stays to exerts its health enhancing properties mentioned above. The combination of vitamin C and a homocysteine blood test can be effective in improving heart health.
It is worth noting that Vitamin C, being water-soluble, is cleared through the body very quickly, giving it a very short half-life. To maintain continuous optimum levels of Vitamin C in the body, ascorbate should be taken in divided dosages throughout the day. To overcome this problem, a fat-soluble form of Vitamin C, ascorbyl palmitate, has been developed. It is readily absorbed from the gastrointestinal track and finds its way to the micro-capillaries where it stays to exerts its health enhancing properties mentioned above. The combination of vitamin C and a homocysteine blood test can be effective in improving heart health.
The amount of each nutrient required to prevent the onset of disease states is outlined in the Recommended Dietary Allowances (RDAs). As of July 2000, the RDA for Vitamin C is 60 mg per day. This is about the amount present in one RED and will prevent scurvy. The amount for optimum health, however, is less well defined. However, use of vitamin C and a homocysteine blood test are effective in over all hearth health.
Humans, other primates, and guinea pigs do not produce ascorbate endogenously. Guinea-pigs fed a diet low in ascorbate, an amount equivalent to the usual human intake, rapidly developed atherosclerotic plaques, similar to those found in humans. When large amounts of supplementary ascorbate were given to these guinea pigs, there was a regression in plaque formation. Linus Pauling, two-time Nobel Laureate, postulated that Lp(a) may be the surrogate for ascorbate in the human. Low dietary intake of ascorbate leads to weakened blood vessels because ascorbate is required for the synthesis of collagen and elastin, which strengthen the blood vessel wall. In the absence of sufficient ascorbate, Lp(a) is mobilized to repair these structural defects in arterial walls by being deposited to strengthen the tissue. However, if the plasma concentration of Lp(a) is too high, the process goes too far. Too much Lp(a) gets deposited in the arterial wall, and plaque formation is initiated. Dr. Pauling concluded that the optimum intake of Vitamin C is perhaps 100 times more than the RDA. During the last 25 years of his life (he died at age 93 from cancer), Dr Pauling increased his own intake of Vitamin C from 50 times to 300 times the RDA, taking 3,000 mg to 18,000 mg per day. This amount is consistent with the amount of ascorbate in animals that are capable of producing their own on a daily basis. It is fair to say that Dr. Pauling believed that cardiovascular disease is the general result of ascorbate deficiency.
 Mitochondria are the energy factories of the cell. The energy currency they produce is ATP. Generation of ATP is therefore vital to cellular process. Coenzyme Q10, or ubiquinone, is a vital component in the ATP-generating process. It acts as an electron acceptor/proton donor; hence its presence in the body is fundamental to the support of cellular life. It is omnipresent in body tissues.
Mitochondria are the energy factories of the cell. The energy currency they produce is ATP. Generation of ATP is therefore vital to cellular process. Coenzyme Q10, or ubiquinone, is a vital component in the ATP-generating process. It acts as an electron acceptor/proton donor; hence its presence in the body is fundamental to the support of cellular life. It is omnipresent in body tissues.
The body's production of CoQ10 begins to decline after age 20 to just 50% of levels by age 70. Because the function of the heart is so dependent on the energy produced with the help of CoQ10, CoQ10 is extremely important for heart health. It is also important as a powerful antioxidant and a membrane stabilizer. The range of heart conditions for which research has found CoQ10 beneficial include (1) congestive heart failure, (2) cardiomyopathies, (3) arrhythmias, (4) angina, when there is a lack of oxygen, and (5) muscular dystrophy.
Individuals with cardiac disorders have been identified as having abnormally low levels of CoQ10. Numerous long-term studies have been conducted to ascertain the efficacy of CoQ10. These studies indicate that there is a statistically significant improvement in the condition of those patients with myocardial dysfunctions such as ischemic cardio-myopathy or congestive heart failure when they take CoQ10. In an 8-year study of 424 patients with cardiac dysfunction, 58% improved by one functional class, 28% by two classes, and 1.2% by three classes. Further, overall medication requirements dropped, with 43% of the patients discontinuing between one and three drugs. Only 6% were required to add one drug. In another study on 40 patients undergoing elective coronary artery bypass surgery, pretreatment with CoQ10 at 150mg/day for seven days served as a protection against oxidative compounds.
CoQ10 also plays a vital role as an antioxidant in cellular membranes and plasma lipoproteins. It is present in all plasma membranes and in LDL-cholesterols. Studies illustrate CoQ10's protective action against the oxidative modification that makes LDL-cholesterol atherogenic. In its reduced form, ubiquinol, CoQ10 also functions as a chain-breaking antioxidant and is believed to regenerate Vitamin E.
You can get CoQ10 from your diet, although the amount of food intake is insubstantial. For example, one pound of sardines or 2.5 pounds of peanuts provide 30 mg of CoQ10.
