 Histamines are chemicals your immune system produces in response to being exposed to some kind of allergen. Some of the most common allergens that do that include pollen, dust, and pet dander.
Histamines are chemicals your immune system produces in response to being exposed to some kind of allergen. Some of the most common allergens that do that include pollen, dust, and pet dander.
» Read our complete long-read article on Histamines and Adrenal Fatigue Syndrome
» Adrenal Fatigue FAQs
» Take our 3-minute test to see if you may have Adrenal Fatigue
Histamine helps your body rid itself of the allergen. And not everyone has the same reaction to these allergens. You could be more sensitive to pollen, while someone else may not have that allergy. At the same time, you could be totally fine with your pet, while a visitor might end up with an allergic reaction.
When your body is exposed to something you’re sensitive to, your immune system sends signals to cells in different areas to release histamines. In particular, mast cells, which are part of your immune and neuroimmune system, are the ones that produce the chemical. They can be found in your skin, blood, gut, nose, mouth, and lungs.
Histamine creates inflammation and increases blood flow in the area in contact with the allergen. That’s why you can get a blocked or stuffy nose, for example, when the lining of your nose is given the signal to produce more mucus as a way to get rid of the pollen or cat hair. Histamines released from your skin can make you itch, and histamines released from mast cells in your lungs can make you cough. The increased blood flow to these areas then allows other immune system chemicals to come in and repair the damage done. This is why you take antihistamines to fight allergies. It reduces the histamines and so reduces the symptoms of the allergy.
Histamine intolerance is not the same thing as the allergic reactions that produce histamine described above. It’s more to do with a build-up of the histamines in your body, or your body lacking the ability to break down the histamine.
The enzyme responsible for breaking histamine down is diamine oxidase, or DAO. Some people can have a DAO deficiency, and even if they’re not exposed to a lot of histamines, the little they are exposed to or produce in their body is enough to cause a build-up. DAO deficiency can be due to dysbiosis, leaky gut, inflammatory bowel disease, overconsumption of histamine-rich foods, and certain DAO-blocking medications.
But regardless of the cause, symptoms of histamine intolerance are quite similar to those of seasonal allergies, and they can include:
As you will see later, many of these symptoms are also present when you have adrenal fatigue and its associated inflammation and detoxification problems. But first, let’s discuss how histamine intolerance can be directly linked to your diet.

Diet can increase the levels of histamine in your body in three ways:
For the first group of histamine-rich foods, some of the biggest culprits are fermented and/or aged foods and drinks. They tend to have the highest levels of histamine, and they include:
Along with these, there are other foods that are not necessarily aged or fermented that can also contain high amounts of the chemical and/or trigger your body to produce histamines. They include:
As for substances that can block DAO production, these include:
 Before you worry about having to cut all these foods out for good, there are three things to know.
Before you worry about having to cut all these foods out for good, there are three things to know.
First of all, not everyone has histamine intolerance; your symptoms could be due to something else entirely.
Secondly, histamine intolerance has to do with a build-up of histamine in your body. So, you may not need to cut everything out completely, but just find a way to ensure you don’t cross a certain threshold of quantity or frequency of consumption.
The third thing to understand is that there are certain conditions that can make you temporarily sensitive to certain foods and chemicals. And those include Adrenal Fatigue Syndrome (AFS) and NeuroEndoMetabolic (NEM) Stress Response dysregulation.
AFS is a condition that comes as a result of your body facing chronic stress. That stress can be physical, such as eating a bad diet, getting recurring infections, or being exposed to toxins. Or it can be psychological, such as family problems, financial worries, or a mental health issue. This stress is dealt with first and foremost by your adrenal glands, which produce cortisol, your body’s main anti-stress hormone.
But when your adrenals get overworked, they can dysregulate, causing your cortisol levels to consistently rise or fall outside normal ranges. Usually levels are too high levels at first, then after some time, they drop to very low levels.
Symptoms of AFS include fatigue, food and chemical sensitivities, sleep disturbances, weight gain, anxiety, mild depression, brain fog, lowered immunity, gastrointestinal issues, hypoglycemic episodes, low libido, PMS, infertility, dry or itchy skin, hair loss, heart palpitations, and salt and sugar cravings, among others.
