 Unless you’ve experienced a major hormonal change, such as pregnancy or menopause, you may not be aware of just how much hormones affect your health and wellbeing. They can have a major influence on just about every part of your body and how you feel as a whole. And even if you aren’t currently experiencing obvious symptoms, you could still benefit from taking a holistic hormone balance approach to maintain your health.
Unless you’ve experienced a major hormonal change, such as pregnancy or menopause, you may not be aware of just how much hormones affect your health and wellbeing. They can have a major influence on just about every part of your body and how you feel as a whole. And even if you aren’t currently experiencing obvious symptoms, you could still benefit from taking a holistic hormone balance approach to maintain your health.
Hormones play a role in essential functions, including your metabolism, sleep/wake cycle, body temperature, hunger/satiety signals, stress response, and reproduction. The four main areas to consider when talking about holistic hormone balance are:
Each of these affects the other. And the last three of them make up the Hormone Circuit, which is part of your NeuroEndoMetabolic (NEM) Stress Response.
Your NEM is your body’s global response to stress. It’s a network of organs and systems that work together towards that goal. There are six NEM circuits: the Hormone, the Bioenergetics, the Cardionomic, the Neuroaffect, the Inflammation, and the Detoxification circuits. All of them are involved when your body is facing stress, but the usual first responders are your adrenal glands, which are part of your Hormone Circuit.
The Hormone Circuit is composed of your adrenals, thyroid, and gonads (sex organs). Insulin, another major hormone in your body's hormone balance, is related more to the Bioenergetic Circuit, which is composed of your pancreas, thyroid, and liver. The thyroid links these two circuits.
Hormone balance is a delicate affair. First, all hormones fluctuate according to a rhythm or in response to some physiological change. For example, insulin secretion increases when you eat carbohydrates. Cortisol, your body’s main stress hormone, should be at its peak in the morning to help you get up and be alert, then dip to its lowest levels at night to allow you to sleep.
Already, you can deduce some possible disruptors of these hormones, such as overconsumption of sugar or bad sleep. But there are many other possible hormone balance disruptors, and most people have a combination of several going on at the same time. They include:
Unfortunately, just one of these issues can cause a domino effect that can affect multiple organs and systems, including your Hormone and Bioenergetics circuits.
When you talk to your doctor about potential hormone imbalances, it can be a good idea to bring this list. We consider these points as part of our diagnostic approach for hormone imbalance, along with certain tests and taking a thorough medical, nutritional, and psychological history. Determining what kind of hormone imbalance you have as well as what factors are aggravating it can be very important for choosing the right care plan.
 Before we get into each of the four main areas you need for holistic hormone balance, it helps to have an understanding of how some of these hormones are made. Specifically, mineralocorticoids, glucocorticoids, androgens, and estrogens.
Before we get into each of the four main areas you need for holistic hormone balance, it helps to have an understanding of how some of these hormones are made. Specifically, mineralocorticoids, glucocorticoids, androgens, and estrogens.
First, the primary substance that your body uses to make these hormones is cholesterol. Cholesterol is a type of lipid that’s found in all your body’s cells. It’s then biosynthesized into pregnenolone, the precursor to most of your steroid hormones.
From pregnenolone, your body makes progesterone. Then from progesterone, you get mineralocorticoids, such as corticosterone and aldosterone, as well as glucocorticoids, such as cortisol. Progesterone is also used to make DHEA, the precursor to androstenedione, which then ultimately makes testosterone. The androstenedione is synthesized into estrone, and the testosterone makes estradiol, both of which are estrogens. Finally, testosterone also makes dihydrotestosterone (DHT).
As you can see, there are common roots to these steroids, linking them in more than one way. This means that a dysfunction in the synthesis at any point could cause downstream disruptions. This is why, for example, low testosterone is a problem in women just as much as it is in men, thanks to how it also affects estrogen production. And progesterone is not just a female hormone, it affects the holistic hormone balance in men as well.
Insulin is not part of the above network of steroids, although it can affect all of them through its downstream actions. It is made by pancreatic beta cells in the pancreas. Its precursor molecules are preproinsulin and proinsulin. Your pancreas is part of the Bioenergetics Circuit, which is the circuit that deals with energy and metabolism.