Working synergistically with CoQ10 are two endogenous antioxidants that enhance mitochondrial function and reduce free radical damage - L-Carnitine and Lipoic Acid.
 The ability of the cell to utilize fatty acids as a source of fuel is essential for optimizing the production of ATP by mitochondria in cardiac cells to keep the heart properly functioning. L-carnitine assists in this transportation process by bringing fatty acids from the extracellular space into the mitochondria. In one double-blind trial, 500 mg per day of a modified form of carnitine called propionyl-L-carnitine lead to a 26% increase in exercise capacity after six months.
The ability of the cell to utilize fatty acids as a source of fuel is essential for optimizing the production of ATP by mitochondria in cardiac cells to keep the heart properly functioning. L-carnitine assists in this transportation process by bringing fatty acids from the extracellular space into the mitochondria. In one double-blind trial, 500 mg per day of a modified form of carnitine called propionyl-L-carnitine lead to a 26% increase in exercise capacity after six months.
Lipoic Acid is both a water- and fat-soluble antioxidant. It neutralizes free radicals in both the fatty and watery regions of cells, in contrast to Vitamin C, which is water soluble, and Vitamin E, which is fat soluble. Lipoic acid is therefore called the "universal antioxidant". It has the ability to recycle both Vitamin C and E in our body. It helps break down sugars so that energy can be produced from them through cellular respiration. In addition to serving as the bulb of the body's antioxidant network, lipoic acid is the only antioxidant that can boost the level of intracellular glutathione, a cellular antioxidant of tremendous importance. Glutathione is a water-soluble antioxidant and is essential for the optimum functioning of the immune system.
Homocysteine is an amino acid by-product of food metabolism. It contributes to atherosclerosis, reduces the flexibility of blood vessels, and increases clotting by making platelets stickier and slows blood flow. Studies show a direct correlation between high serum homocysteine levels increases the risk of heart attack and stroke. A homocysteine blood test measures the levels of homocysteine in the blood and can thereby identify potential heart attack and stroke risk.
Research has shown that folate and other B vitamins break down homocysteine. The American Heart Association currently advocates that people who are at high risk of heart disease include more folate and other B vitamins in their diet - at least 400 microgram's worth. Studies have been conducted that show very modest supplementation of Vitamin B-6 (10mg), folic acid (650 mcg), and Vitamin B-12 (400 mcg) reduce plasma serum homocysteine levels by 49.8% in men with hyper-homocysteinemia. A homocysteine blood test may be ordered for individuals with a vitamin B12 or folate deficiency.
There are other factors that may prompt the use of a homocysteine blood test. Individuals who are or have been clinically malnourished, for reasons including poverty, eating disorders, and addiction and alcoholism may benefit from a homocysteine blood test. Doctors may order a homocysteine blood test for patients with other risk factors, such as: a family history of coronary artery disease, tobacco use, high blood pressure, high cholesterol, and obesity.
 Oxidative stress by free radicals in our body contributes to cardiovascular disease. During oxidative stress, free radicals produce structural changes in serum LDL-cholesterol. These damaged LDL-cholesterol molecules are recognized as foreign to the body, and are therefore phagotized (engulfed) by macrophages (specialized white blood cells). These macrophages then fill up with lipids, forming "foam cells" that aggregate and adhere to the inner surface of blood vessels. They contribute to the development of lesions on the artery wall, initiating a cascade of events that ultimately lead to atherosclerosis.
Oxidative stress by free radicals in our body contributes to cardiovascular disease. During oxidative stress, free radicals produce structural changes in serum LDL-cholesterol. These damaged LDL-cholesterol molecules are recognized as foreign to the body, and are therefore phagotized (engulfed) by macrophages (specialized white blood cells). These macrophages then fill up with lipids, forming "foam cells" that aggregate and adhere to the inner surface of blood vessels. They contribute to the development of lesions on the artery wall, initiating a cascade of events that ultimately lead to atherosclerosis.
Over the years, research has consistently shown that Vitamin E offers significant protection against cardiovascular disease. Not only does Vitamin E reduce the risk of heart attack, it also inhibits platelet aggregation, increases the survival rate of patients undergoing bypass surgery and protects against other heart ailments, including angina. With vitamin E and the use of a homocysteine blood test, heart health can see some improvement. In the Cambridge Heart Antioxidant Study, 2002 patients with proven coronary heart disease were given 400 to 800 IU Vitamin E in a double-blind, randomized, placebo-controlled setting. Beneficial effects were apparent after one year of treatment. Other studies have shown that 100 IU per day of Vitamin E can significantly decrease coronary artery lesion progression. 800 IU per day reduced LDL susceptibility to oxidation by 50%. Furthermore, recent studies have determined that there is a synergistic effect between alpha- and gamma-tocopherol. This combination offers a greater level of protection against oxidative damage than either one alone.