The reason you become more sensitive to certain foods and chemicals when you have AFS is because AFS tends to come with Inflammation and Detoxification Circuit imbalance as well. These circuits are part of your NEM, which is your body’s global response to stress. When your adrenals, which are part of your NEM’s Hormone Circuit, are exhausted, the rest of your NEM has to compensate. And if you don't address the chronic stress, all the other circuits start getting overloaded.
Once your Inflammation Circuit is on overdrive or your Detoxification Circuit is congested, your body becomes much more sensitive to certain substances. That includes histamines. And the more your body becomes sensitive to histamines, the more severe the symptoms and the bigger the stress on your adrenals.
Your Inflammation Circuit is composed of your gut, microbiome, and immune system. And since cortisol dysregulation can cause problems in all of these components, if you have AFS, you will likely have higher inflammation levels in your body. And the reverse is also true. Chronic inflammation is a huge stressor on the body, and it can cause or worsen AFS. So, whichever came first, the cycle repeats until you do something about it.
With histamine-rich foods, for example, what happens is that you likely eat them frequently. You don’t know that you have histamine intolerance, and the symptoms aren’t solely gastrointestinal. So you don’t make that connection. As you eat these foods, however, your gut’s histamine H2 receptors are engaged, and they trigger the secretion of gastric acid. That can create some reflux or worsen peptic ulcers.
All food and chemical sensitivities that originate in the gut can compromise the microbiome. And when the microbiome is out of balance – a state called dysbiosis – you can start getting leaks in the lining of your gut. When these leaks allow substances into your bloodstream that shouldn’t be there, including food particles, pathogens, and toxins, your immune system has to react.
Your immune system, which is the third component of your Inflammation Circuit, creates inflammation in your gut. And if that inflammation isn’t addressed, it can turn chronic and then travel to other areas of your body. Inflammation that reaches the skin can cause skin rashes and itching, inflammation that reaches the brain and nervous system can cause psychiatric and neurological symptoms.
Histamines can also cause inflammation in these areas directly. It doesn’t have to be only through the microbiome and gut. For example, when histamine binds to H1 receptors found in blood vessels, it can cause vasodilation and increased permeability, leading to the redness and swelling we typically associate with visible inflammation.
Still, more often than not, we see that inflammation begins in the gut and it creates a ripe environment for other types of inflammatory responses all over the body. So if you feel like you may have some of the symptoms of histamine intolerance or seasonal allergies, it would be a good idea to get your microbiome and gut checked out.
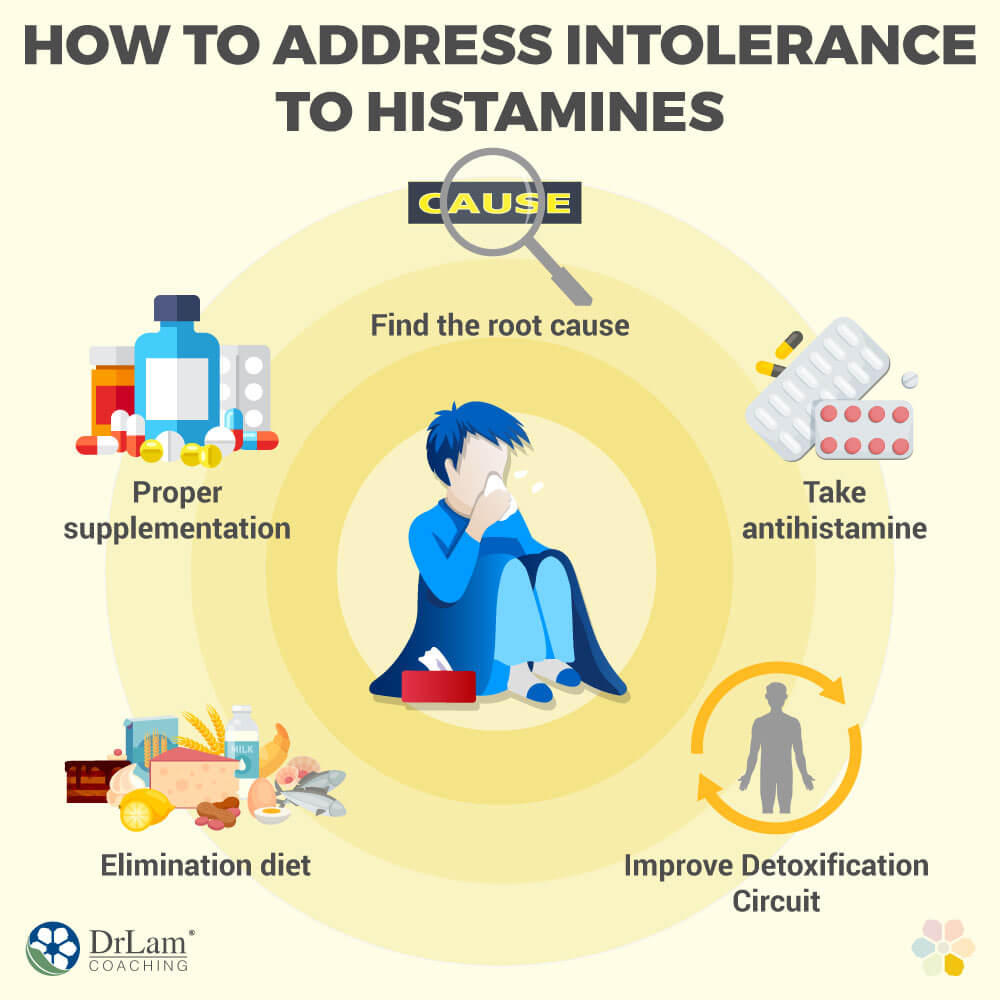
The first and most important step to addressing any health challenge is to actually know the root cause. Unfortunately, with histamine intolerance, your standard lab tests will not help. You might get tested and receive negative results. However, it may still be a good idea to get an allergy test done anyway, in case your symptoms are thanks to an allergy you didn’t know you had.