Insulin is the hormone that takes the glucose that’s been released into your bloodstream through digestion and transports it to your cells. Inside the cells, that glucose is used by the mitochondria to create ATP, the energy currency of life.
Without insulin, the glucose will remain in the bloodstream, and your cells will be deprived of the energy they need to carry on their biochemical processes. High blood glucose levels are also dangerous for your health.
An issue that is quite common, yet frequently overlooked, is insulin resistance. Insulin resistance is when your cells resist the insulin and don’t allow the glucose it is carrying to enter. As you can imagine, this leads to high blood glucose levels, called hyperglycemia, as well as less ATP creation. But it also can cause your pancreas to release more and more insulin, a state called hyperinsulinemia.
A very interesting sign of hyperinsulinemia is acanthosis nigricans, which is the appearance of a velvety plaque of hyperpigmentation on the skin. Usually around the neck, elbows, groin, and hands. Another sign is the android body type, with a thick chest and abdomen.
Hyperglycemia and hyperinsulinemia are huge stressors on the body. They lead to blood sugar spikes and crashes, where the flooding of insulin throughout the body will cause a sudden drop in blood sugar levels, a state called hypoglycemia.
This will create symptoms such as anxiety, shakiness, lightheadedness, and even fainting. It will also make you crave sweets. Consuming these sweets will then spike blood glucose once more, and insulin resistance will lead to more hyperglycemia, causing the pancreas to then flood the body with more insulin again, leading to hyperinsulinemia.
 Because insulin resistance is a stressor, it can raise your cortisol levels to deal with that stress. And chronically elevated cortisol will lead to more insulin resistance. In some cases, the elevated cortisol came first due to other stressors, but brought about insulin resistance in tow.
Because insulin resistance is a stressor, it can raise your cortisol levels to deal with that stress. And chronically elevated cortisol will lead to more insulin resistance. In some cases, the elevated cortisol came first due to other stressors, but brought about insulin resistance in tow.
Insulin resistance also has an effect on other hormones. For example, it stimulates the synthesis of more DHEA, which increases testosterone levels. It also affects your hepatocytes, or liver cells, which leads to a decrease in the production of sex hormone-binding globulin (SHBG). The little SHBG left will also preferentially bind to the increased testosterone, and all of that will result in an increase in free estrogen in the body.
Insulin resistance is associated with many conditions, including:
As mentioned, the adrenal glands are part of the NEM’s Hormone Circuit. They make over 50 different hormones, including your body’s most powerful stress hormones: cortisol, adrenaline, and norepinephrine.
Your adrenals are part of your hypothalamic-pituitary-adrenal (HPA) axis. The hypothalamus and pituitary gland are the control center in the brain. When the hypothalamus senses that stress is present, it sends corticotropin-releasing hormone (CRH) to the pituitary gland to tell it to release adrenocorticotropic hormone (ACTH) to stimulate the adrenal glands. The adrenals then release cortisol to deal with the stressor. Any leftover cortisol then acts as a signal to the hypothalamus to stop the cycle, acting as a kind of feedback mechanism.
Cortisol, which is a glucocorticoid, is especially important here because of how much it affects all the other hormones.
When you’re healthy, your cortisol naturally rises and falls throughout the day, but it doesn’t go above or below certain levels. Some of its main roles include blood pressure and blood glucose regulation, maintenance of heart and blood vessel function, neutralizing inflammation, and suppressing the immune system.
When you’re faced with a stressor, it rises in order to make you more alert. It’s involved in your “fight or flight” response, which helps your heart pump more oxygenated blood to your muscles, triggers the release of stored glucose to give your muscles and brain more fuel, and makes you more alert. But then, once the threat has passed, it should go back to baseline levels again and allow your body to enter a more relaxed state.
The problem occurs when your stress is chronic. Then your adrenals have to overwork to produce more and more cortisol. Eventually, when they become exhausted and the stress continues, their cortisol output drops completely. These are all phases of Adrenal Fatigue Syndrome (AFS).
