
Everyone experiences rapid heartbeat or tachycardia symptoms on occasion. When you exercise, you want your heart rate to increase. Likewise, when you’re frightened, under stress, when you experience trauma, and when you’re ill, your heart rate increases. However, tachycardia occurs when you experience a heart rate of over 100 beats per minute when you shouldn't. This condition can have serious consequences and requires a visit to your doctor.
» Read our complete long-read article on tachycardia symptoms and Adrenal Fatigue Syndrome
» Adrenal Fatigue FAQs
» Take our 3-minute test to see if you may have Adrenal Fatigue
Tachycardia describes a heart rate that exceeds normal. Typically, healthcare professionals consider a heart rate above 100 beats per minute to fall into the tachycardia range.
Some of the time, tachycardia symptoms or complications may not appear. However, if it continues without treatment, severe consequences can result. These consequences include:
 To understand how tachycardia works, it's important to understand your heart’s electrical system.
To understand how tachycardia works, it's important to understand your heart’s electrical system.
Your heart consists of four chambers, two upper chambers (atria) and two lower chambers (ventricles). Normally, a natural pacemaker called the sinus node in the right atrium controls your heartbeat. This sinus node utilizes an electrical impulse to start each of your heartbeats.
These electrical impulses go across your atria causing the muscles there to contract to pump blood into the ventricles. From there, the impulses reach the atrioventricular (AV) node, typically the only path for them to follow to travel to the ventricles.
The AV node slows down the electrical signal to give the ventricles enough time to fill with blood. Once the ventricles become filled with blood, the electrical signal stimulates the ventricles to contract, forcing blood to the lungs or other parts of the body.
But if anything disrupts the electrical signal in this complex system, tachycardia, bradycardia (slow heartbeat) or irregular heartbeat can occur.
Researchers and clinicians delineate several types of tachycardia. All of them involve some disruption of the electrical signal that works to keep your heart rate normal.
Atrial fibrillation describes a rapid heart rate brought on by chaotic and irregular impulses in the atria. As a result, you experience rapid, weak, and uncoordinated atrial contractions. The most common type of tachycardia, atrial fibrillation may occur temporarily. On the other hand, some episodes will not stop without treatment.
Your heart’s atria beat at a regular rate normally, but begin moving very fast in atrial flutter. As a result of this fast rate, you experience weak contractions of the atria. Irregular circuitry in the atria causes this flutter. Episodes may go away spontaneously, or they may require treatment. People who suffer from atrial flutter also may experience atrial fibrillation at times.
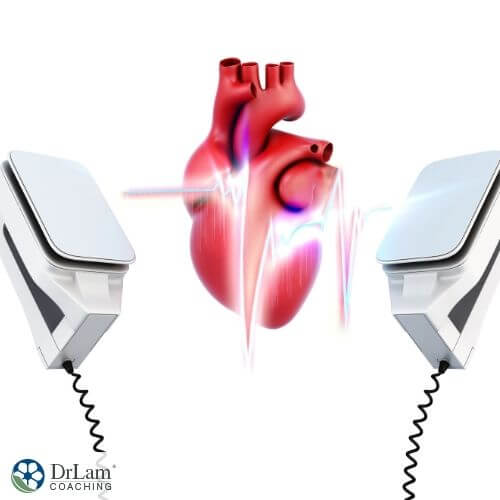
This type of tachycardia occurs when rapid and chaotic electrical impulses cause the ventricles of your heart to quiver rather than contract normally. Therefore, not enough blood gets pumped out of the ventricles to the rest of the body. As a result, this type of tachycardia can become deadly if an electric shock to the heart doesn’t occur within minutes. Ventricular fibrillation can occur during or after a heart attack or because of severe physical trauma such as being struck by lightning.
This type of tachycardia begins in the atria of your heart where the electrical signals fire abnormally. Therefore, they interfere with the electrical impulses coming from your body’s natural pacemaker, the sinoatrial node. As a result, your heart beats faster than normal. This leads to the chambers of your heart not filling with blood properly and not pumping blood adequately to your body.
And two other forms of this type of tachycardia include paroxysmal atrial tachycardia (PAT) and paroxysmal ventricular tachycardia (PVT).