Optimum cardiovascular health entails controlling the well-known risk factors including elevated cholesterol levels, hypertension, and stress. Elevated cholesterol levels can be controlled through drugs or natural supplements such as fiber, niacin, and more recently, red yeast rice powder (600 mg two times a day). Control of hypertension can be accomplished through drugs and/or natural supplementation such as Hawthorne (250 mg), magnesium (400 - 700 mg), calcium (800 - 1,000 mg), and potassium from food (400 - 600 mg). Adjunct nutritional supplementation to enhance stress reduction includes antioxidant nutrients such as coenzyme Q10 (CoQ10) and Vitamin E, Vitamin B complex, and Magnesium. These antioxidants counteract the increase in oxidative stress associated with psychological stress. A homocysteine blood test can also help with overall cardiovascular health.
 It is obvious that the traditional risk factors such as cholesterol, hypertension, and stress, while good markers of cardiovascular disease, do not tell the whole story. The fact that many people develop cardiovascular disease in spite of normal cholesterol levels, normal blood pressure values, and relatively low stress environment imply that there are other risk factors yet to be discovered.
It is obvious that the traditional risk factors such as cholesterol, hypertension, and stress, while good markers of cardiovascular disease, do not tell the whole story. The fact that many people develop cardiovascular disease in spite of normal cholesterol levels, normal blood pressure values, and relatively low stress environment imply that there are other risk factors yet to be discovered.
Four such markers are explored. Standardized laboratory references have yet to be established for these new markers and may never be established due to their multifactorial complexity of cardiovascular disease. A natural nutritional supplementation approach appears to the best available option for those who don't want to wait.
References
Chello M, Mastroroberto P, Romano R, et al: Protection by coenzyme Q10 from myocardial reperfusion injury during coronary artery by-pass grafting. Ann Thorac Surg 1994;58(5): 1427-1432.
Cooney RV, Franke AA, Harwood PJ, et al: Gamma-tocopherol detoxification of nitrogen dioxide: superiority to alpha-tocopherol. Proc Natl Acad Sci 1993;90:1771-1775.
Heber D, Yip I, Ashley JM, Elashoff DA, Elashoff RM, Go VL. Cholesterol-lowering effects of a proprietary Chinese red-yeast-rice dietary supplement. Am J Clin Nutr 1999 Feb 69;2:231-6.
Heber D. Natural Remedies for a Healthy Heart. Garden City Park, NY: Avery; 1998.
Langsjoen H, Langsjoen P, Lansjoen P, et al. Usefulness of coenzyme Q10 in clinical cardiology - a long-term study. Mol Aspects Med 15(suppl) 1994;S165-S175.
Leuchtgens H. Crataegus special extract WS 1442 in NYHA. Heart Failure: a placebo-controlled randomized double-blind study Fortschr Med 1993;111( 20-21):352-354.
Mancini M, Rengo F , Lingetti M, Somentino GP, Nolfe G. Controlled study on the therapeutic effect of propionyl L-carnitine in patients with congestive heart failure. Arzneimitteforschung 1992; 42:1101-4.
Papas AM. Other antioxidants In: Antioxidant Status, Diet, Nutrition and Health. New York: CRC Pr, 1999.
Pauling L. Case Report : Lysine/Ascorbate-Related Amelioration of Angina Pectoris. J of Ortho Med 1991;6:3-4.
Pauling L. Proceedings of the National Academy of Sciences, USA (4-6).
Rath M, Niedzwiecki A. Nutritional Supplement Program Halts Progression of Early Coronary Atherosclerosis. Documented by Ultrafast Computed Tomography. Journal of Applied Nutrition 1996; 3:68-77.
Rath M, Pauling L. Solution to the puzzle of human cardiovascular disease. Its primary cause is ascorbate deficiency, leading to depositon of lipoprotein(a) and fibrinogen/fibrin in the vascular wall. J Ortho Med 1991; 6:125-134.
Reaven PD, Knouw A, Beltz WF, et al. Effect of dietary antioxidant combinations in human: protection of LDL by Vitamin E but not by beta-carotene. Arter Throm 1993;3:590-600.
Schussler M. Holzl J, Fricke U: Myocardial effects of flavonoids from Crataegus species. Arzneim Forsch 1995;45(8): 842-845.
Sinatra ST, De Marco J. Free radicals, oxidative stress, oxidized low-density lipoprotein (LDL), and the heart: antioxidants and other strategies to limit cardiovascular damage. Conn Med 1995; 59(10):579-588.
Stephens NG, Parson A, Schofield PM, et al: Randomized controlled trial of Vitamin E in-patients with coronary disease: Cambridge Heart Antioxidant Study. The Lancet 1996;347(9004):781-786.
Stoney CM. Plasma homocysteine levels increase in women during psychological stress. Life Sci 1999; 64(25):2359-2365.
© Copyright 1999 Michael Lam, M.D. All Rights Reserved.