Symptoms of AFS include fatigue, weight gain, sleep disturbances, brain fog, anxiety, mild depression, hair loss, dry skin, loss of libido, PMS, infertility, estrogen dominance, hypoglycemia, salt and sugar cravings, unstable blood pressure, heart palpitations, lowered immunity, food and drug sensitivities, central obesity, thyroid dysfunction, gastrointestinal issues, osteoporosis, and an inability to handle or recover from stress.
 Some people also suffer from stress-related health issues more than others. Some people have a genetic predisposition to remain in the sympathetic dominant state. This is the branch of your autonomic nervous system (ANS) that provides the stress response, whereas the parasympathetic branch of your ANS is the one that allows your body to calm down and digest.
Some people also suffer from stress-related health issues more than others. Some people have a genetic predisposition to remain in the sympathetic dominant state. This is the branch of your autonomic nervous system (ANS) that provides the stress response, whereas the parasympathetic branch of your ANS is the one that allows your body to calm down and digest.
How fast the shift from sympathetic to parasympathetic ANS goes is also a key difference between us and other animals.
Non-human animals can return to the parasympathetic state relatively quickly after facing a threat, including a life-threatening one. On the other hand, we spend a lot more time in the sympathetic state than we should. With our modern lives, we are less likely to face survival situations, yet are constantly battling chronic stressors.
And although we are extremely adaptable creatures, that is not the same thing as being healthy. You cannot go through life constantly adapting to chronic stress without accumulating some damage, such as AFS, insulin resistance, and thyroid dysfunction.
Like the adrenal glands, your thyroid works as part of an axis using the same control center in the brain: the hypothalamic-pituitary-thyroid (HPT) axis. The hypothalamus sends thyroid-releasing hormone (TRH) to the pituitary gland to make it release thyroid-stimulating hormone (TSH). TSH is the hormone that stimulates your thyroid into making thyroid hormones T3 and T4.
T3 is the active hormone needed for cells’ metabolism and the Bioenergetics Circuit to function properly. Your thyroid gland only makes a small percentage of your active T3. The majority needs to be converted from T4 by your liver and kidneys.
Elevated cortisol levels will decrease the release of TSH, as well as the conversion of T4 into active T3. At the same time, it will increase the conversion of T4 to reverse T3, which is an inactive form of T3.
Also, like insulin resistance, high cortisol levels will affect your liver as well. It will also inhibit its ability to remove excess estrogen from your blood. Increased levels of free estrogen will increase your levels of thyroid-binding globulin, which binds to your thyroid hormones, rendering them inactive.
Your thyroid hormones regulate your basal metabolic rate, which is the rate at which your body utilizes energy to stay alive, functioning, and warm. These hormones are crucial to the mitochondria’s ability to produce ATP. Low levels of thyroid function and thyroid hormones can lead to hypothyroidism, and it is a very common condition. It affects more women than men, especially those going through big hormonal shifts. It’s also common in people with diabetes. Hypothyroidism symptoms include:
Hyperthyroidism, on the other hand, is when your thyroid is overactive, and its symptoms can include:
Thyroid dysfunction is usually evaluated with lab tests. They check your TSH levels, and if they’re low, it means that your thyroid is working well, since it doesn’t need more stimulation. If the levels are high, it shows that your HPT axis is trying to push your thyroid to produce more hormones, which means your thyroid gland is not functioning properly.
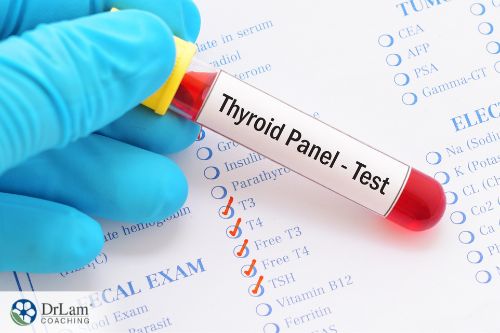 However, we like to test for free T3 and T4 levels as well, along with other important diagnostics. Some possible other lab tests include checking for anti-thyroid antibodies, like anti-thyroglobulin, anti-peroxidase, and anti-TSH receptor antibodies. High LDL cholesterol, homocysteine, and cortisol levels are also associated with thyroid dysfunction, so we sometimes look at those as well. Finally, some micronutrients important for T4 to T3 conversion are iodine, selenium, iron, potassium, and zinc. We check for many nutrient deficiencies in our nutritional evaluation as well.