Those who will most likely experience this type of tachycardia include:
SVT does not typically occur with heart attack or mitral valve problems.
This type of tachycardia describes a normal increase in your heart rate. In it, your sinoatrial node fires faster than normal, but your heart continues to beat normally. This means that sinus tachycardia is essentially a normal reaction to some conditions, such as:
Less common causes of this type of tachycardia include:
This type of tachycardia begins in the lower chambers, ventricles, of your heart. You may tolerate it well if you have no underlying heart condition. On the other hand, with such an underlying condition the tachycardia may become life-threatening and require immediate medical intervention. And episodes may occur briefly and cause no harm. But episodes lasting for several seconds may become a medical emergency.
This condition interferes with the electrical impulses from the sinoatrial node resulting in a rapid heartbeat. In addition, it prevents the chambers of your heart from filling with blood and pumping sufficient blood to the rest of your body.
Most of the time, this type of tachycardia comes as a result of other disorders interfering with your heart’s electrical system. For example:
 Tachycardia symptoms can vary depending on which type of tachycardia you have. Most of the common symptoms include:
Tachycardia symptoms can vary depending on which type of tachycardia you have. Most of the common symptoms include:
The typical therapy for tachycardia symptoms can range from no therapy to emergency hospitalization. Deciding factors include the strength of symptoms and whether or not you suffer from underlying conditions.
Many people with this type of tachycardia do not require treatment. But if the episodes continue for some time, some kind of medical intervention may prove necessary. These include:
Other interventions require lifestyle changes to help slow your heart rate. For example:
However, if you suffer from Wolff-Parkinson-White Syndrome, you may need medications or ablation to control paroxysmal supraventricular tachycardia symptoms.
Most of the time, sinus tachycardia symptoms will not need medical intervention. However, if they persist, you should consult your healthcare professional. He or she should consider not just managing the symptoms, but investigating whether you may suffer from an underlying more serious condition.
The causes of ventricular tachycardia symptoms are essential in deciding on the appropriate remediation efforts. These may include:
 As with any health condition, tachycardia brings with it some potential complications. These complications depend on the type of tachycardia you experience, how long your rapid heartbeat lasts, how fast your heart beats, and any underlying heart condition you may suffer from.
As with any health condition, tachycardia brings with it some potential complications. These complications depend on the type of tachycardia you experience, how long your rapid heartbeat lasts, how fast your heart beats, and any underlying heart condition you may suffer from.
Possible complications include:
As with many illness conditions, a family history of tachycardia will increase your risk of developing the condition. In addition, any other condition that puts a strain on your heart or that may damage heart tissue can increase your risk. For example, these conditions include:
Chronic stress is a common condition, but it can lead to a condition known as Adrenal Fatigue Syndrome (AFS), resulting from fatigued adrenal glands. This condition also increases the risk of developing tachycardia and potential complications increases.
AFS begins when chronic stress depletes your adrenal glands’ ability to produce sufficient cortisol to fight the effects of stress. This condition develops over time, beginning as subclinical symptoms and eventually developing into a debilitating condition.
The NeuroEndoMetabolic (NEM) stress response is another natural mechanism that your body uses to deal with stress and to attempt to maintain homeostasis. The NEM consists of six inter-related circuits with three organs or systems in each circuit. What affects one of these circuits also affects others due to the inter-related nature of the circuits. And when one of the circuits becomes dysregulated due to chronic stress, others will also become dysregulated, generating sometimes significant symptoms, including severe tachycardia.
 The Cardionomic circuit of the NEM is the most involved in tachycardia symptoms. This circuit consists of the cardiovascular system, the autonomic nervous system, and the adrenal glands.
The Cardionomic circuit of the NEM is the most involved in tachycardia symptoms. This circuit consists of the cardiovascular system, the autonomic nervous system, and the adrenal glands.
Your autonomic nervous system controls involuntary functions of your body including heart rate, blood pressure, and the fight or flight response to stress. Neurotransmitters and hormones such as acetylcholine, dopamine, norepinephrine, and epinephrine (adrenaline) work to regulate the autonomic nervous system. Any condition affecting the autonomic nervous system is called dysautonomia.