With seasonal allergies, antihistamine medications can do the trick in most cases. But they come with side-effects and don’t address histamine intolerance. For the intolerance, a DAO supplement might be a better idea, but it also really depends on your situation.
Supplements and medications, even the over the counter types, should still be used with caution. Especially if you have AFS or NEM dysregulation. And that’s because taking supplements can add to your toxic load, especially when your adrenals are weak and your body is already inflamed. You can end up with paradoxical reactions and even adrenal crashes.
That’s why another thing you can do to address histamine intolerance is improve your Detoxification Circuit. Your Detoxification Circuit is composed of your liver, interstitium, and immune system. It’s what helps your body get rid of toxins and metabolic byproducts, including any that result from high levels of histamines.
Improving your detoxification will help lower the inflammation in your body and also improve your adrenal function. And if you combine that with adrenal fatigue recovery, an elimination diet that reduces the histamine load, healing any leaks in your gut through diet and correct supplementation, you can find a lot of relief from histamine intolerance. And you may even be able to slowly add back some of those foods you had to eliminate in the beginning.
Histamines are chemicals your immune system produces when you’re exposed to certain allergens. They can also be found in certain foods. If you have histamine intolerance, a build-up of these histamines, whether from food or as a reaction to allergen exposure, will cause symptoms. These include a stuffy or blocked nose, sinus problems, gastrointestinal issues, sneezing, coughing, headaches, hives, anxiety, tiredness, and brain fog, among others.
Histamine intolerance can cause or aggravate AFS. At the same time AFS can make you more sensitive to histamines and histamine-rich foods. So it’s a good idea to address any adrenal issues you have. And that will also entail ensuring your NEM is in good condition, especially its Inflammation and Detoxification Circuits.
Do your best to address the issue at the root rather than just medicating and treating surface symptoms. In the end, these kinds of temporary solutions will not help you long-term, and may even cause side effects. An elimination diet, supplementation, and adrenal fatigue recovery are your best options for lasting relief. But it's important to make all of these changes under the guidance of an experienced healthcare professional. That will help you avoid some of the common pitfalls that you can encounter along your recovery journey.
» Read our complete long-read article on Histamines and Adrenal Fatigue Syndrome
» Adrenal Fatigue FAQs
» Take our 3-minute test to see if you may have Adrenal Fatigue
Histamines are natural chemicals your body produces in response to allergens. They can also be found in food. If you have histamine intolerance, however, your body can’t process them properly, and you end up with symptoms very similar to those of seasonal allergies. Here’s what to do.
"Thank you for your generous sharing of such valuable resources"
"Dear Dr. Lam,
I am a family practice physician who came across your website when I was searching for information for my 'hypothyroid' patient who wasn't responding to treatment. Your work is extensive, intriguing, and very informative.
Thank you for your generous sharing of such valuable resources. Your work is already changing my understanding of the complexities of this issue."