However, we like to test for free T3 and T4 levels as well, along with other important diagnostics. Some possible other lab tests include checking for anti-thyroid antibodies, like anti-thyroglobulin, anti-peroxidase, and anti-TSH receptor antibodies. High LDL cholesterol, homocysteine, and cortisol levels are also associated with thyroid dysfunction, so we sometimes look at those as well. Finally, some micronutrients important for T4 to T3 conversion are iodine, selenium, iron, potassium, and zinc. We check for many nutrient deficiencies in our nutritional evaluation as well.
If you are getting lab tests done via a conventional medical route, you should be aware that most doctors use a reference range rather than the optimal range of values for hormone levels and other laboratory tests. You should aim for optimal levels.
Although sex hormones have many functions, their main effect is on your reproductive health. That includes things like the health of your reproductive organs as well as libido, menstruation, fertility, and even appearance.
Men have female sex hormones, like estrogen and progesterone, and women have male sex hormones, like testosterone. What’s different are the concentrations of these hormones in each gender and even in each person. Also, what’s important to note here is that it’s not just about the absolute levels of these hormones in your system, but their relative levels and how they balance each other out.
In women, estrogen and progesterone have to work against each other. And that’s not a bad thing; each one keeps the other in check in order to maintain a balance. This balance is vital for a woman’s menstrual cycle, reproductive health, energy levels, mental health, mood, and weight. In men, the balance is between testosterone and estrogen.
Although your cycle might be slightly different from someone else’s, there is a healthy pattern to aim for through the three main phases of the menstrual cycle:
Perimenopause disrupts this cycle. Your FSH and estrogen levels rise and fall over weeks or months, rather than days, and your progesterone curve flattens. Menopause is when your menstrual cycle stops completely.
A very common and challenging hormone imbalance we see with our clients is estrogen dominance. As mentioned, AFS can lead to estrogen dominance. But estrogen dominance can also cause AFS, since it’s a big stressor on the body.
In women, this imbalance happens when you get a relative dominance of estrogen over progesterone, rather than an absolute increase in estrogen.
 Many factors can cause estrogen dominance, including all the hormone imbalance triggers mentioned above. But, one specific thing to look out for is exposure to xenoestrogens. These are synthetic chemicals that are molecularly similar to estrogen and can mimic its action. They can be found in things like perfume, beauty products, and pesticides.
Many factors can cause estrogen dominance, including all the hormone imbalance triggers mentioned above. But, one specific thing to look out for is exposure to xenoestrogens. These are synthetic chemicals that are molecularly similar to estrogen and can mimic its action. They can be found in things like perfume, beauty products, and pesticides.
Also, with aging, both estrogen and progesterone decrease, but not at the same rate. As we saw with perimenopause, progesterone decreases faster, so estrogen becomes more dominant in the system. At least for a while.
Symptoms of estrogen dominance include:
In men, testosterone regulates libido, fat distribution, bone mass, the production of sperm, muscle mass, muscle strength, and the production of red blood cells. Men can also get estrogen dominance, but in this case, it’s the relative dominance of estrogen over testosterone. Its symptoms include loss of libido, infertility, breast enlargement, and sexual dysfunction.
Women can also experience the consequences of testosterone imbalance – either too little or too much testosterone. Symptoms of low testosterone include loss of libido, reduced muscle mass, and a decrease in bone density. Symptoms of high testosterone in women include acne, excess body hair, aggressive attitude, increased risk of diabetes, and polycystic ovarian syndrome (PCOS). High testosterone levels can also make breast cancer more difficult to overcome.
If you suspect you have any of these issues, or if you’re having issues with insulin, thyroid, or cortisol, you might want to get your sex hormone levels tested. Get your progesterone, DHEA, pregnenolone, estrone, estradiol, estriol, SHBG, and testosterone checked as part of your holistic hormone balance recovery plan.