POTS, or postural orthostatic tachycardia syndrome, is one type of dysautonomia that involves low blood pressure and fast heart rate when standing. When you lie down, around 25% of your blood pools in your chest cavity. So, if you stand up, a significant amount of that blood is pulled to the lower part of your body by gravity. Therefore, in order to prevent fainting and to assure sufficient blood to your brain, the sympathetic nervous system, one aspect of the autonomic nervous system, activates and releases norepinephrine into your bloodstream. It quickly reaches your heart and peripheral blood vessels, narrowing them and increasing your heart rate. As a result, more blood flow to your brain prevents fainting.
Without norepinephrine, you could not remain in an upright position for day-to-day living. A lot of the POTS and tachycardia symptoms come from an inability to move blood quickly to the brain.
When you come under stress from any source, your body releases cortisol, norepinephrine, and epinephrine to deal with it. But under ordinary circumstances, once the stress diminishes and your body returns to normal, the levels of these hormones also return to normal.
However, if stress continues and becomes chronic, more and more norepinephrine floods your system. Sympathetic overtone occurs in a body chronically flooded with norepinephrine. As a result, your brain remains continually on high alert and your heart remains ready to run from stressors or fight them. People who suffer from advanced AFS live continually in a state of alarm as a result of this response to stress.
This leaves your cardiovascular system at risk for POTS and tachycardia symptoms.
Another of the neurotransmitters/hormones affecting the autonomic nervous system is epinephrine. This very powerful biochemical plays a minimal role in everyday life, but when stress becomes severe and chronic, its role increases. Your body’s last response to stress, epinephrine comes from the fight or flight response. Above all, its role is to supply blood to your brain and muscles so you can survive.
If epinephrine continues to flood your system, significant symptoms can develop. Your heart rate will rise significantly due to the nodes supplying electrical impulses to your heart being bathed in epinephrine. They can become overstimulated and ultimately damaged.
This may result in several conditions that occur due to an irregular heartbeat. For example:
In addition, an excessive heart rate leads to increased reactive metabolites at a cellular level, which then cause abrasion to the cardiac nodes due to inflammation.
Activation of the sympathetic nervous system in normal people tends to bring about an increase in heart rate by 10-15 beats per minute and a slight increase in blood pressure. This becomes normalized very quickly by an automatic response involving blood vessel dilation.
However, with some people, this mechanism fails and the normalization of blood flow to the heart and brain doesn’t occur. This sets in motion POTS and tachycardia symptoms.
POTS syndrome refers to a collection of symptoms. These symptoms occur throughout your body because the functions of the autonomic nervous system affect all parts of your body. Some of the symptoms of POTS are:
 A number of natural methods for regulating the cardionomic circuit and normalizing many of the tachycardia symptoms can be utilized. For example:
A number of natural methods for regulating the cardionomic circuit and normalizing many of the tachycardia symptoms can be utilized. For example:

There are many different types of tachycardia that can lead to tachycardia symptoms. In general, symptoms can range from hardly any to very severe. Regardless of the intensity of your symptoms, if your tachycardia continues you should consult with your healthcare professional. Continuing tachycardia symptoms may indicate an underlying more serious disorder.
Tachycardia symptoms may also present similar symptoms to those found in AFS. One of the symptoms of advanced AFS is tachycardia. This suggests adrenal issues or imbalances in the Cardionomic circuit of the NEM could be involved.
Disturbances of the Cardionomic circuit of the NEM stress response may also lead to tachycardia in the form of POTS. Addressing your tachycardia symptoms from a natural standpoint with AFS in mind may be of benefit.
If you are suffering from tachycardia symptoms, here are a few things you can do to alleviate the situation.
» Read our complete long-read article on tachycardia symptoms and Adrenal Fatigue Syndrome
» Adrenal Fatigue FAQs
» Take our 3-minute test to see if you may have Adrenal Fatigue
While tachycardia symptoms can be normal at times, there are also times when these symptoms indicate something wrong with your heart and other body systems. Knowing when to seek medical care and when to simply rest is valuable information. And it’s important to know there are natural ways of dealing with these symptoms.
"I'm feeling great on this program"
"Hi Dr. Lam! I'm feeling great on this program so far! Wow, this is amazing!"