There are some genetic predispositions that can make it more difficult for your body to metabolize and detoxify certain hormones.
There are three pathways of estrogen metabolism: the 2-OHE1, the 4-OHE1, and the 16alpha-OHE1.
The CYP1B1 gene regulates the production of the cytochrome P450 1B1 enzyme, which is the enzyme that helps break down certain substances, including estrogen and some types of drugs, as well as produce certain types of lipids. The gene is present in tissues of the uterus, ovaries, and prostate gland. And it can give rise to hormone-related cancers.
Although generally genes play a much lesser role in your health than your diet and lifestyle, we do sometimes propose genetic testing as part of our Lam Clinic functional lab tests to make sure our health plans are suited to any inherited conditions.
For most hormone imbalances, it's best to look into diet and lifestyle changes first. For example, in some cases, you can reverse thyroid dysfunction when you improve adrenal fatigue or insulin resistance. Then, you don’t need to take thyroid hormones. Also, if you have certain nutritional deficiencies, the best solution is to change your diet and take good-quality supplements.
But sometimes, the hormone imbalance is just part of the aging process and there are no natural approaches that could reverse that. For example, this is the case for menopause in women and testosterone decline in older men. Of course, having a healthy diet and lifestyle can improve the symptoms of these conditions. But if you want to regain a holistic hormone balance, you may want to consider taking some HRT.
 However, before you start HRT you need to know that certain types of HRT can increase hormone-related cancer risk, while others can actually decrease those risks. That’s why it’s imperative that you know the difference and that you discuss these things with your healthcare provider.
However, before you start HRT you need to know that certain types of HRT can increase hormone-related cancer risk, while others can actually decrease those risks. That’s why it’s imperative that you know the difference and that you discuss these things with your healthcare provider.
For example, a French study of over 54,000 post-menopausal women on different types of HRT provided some interesting results. The group that took oral or transdermal estrogens in combination with oral micronized progesterone had little to no increase in breast cancer risk. On the other hand, those that took either type of estrogen but with a synthetic progestin had a significantly higher increase in breast cancer risk.
This shows that the type of progesterone used is key. Natural progesterone is protective, while synthetic progestin is not. Also, it’s important that the HRT consists of a combination of estrogen and progesterone, rather than just estrogen alone. As noted in the estrogen dominance section above, estrogen and progesterone balance each other. Maintaining this balance is something you want to address when taking HRT as well.
Overall, properly done HRT reduces coronary artery disease and all-cause mortality in post-menopausal women. This is why we offer many of our clients bioidentical HRT as part of our holistic hormone balance approach.
In order to cover all your bases, there are five main steps you should take in a holistic hormone balance strategy. They are:
You may need support and guidance to implement these strategies correctly. Especially when it comes to supplements and AFS. The right kind of support can help you avoid many pitfalls, including paradoxical reactions and adrenal crashes.
 Holistic hormone balance is about looking at each hormone as part of a network. Your hormones work together and affect each other. So, a disruption in one can lead to imbalances in all the rest. As we’ve seen, insulin resistance can cause thyroid dysfunction and AFS, which can then lead to estrogen dominance as well. This is just one way it can play out.
Holistic hormone balance is about looking at each hormone as part of a network. Your hormones work together and affect each other. So, a disruption in one can lead to imbalances in all the rest. As we’ve seen, insulin resistance can cause thyroid dysfunction and AFS, which can then lead to estrogen dominance as well. This is just one way it can play out.
An integrated approach to hormone balance will look at all the possible triggers of imbalances as well as your medical history, diet, lifestyle, biographical information, and any genetic predispositions. Then, your healthcare professional will devise a recovery plan that suits your specific needs and goals. It may or may not include HRT.
If you’d like to know more about our holistic hormone balance recovery plans or our bioidentical hormone replacement therapy, you can call us at +1 (626) 571-1234 for a free initial consultation. Our expert coaches would be happy to talk to you.
Holistic hormone balance requires an integrated approach to four key areas: your insulin and blood glucose levels, your thyroid function and metabolism, your adrenal hormones and stress response, and your sex hormone balance. Learn about whether hormone replacement therapy is a good option for you.
